Sarcoidosis
DR FAROOQ
Introduction
- Sarcoidosis is a multisystem granulomatous disorder of unknown cause.
- Characterised by non-caseating granulomas in affected organs.
- Most commonly affects lungs, lymph nodes, skin, and eyes.
- Can present acutely or chronically.
Epidemiology
- Worldwide distribution, more common in northern Europe and African Americans.
- Peak incidence: young adults (20–40 years).
- Slight female predominance.
- Genetic and environmental factors.
Pathophysiology
- Granulomatous inflammation with non-caseating granulomas.
- Exaggerated immune response to unknown antigen.
- CD4+ T cells and macrophages play key role.
- Leads to organ damage and fibrosis in chronic cases.
Clinical Manifestations & Features
Pulmonary (>90%)
- Most common site of involvement (~90%).
- Dyspnea, dry cough, chest pain.
- Bilateral hilar lymphadenopathy on chest X-ray.
- May progress to pulmonary fibrosis.
- Pulmonary fibrosis in chronic disease.
It is restrictive lung disease
Cutaneous (25-35%)
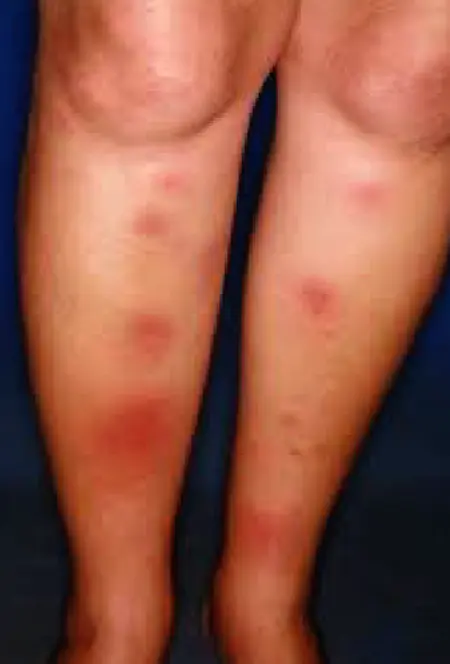
- Erythema nodosum.
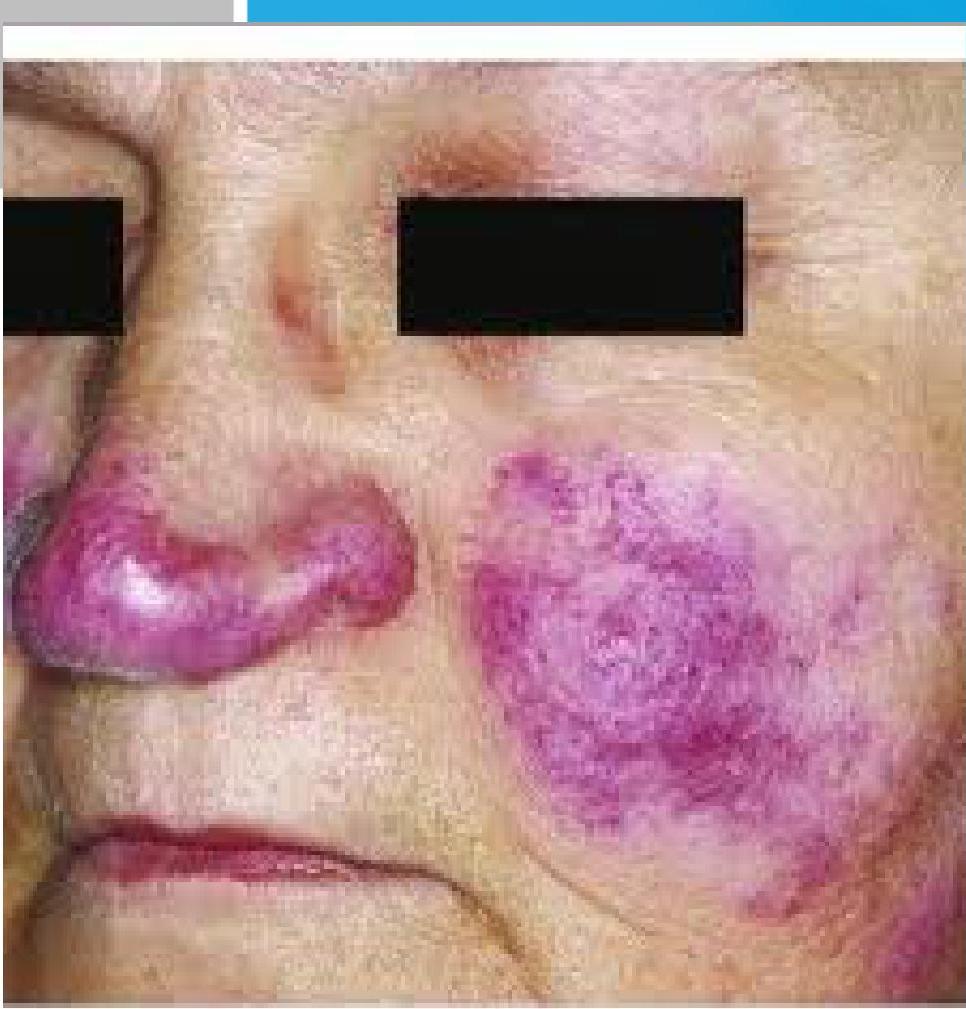
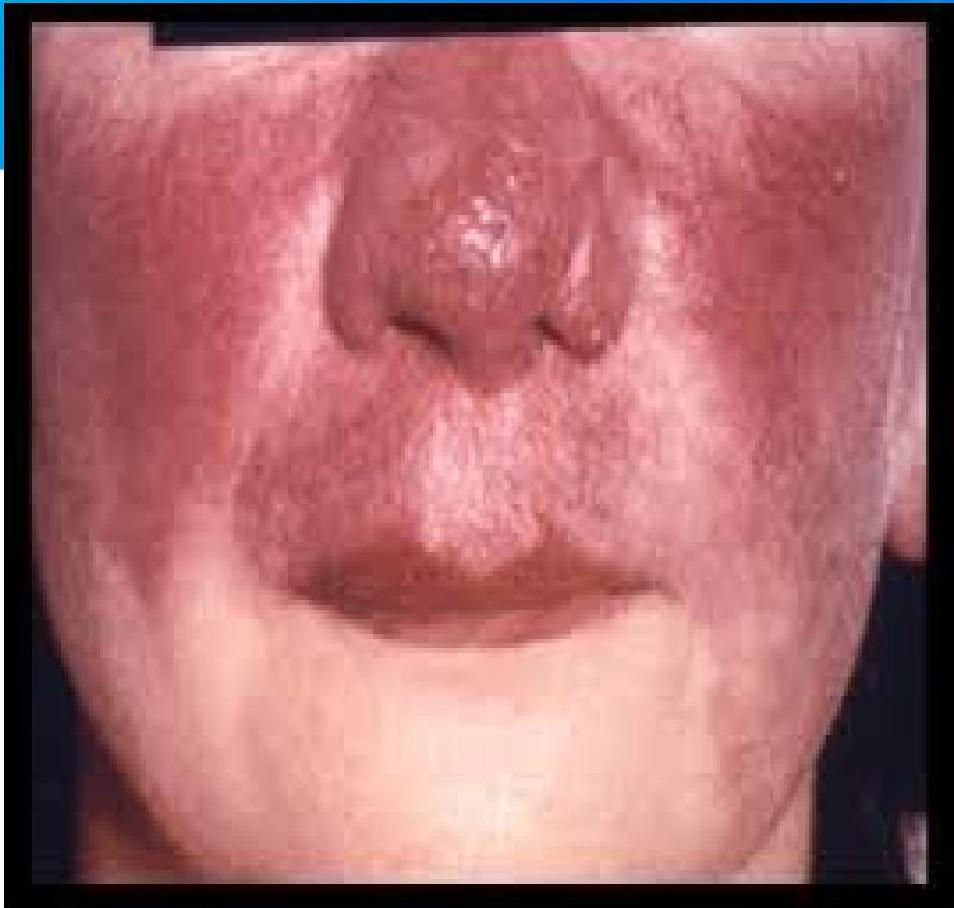
- Lupus pernio.
