
Asthma Updated Guidelines
Authors: Lina Serhan, Dr Nada Abdelrahman
This Photo by Unknown Author is licensed under CC BY-SA-NC
Date: 3/4/2024
Learning Objectives
By the end of this session, the student should be able to:
- Diagnose different types of asthmatic attack
- Manage different types and stages of asthma

Aetiology and Pathophysiology
Imbalance in Immune Response
Type 2 T-helper (Th2) cell-mediated response leads to:
- Increased cytokines: IL-4, IL-5, IL-13, IL-25, IL-33
- These promote eosinophilic inflammation
- Immunoglobulin E (IgE) production
- Airway hyperresponsiveness
Environmental Factors
Environmental exposure to allergens:
- Dermatophagoides pteronyssinus (house dust mite)
- Grass pollen
- Domestic pets

Genetic Factors
Immunological Factors
Risk Factors and Associations
- Personal or family history of atopy
- IgE-mediated atopic conditions:
- Atopic dermatitis (eczema)
- Allergic rhinitis (hay fever)
- Antenatal factors:
- Maternal smoking
- Viral infection (RSV)
- Low birth weight; not being breastfed puts baby at risk for asthma
- Air pollution and exposure to allergens
- “Hygiene hypothesis”: Increased risk of asthma in developed countries due to less exposure and therefore less immunity
- Aspirin sensitivity and nasal polyps
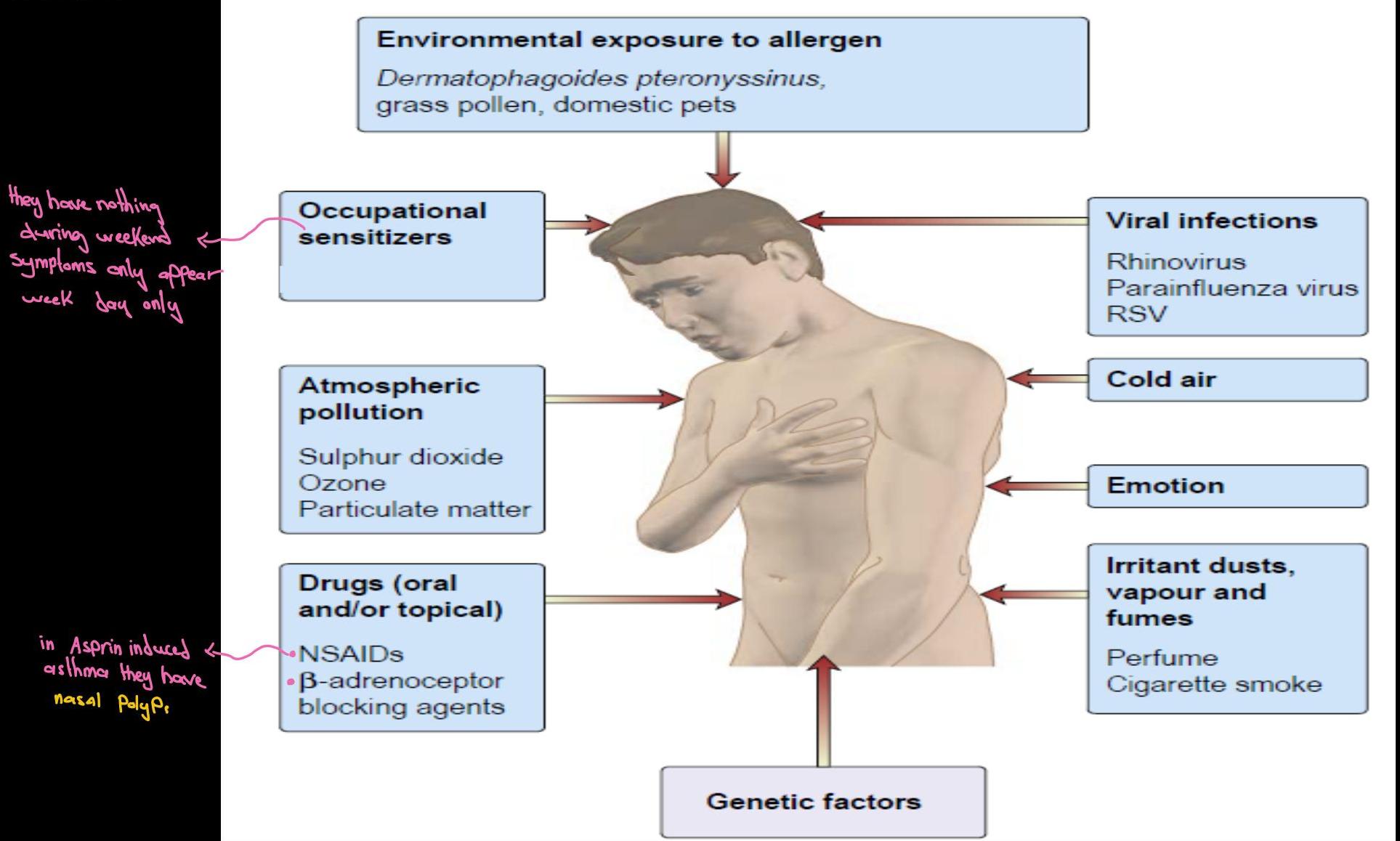

