FEMALE URINARY INCONTINENCE
DR MONA AHMED
FUNCTIONS OF URINARY SYSTEM
The urinary system’s functions include:
- URINE
- FORMATION
- TRANSPORT
- MICTURITION CYCLE
- STORAGE PHASE
- VOIDING PHASE
ANY DEFECT in these functions can lead to URINARY INCONTINENCE.
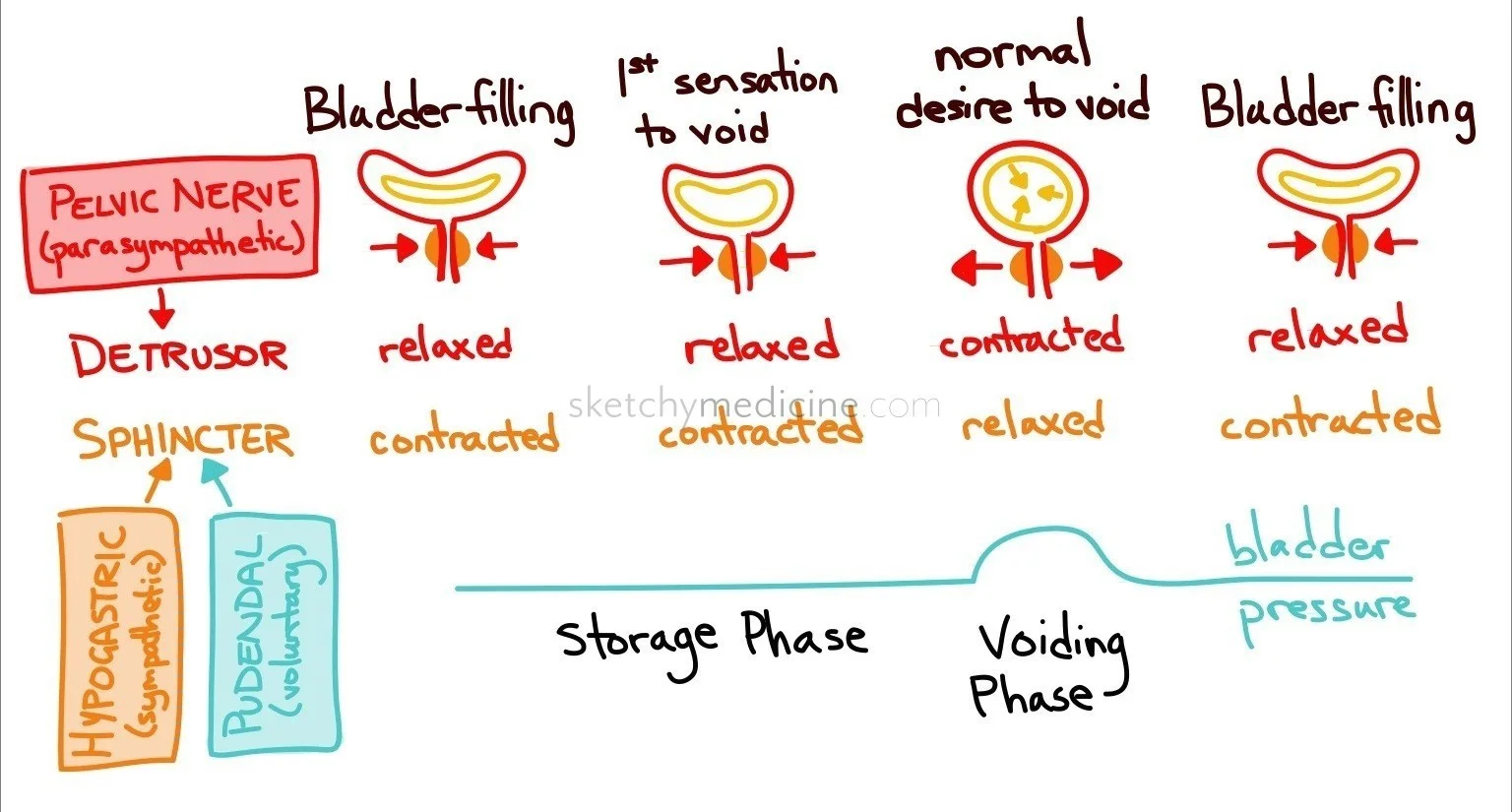
NORMAL MICTURITION CYCLE
URINARY INCONTINENCE
Urinary incontinence is demonstrable and is a social or hygienic problem.