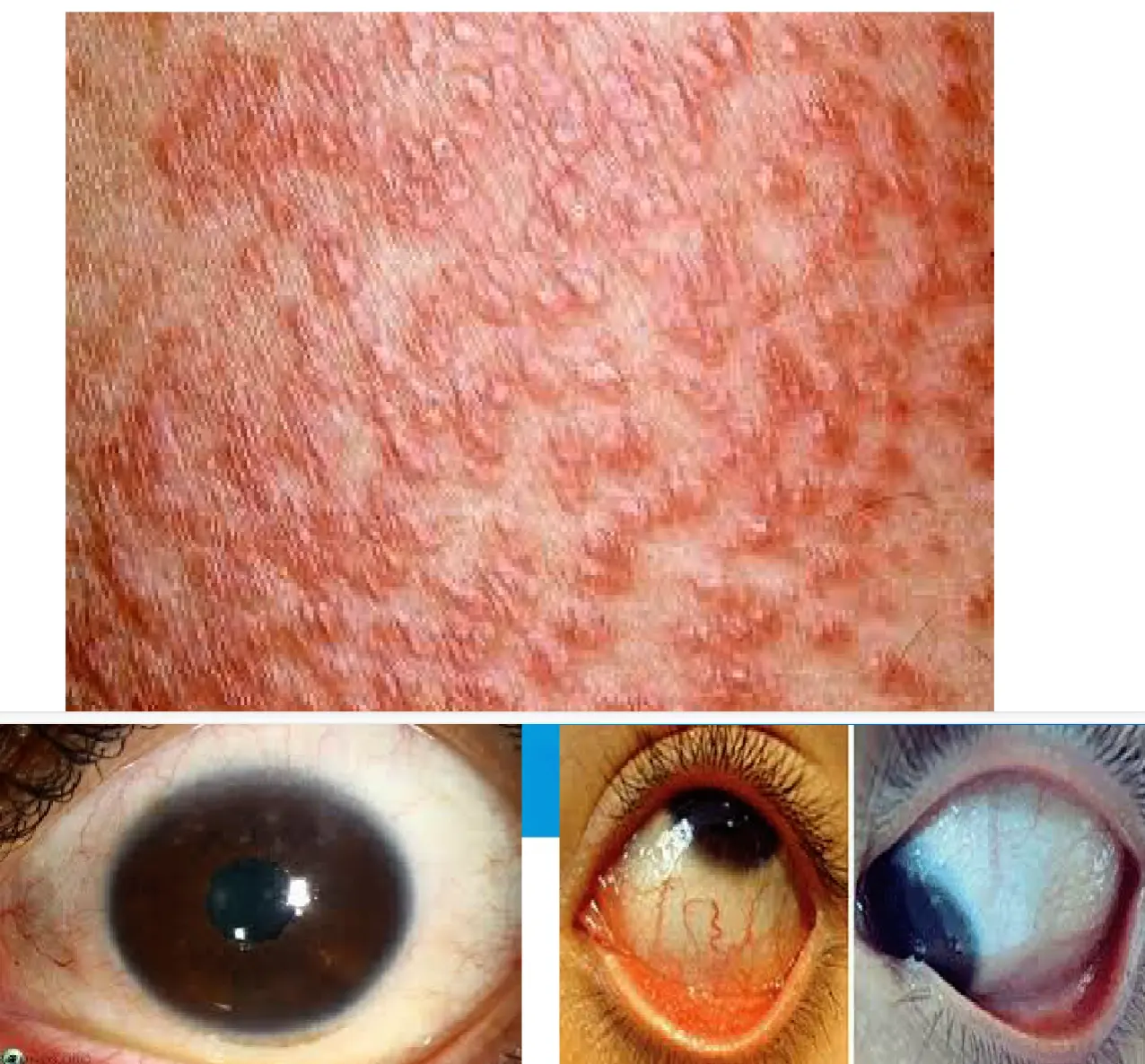
- Maculopapular lesions / maculopapular rash.