This Photo by Unknown Author is licensed under CC BY-NC
Pathophysiology of Asthma
Note: Video content referenced (line 6)
Investigations and Diagnosis
Objective Tests for Asthma
Guidelines avoid subjective/clinical judgements and advocate objective tests. All patients ≥ 5 years should have objective tests.
1. Fractional Exhaled Nitric Oxide (FeNO)
- 3 types; inducible (iNOS) levels rise in inflammatory cells (eosinophils) and correlate with levels of inflammation
- Positive: ≥ 40 parts per billion (ppb) - Confirmatory with other tests
2. Spirometry and Peak Flow Variability
- Obstructive pattern: FEV1/FVC ratio < 70%
- Note: Could also indicate other diseases like COPD
3. Bronchodilator Reversibility (BDR) Test
- Positive test: Improvement in FEV1 of 12% or more (increase in volume of ≥ 200 ml)
4. Exercise Challenge Test
- Using histamine or methacholine
- Positive test: Reduction in FEV1 of > 10-15% or more (decrease in volume of ≥ 200 ml)
Steps of Investigation (Diagnostic Algorithm)
- Measure FeNO
- Do Spirometry
- If obstruction present → BDR test
- If negative → Monitor Peak Flow variability (2-4 weeks)
- If there’s variability → This is asthma
- If no variability → Go to next step
- If negative → Histamine or methacholine challenge test
- If step 5 unavailable → Suspect and treat

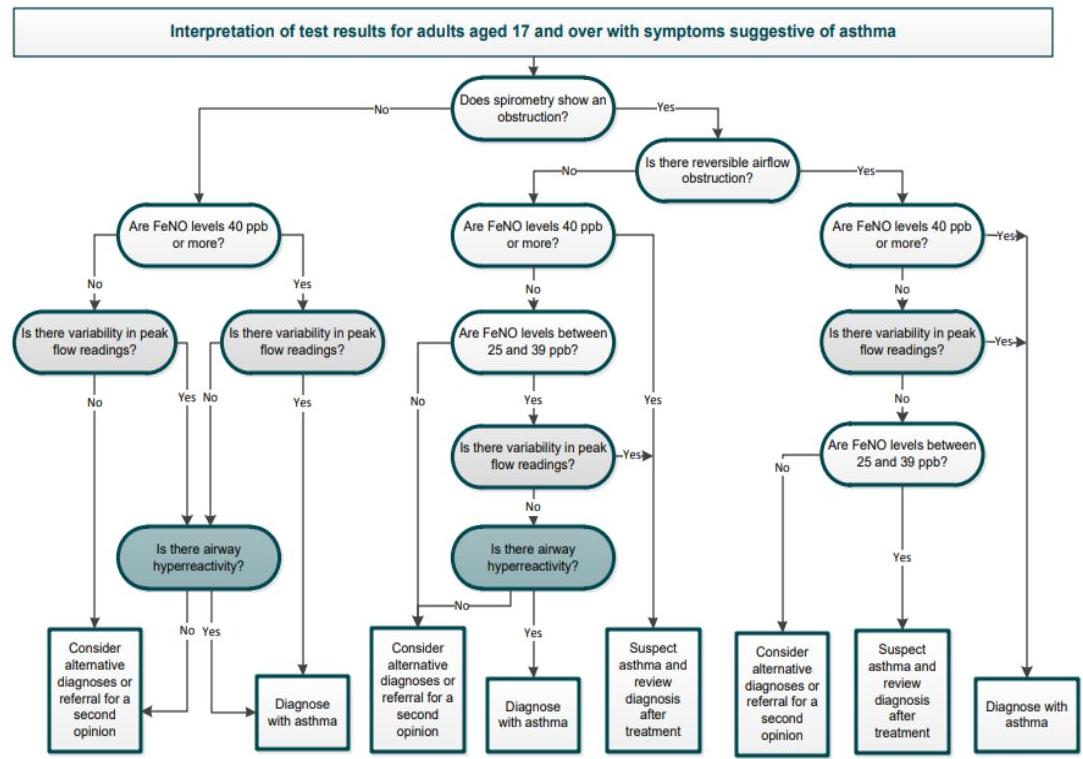
Algorithm C: Objective tests for asthma in adults aged 17 and over
Abbreviations:
- FeNO: Fractional exhaled nitric oxide
- BDR: Bronchodilator reversibility
This algorithm is based on recommendations from NICE’s guideline on asthma, diagnosis, monitoring and chronic asthma management (2017)
Positive Test Thresholds:
- Obstructive spirometry: FEV1/FVC ratio less than 70% (or below the lower limit of normal if available)
- FeNO: 40 ppb or more
- BDR: Improvement in FEV1 of 12% or more and increase in volume of 200 ml or more
- Peak flow variability: Variability over 20%
- Direct bronchial challenge test with histamine or methacholine: PC20 of 8 mg/ml or less
© NICE 2017. All rights reserved. Subject to Notice of rights
Diagnosis Principles
Diagnosis should be based on objective tests.
Asthma Classification (Acute Attack Severity)
| Moderate | Severe | Life-threatening |
|---|---|---|
| • PEFR 50-75% best or predicted | • PEFR 33-50% best or predicted | • PEFR ≤ 33% best or predicted |
| • Speech normal | • Can’t complete sentences | • Oxygen sats < 92% |
| • RR < 25/min | • RR > 25/min | • ‘Normal’ pCO2 (4.6-6.0 kPa) due to Respiratory Fatigue |
| • Pulse < 110 bpm | • Pulse > 110 bpm | • Exhaustion, confusion or coma |
| • Silent chest, cyanosis or feeble respiratory effort | ||
| • Bradycardia, dysrhythmia or hypotension |
“Near-fatal asthma”: Raised pCO₂ and/or requiring mechanical ventilation with raised inflation pressures.
Acute Severe Asthma Management
Initial Assessment (ABC Approach)
- ABC (Airway, Breathing, Circulation)
- Give oxygen
- IV Fluid and Steroid - if very severe and patient able to swallow, give oral prednisolone
- Inhaler β-agonist (salbutamol)
Management of Acute Severe Asthma
Assess Severity of Attack
Evaluate:
- PEF (Peak Expiratory Flow)
- Ability to speak
- RR (Respiratory Rate)
- Pulse rate
- O₂ sats
Warn ICU if severe or life-threatening attack
Immediate Treatment
- Salbutamol 5mg (or terbutaline 10mg) nebulized with O₂
- Hydrocortisone 100mg IV or prednisolone 40-50mg PO (or both if very ill)
- Start O₂ if saturations < 92% (also check ABG), aim sats 94-98%
If Life-threatening Features Present
- Inform ICU and seniors
- Give salbutamol nebulizers every 15 minutes, or 10mg continuously per hour
- Monitor ECG; watch for arrhythmias
- Add ipratropium 0.5mg to nebulizers
- Give single dose of magnesium sulfate (MgSO₄) 1.2-2g IV over 20 minutes
If Not Improving
Refer to ICU for consideration of ventilatory support and intensification of medical therapy (e.g., aminophylline, IV salbutamol) if any of the following signs are present:
- Deteriorating PEF
- Persistent/worsening hypoxia
- Hypercapnia
- ABG showing low pH or high H⁺
- Exhaustion, feeble respiration
- Drowsiness, confusion, altered conscious level
- Respiratory arrest
If Improving Within 15-30 Minutes
- Nebulized salbutamol every 4 hours
- Prednisolone 40-50mg PO for 5-7 days
- Monitor peak flow and O₂ sats, aim 94-98% with supplemental O₂ if needed
Admission Criteria
- All patients with life-threatening asthma require admission
- Severe acute asthma admitted if they fail to respond to initial treatment
- Other admission criteria include:
- Previous near-fatal asthma attack
- Pregnancy
- Attack despite already using oral corticosteroid
- Presentation at night (incidence at night is high)
Discharge Criteria
- Stable on discharge medication (no nebulisers or oxygen) for 12-24 hours
- Inhaler technique checked and recorded
- PEF > 75% of best or predicted