- TYPES
- CONTINUOUS:
- TOTAL
- PARTIAL
- INTERMITTENT:
- STRESS (1ST)
- URGE (2ND)
- MIXED (3RD)
- REFLEX
- OVERFLOW
- NOCTURNAL ENURESIS
- FUNCTIONAL
- VAGINAL ??
- CONTINUOUS:
CONTINUOUS INCONTINENCE (PATIENT IS ALWAYS WET)
| Type | Total | Partial |
|---|---|---|
| Cause | - Vesicovaginal fistula - Bilateral ureterovaginal F | - Unilateral Uterovaginal F - Small, valvular or very high VVF |
| Micturition desire | Absent | Present but less than normal |
| Bladder distention | Absent | May be distended |
INTERMITTENT INCONTINENCE
(URINE PASSES INTERMITTENTLY AND PATIENT IS DRY IN BETWEEN)
INVOLUNTARY LOSS OF URINE: Z
-
STRESS : WHEN IVP EXCEEDS IUP DUE TO ↑IAP BY STRESS.
-
URGE: ASSOCIATED WITH STRONG DESIRE TO VOID DUE TO DETRUSOR INSTABILITY.*
-
REFLEX: DUE TO ABNORMAL REFLEX ACTIVITY IN SPINAL CORD (DUE TO BRAIN TUMOR & SPINAL CORD INJURY) USUALLY ASSOCIATED WITH STRONG DESIRE TO VOID.
-
OVERFLOW : WHEN IVP EXCEEDS IUP DUE TO EXCESSIVE BLADDER DISTENSION.
-
NOCTURNAL ENURESIS : DURING SLEEP E.G. SPINA BIFIDA, SMALL BLADDER CAPACITY, PSYCHOSOMATIC, & CHILDREN.
-
FUNCTIONAL : DUE TO IMMOBILITY OR COGNITIVE IMPAIRMENT HINDER TO GET TO TOILET.
-
MIXED
GENUINE STRESS INCONTINENCE
DEF: INVOLUNTARY LOSS OF A SPURT OF URINE SIMULTANEOUSLY WITH MANOEUVRES THAT INCREASE IAP WHICH ENDS ABRUPTLY WITH END OF ACT
DEGREE OF STRESS INCONTINENCE :
- GRADE I: INCONTINENCE OCCUR ONLY WITH SEVERE STRESS SUCH AS COUGHING, SNEEZING, ETC.
- GRADE II : INCONTINENCE WITH MODERATE STRESS SUCH AS RAPID MOVEMENT OR WALKING UP AND DOWN STAIRS
- GRADE III : INCONTINENCE WITH MILD STRESS, SUCH AS STANDING. THE PATIENT IS CONTINENT IN THE SUPINE POSITION
PATHOPHYSIOLOGY Y
-
AN INTERACTION BETWEEN BLADDER AND SPHINCTER
-
BLADDER ABNORMALITIES :
- -DETRUSSOR OVERACTIVITY (IDIOPATHIC, NEUROGENIC)
- -LOW BLADDER COMPLIANCE
- SCI, INTERSTITIAL CYSTITIS, RADIATION CYSTITIS, HYSTERECTOMY
-
SPHINCTER ABNORMALITIES
- EXTRINSIC : URETHRAL HYPERMOBILITY
- WEAKNESS OF PELVIC FLOOR MUSCLE (URETHRAL SUPPORT)
- INTRINSIC : INTRINSIC SPHINCTER DEFICIENCY (ISD)
- URETHRAL MUSCULATURE, BLOOD FLOW, INNERVATION
- EXTRINSIC : URETHRAL HYPERMOBILITY
AETIOLOGY OF GSI
- CONGENITAL
- TRAUMATIC: - OBSTETRICS - IATROGENIC (OPERATIONS) CAUSING SCARRING AT BLADDER NECK.
- 3P - PREGNANCY - PROLAPSE - POSTMENOPAUSAL
- SHORT URETHRA
- OBESITY
CLINICAL EVALUATION
GENERAL EXAMINATION :
- ABDOMINAL EXAMINATION: DISTENDED BLADDER, ABDOMINAL MASS/OBESITY.