Ocular (10-25%)
- Anterior uveitis / uveitis.
- Conjunctival granulomas / conjunctivitis.
- Lacrimal gland enlargement.
- Risk of visual impairment if untreated.
Cardiac (5-10%)
- Conduction defects.
- Cardiomyopathy.
- Arrhythmias.
- Sudden cardiac death.
Neurological (5-10%)
- Cranial nerve palsies (especially facial nerve).
- Peripheral neuropathy.
- Seizures, encephalopathy.
Metabolic (10-15%)
- Hypercalcemia.
- Hypercalciuria.
- Kidney stones, nephropathy.
Hepatic & Splenic
- Hepatosplenomegaly.
Renal
- Hypercalcemia.
- Nephrocalcinosis.
General/Constitutional Symptoms
- Can be asymptomatic (incidental finding on chest X-ray).
- Constitutional symptoms: fever, fatigue, weight loss, night sweats.
- Organ-specific manifestations depend on site of involvement.
Investigations & Diagnosis
Chest X-rayx
- Bilateral hilar lymphadenopathy, interstitial changes.
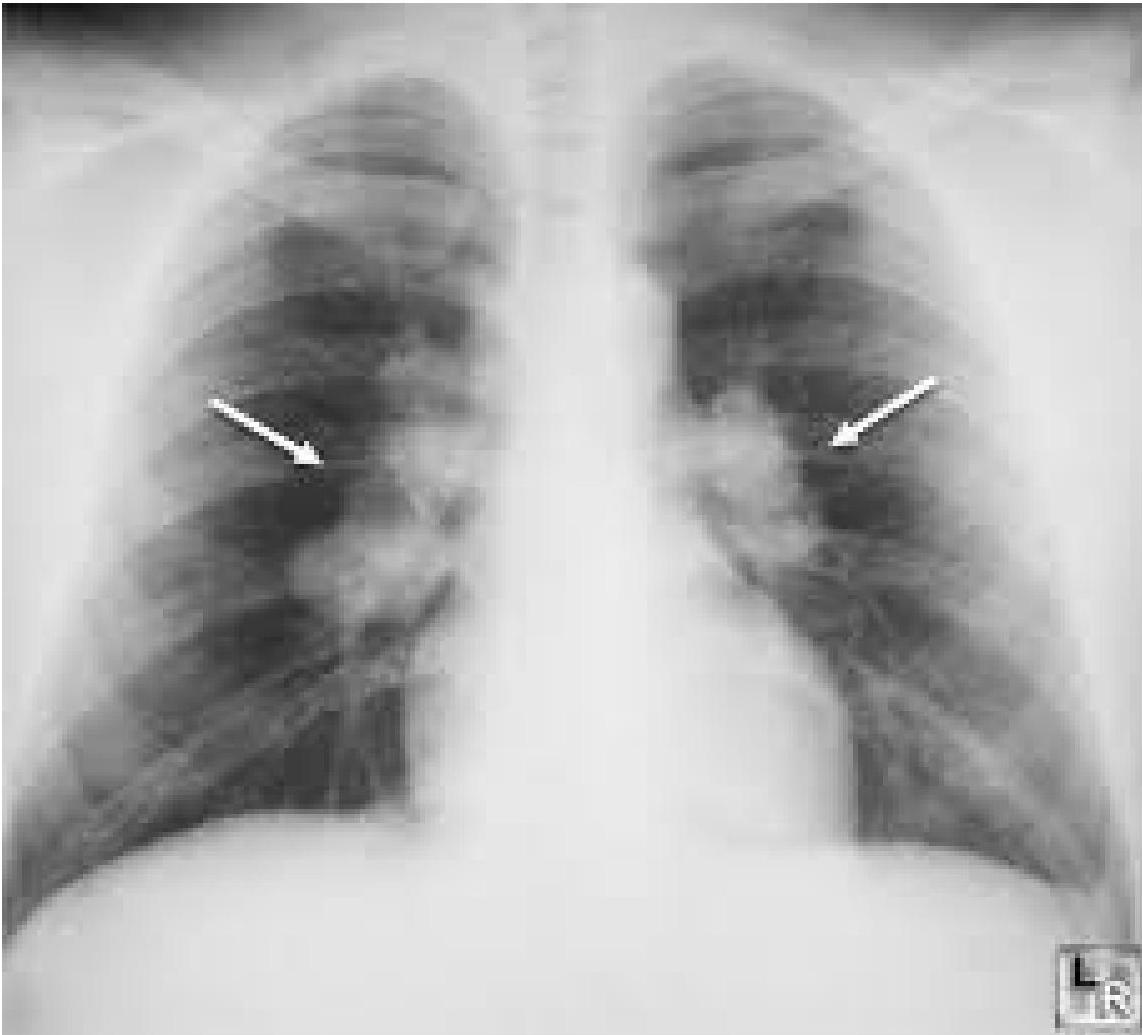
Staging of Sarcoidosis on the Basis of Chest Radiographs
| STAGE | Description | Frequency |
|---|---|---|
| STAGE 0 | No abnormalities | 5%–10% |
| STAGE 1 | Lymphadenopathy (fig. A) | 50% |
| STAGE 2 | Lymphadenopathy + pulmonary infiltration (fig. B) | 25%–30% |
| STAGE 3 | Pulmonary infiltration (fig. C) | 10%–12% |
| STAGE 4 | Fibrosis | 5% (up to 25% during the course of the disease) |
| ![[Sarcoidosis_img-7.jpeg | 227x174]]![[Sarcoidosis_img-8.jpeg | 214x175]]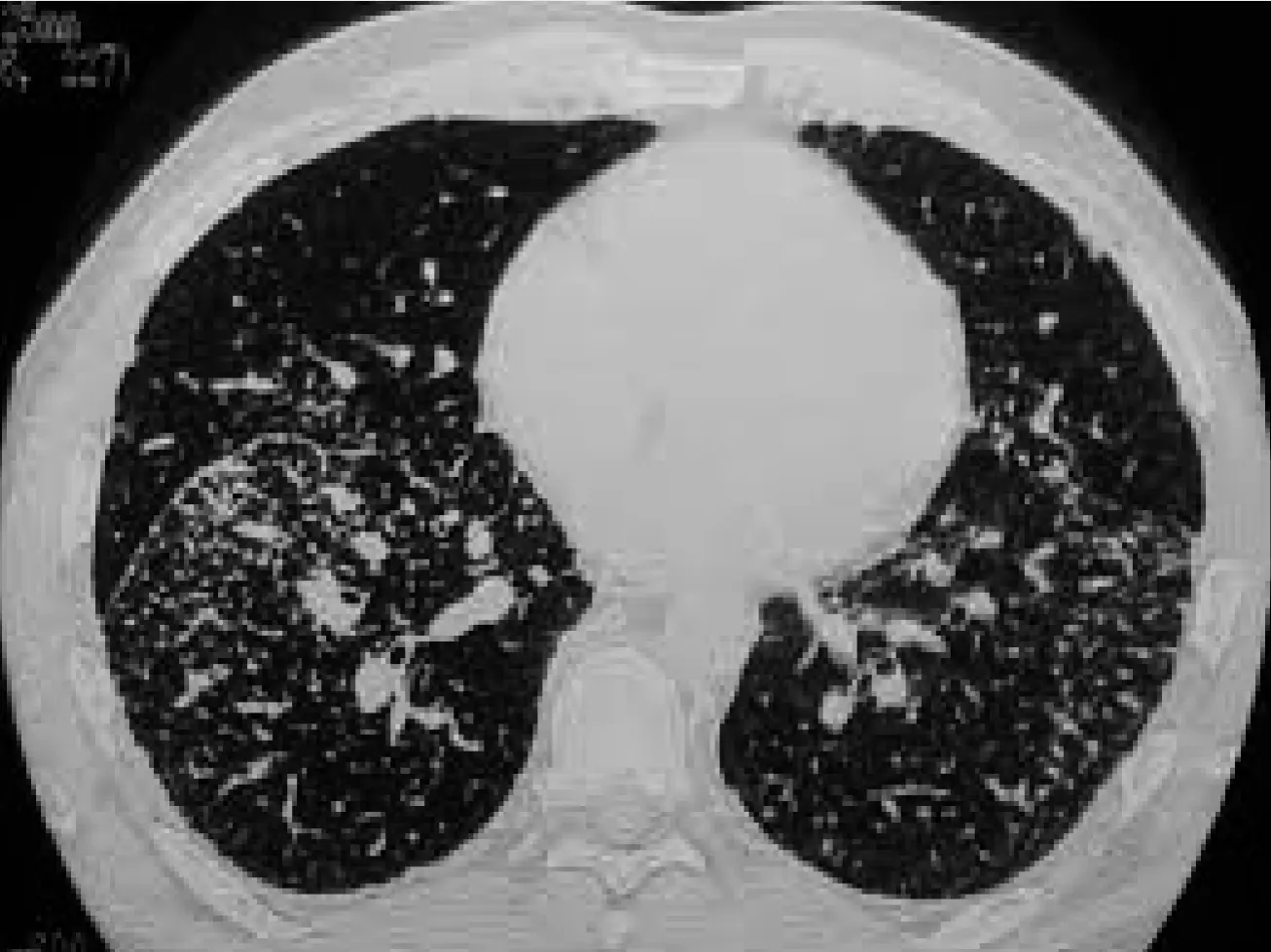
Blood Tests
- ↑ serum ACE.
- ↑ calcium.
- ↑ ESR.
Biopsy
- Non-caseating granulomas (diagnostic).
- Exclude TB and fungal infections.
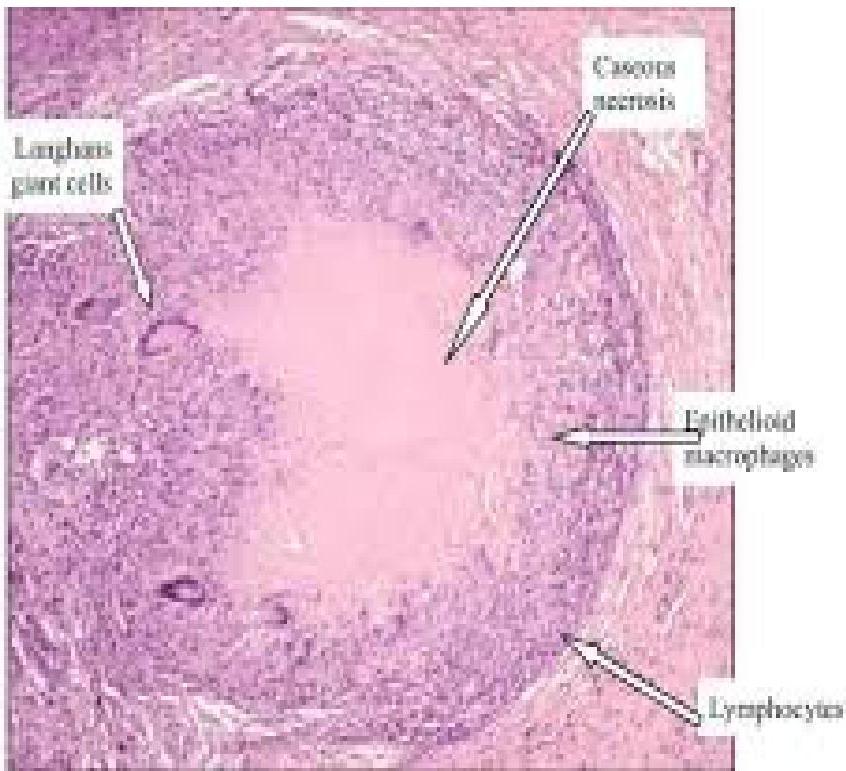
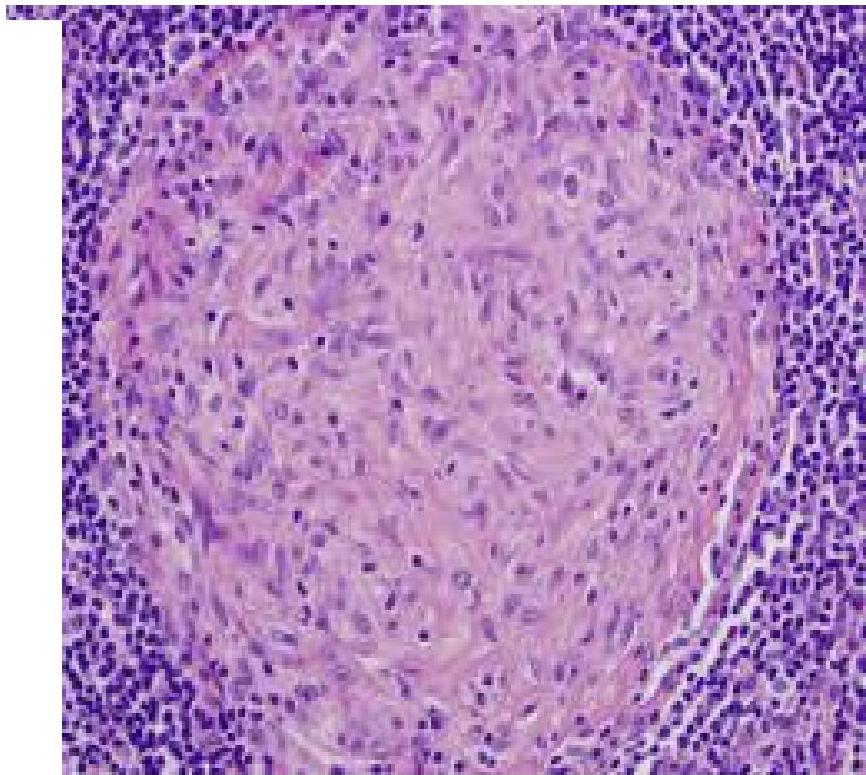
Diagnostic Criteria: Confirming Sarcoidosis