- CHEST EXAMINATION: FOR CHRONIC COUGH.
- PELVIC EXAMINATION:
- INSPECTION:
- ATROPHIC VAGINITIS/ URETHRITIS.
- PELVIC ORGAN PROLAPSE.
- GENITOURINARY
- INSPECTION:
EXAMINATION
- RECTAL EXAMINATION : SKIN IRRITATION, ANAL SPHINCTER CONTROL, FAECAL IMPACTION
- NEUROLOGIC EXAMINATION:
- MENTAL STATUS.
- PERINEAL SENSATION (S2, 3, 4)
- SACRAL REFLEXES ASSESS (S2, 3, 4) CONTROLLING MICTURITION. A} ANAL REFLEX → SCRATCH PERINEUM WITH A PIN.
SPECIAL TESTS
SIGNS: SPECIAL TESTS (AIM, TECHNIQUE, RESULTS)
- STRESS TEST
- PERINEAL PAD TEST
- Q TIP TEST
- WATER BRIDGE TEST
- BLADDER NECK ELEVATION TEST
Q-TIP test

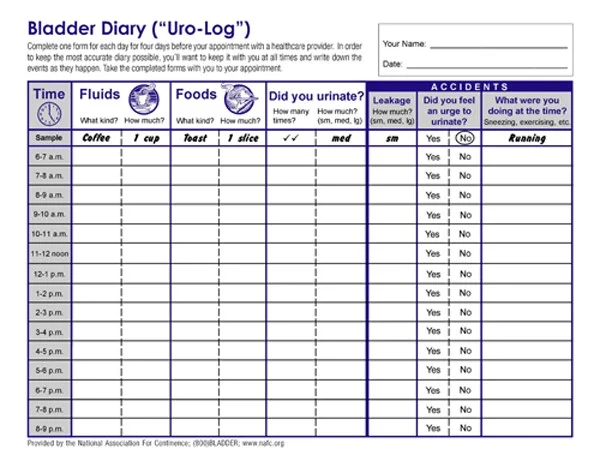
Bladder Diary (“Uro-Log”)
INVESTIGATIONS
- URINE ANALYSIS
- KIDNEY FUNCTION TESTS
- US FOR:
- RESIDUAL URINE
- RENAL SIZE
- BLADDER MASS, NECK AND URETHRAL ANATOMY.
- CYSTOSCOPY
- VOIDING CYSTOURETHROGRAPHY
- URODYNAMIC STUDY
CYTOMETRY
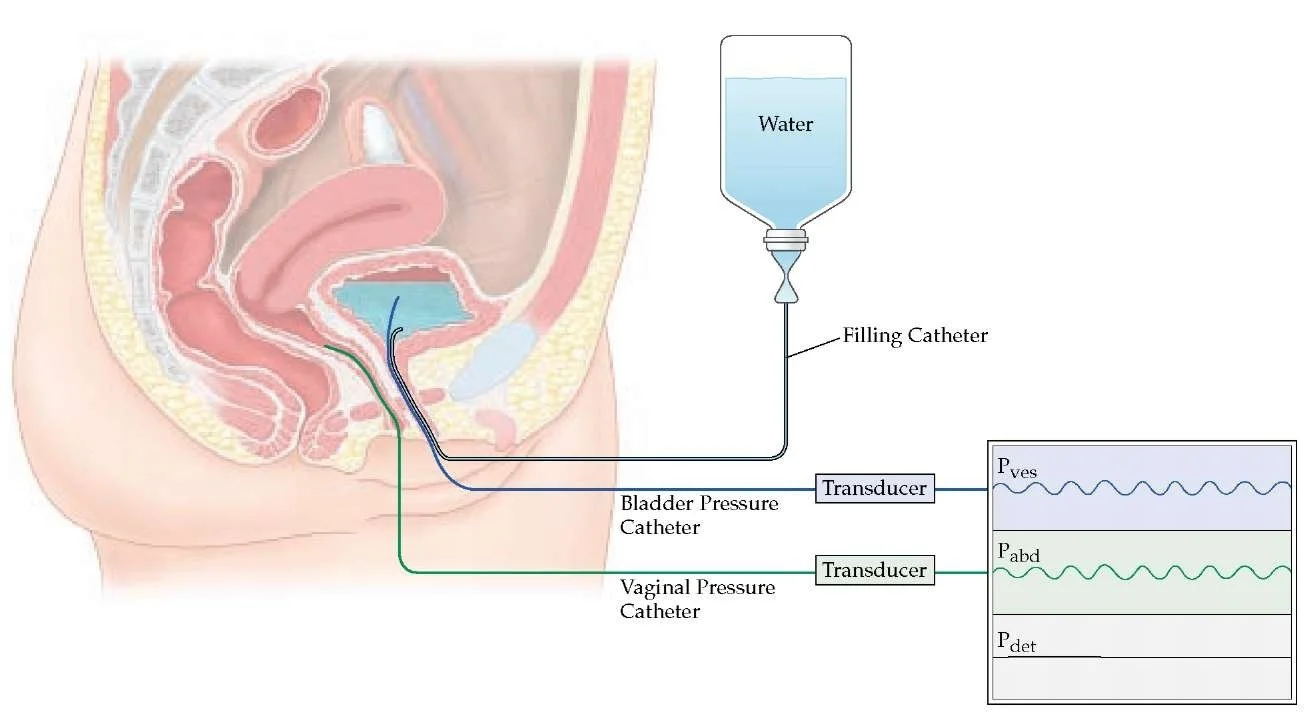
NORMAL CYSTOMETROGRAM

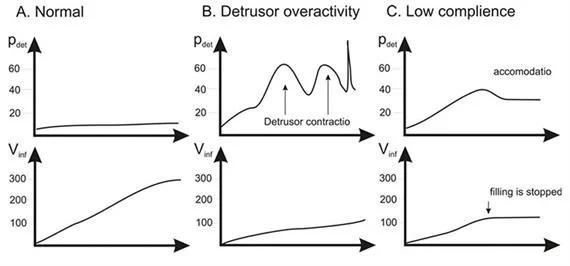
TREATMENT
PROPHYLACTIC:
- TREATMENT OF PREDISPOSING FACTORS.
- GOOD OBSTETRIC CARE
- POSTNATAL PELVIC EXERCISES
- HRT IN POSTMENOPAUSAL WOMEN
- PROPER SURGICAL TECHNIQUE TO AVOID SCARING AT BLADDER NECK.
CONSERVATIVE TREATMENT
LIFE STYLE:
- WEIGHT LOSS
- STOP CAFFEINE & SMOKING
- FLUID MANAGEMENT
MEDICAL:
- ESTROGEN EITHER SYSTEMIC OR LOCAL IN POSTMENOPAUSAL WOMEN.
- ALPHA-ADRENERGIC STIMULANTS
- ANTICHOLINERGICS
PHYSIOTHERAPY:
- PELVIC FLOOR EXERCISES
- FARADIC CURRENT STIMULATION
- MECHANICAL DEVICES: E.G. PESSARY, WEIGHTED CONES USED PREOPERATIVE OR WHEN PATIENT IS UNFIT FOR SURGERY
OTHERS:
- IMPLANTED ARTIFICIAL SPHINCTER
- PARAURETHRAL BULKING AGENTS : COLLAGEN, FAT
SURGICAL TREATMENT
A} VAGINAL URETHROPLASTY : PARAURETHRAL FASCIA ON EITHER SIDE OF BLADDER NECK BY 2-3 SUTURES.
B} ABDOMINAL URETHROCYSTOPEXY: SUTURE THE FRONT OF URINARY BLADDER TO THE BACK OF SYMPHYSIS PUBIS.
C} URETHRAL SLING PROCEDURES
D} MINIMAL INVASIVE SLING LIKE PROCEDURES:
- TENSION FREE VAGINAL TAPE {TVT}
- TRANSOBTURATOR TAPE {TOT}
TREATMENT OF URGE INCONTINENCE
| Non surgical | Surgical |
|---|---|
| 1) Reassurance 2) Physiotherapy 3) Medical treatment: - Antibiotics for infections - Anticholinergics - Tricyclic antidepressants - Antiprostaglandins - Local Estrogen | -Infravesical nerve resection. -Selective bladder denervation. -Cystodistension. Mixed type: treat DI first |
mentoin generally, medical, physical, prophylactic - urinalaysis, indications for urodynamics? Z