| Clinical and Radiological Suspicion | Histopathological Confirmation | Exclusion of Other Granulomatous Diseases |
|---|---|---|
| Compatible symptoms and imaging findings (often incidental) | Non-caseating epithelioid granulomas in one or more organs | Rule out infections, malignancy, and other granulomatous disorders |
Differential Diagnosis
| Infections | Malignancies | Autoimmune |
|---|---|---|
| Tuberculosis, fungal infections, non-tuberculous mycobacteria | Lymphoma, lung cancer, metastatic disease | Granulomatosis with polyangiitis, eosinophilic granulomatosis |
Other Differential Diagnoses:
- Tuberculosis.
- Lymphoma.
- Fungal infections (e.g., histoplasmosis).
- Hypersensitivity pneumonitis.
- Vasculitis. Z
Clinical Syndromes
Löfgren Syndrome
Characterized by acute onset of:
- Erythema nodosum.
- Bilateral hilar lymphadenopathy.
- Fever.
- Arthritis.
Heerfordt Syndrome (Uveoparotid Fever)
Involves:
- Uveitis.
- Parotid gland swelling.
- Fever.
- Facial nerve palsy.
Management
- Asymptomatic/mild cases may resolve spontaneously.
- Corticosteroids: mainstay of treatment.
- Immunosuppressants: methotrexate, azathioprine in resistant cases.
- Symptomatic treatment for organ involvement.
- Regular monitoring for complications.
Prognosis
- Many cases resolve spontaneously within 2–5 years.
- Chronic progressive disease in ~20%.
- Poor prognosis with cardiac, neurological, or fibrotic lung involvement.
Summary
- Sarcoidosis is a multisystem granulomatous disease of unknown cause.
- Non-caseating granulomas in affected organs.
- Common sites: lungs, lymph nodes, skin, eyes.
- Diagnosis: biopsy + exclusion of infections.
- Treatment: corticosteroids, immunosuppressants if needed.
- Prognosis usually good, but variable.