Oxygen Therapy
- If patients are hypoxaemic, start supplemental oxygen therapy
- If patients are acutely unwell: started on 15 L of supplemental O₂ via a non-rebreathe mask, titrated down to a flow rate where they are able to maintain a SpO₂ 94-98%
Bronchodilation
Short-acting beta₂-agonists (SABA):
- High-dose inhaled SABA e.g., salbutamol, terbutaline
- If no features of life-threatening or near-fatal asthma: standard pressurised metered-dose inhaler (pMDI) or oxygen-driven nebulizer
- Life-threatening exacerbation: nebulised SABA is recommended

Corticosteroid Therapy
- All patients: Given 40-50mg of prednisolone orally (PO) daily, continued for at least 5 days or until recovery
- If on inhaled steroid: continue
Additional Therapies
- Ipratropium bromide: For severe or life-threatening asthma, or if not responding to beta₂-agonist and corticosteroid treatment, use nebulised ipratropium bromide
- IV magnesium sulphate: For severe/life-threatening asthma
- IV aminophylline: Consultation required; for patients who fail to respond, require senior critical care support and should be treated in an appropriate ITU/HDU setting
Treatment options for refractory cases:
- Intubation and ventilation
- Extracorporeal membrane oxygenation (ECMO)
Typical Lung Function Results in Asthma
- FEV1 - significantly reduced
- FVC - normal
- FEV1% (FEV1/FVC) < 70%
ABG Interpretation in Life-threatening Asthma
Example ABG findings in life-threatening attack:
| Parameter | Value | Normal Range |
|---|---|---|
| pH | 7.37 | (7.35-7.45) |
| pO2 | 10.1 kPa | (>9 kPa) |
| pCO2 | 4.9 kPa | (4.7-6.0 kPa) - normal |
| Base excess | 1.1 | (-2 to 2) |
| Lactate | 1.9 mmol/L | (<2 mmol/L) |
Note: “Normal” pCO2 in the setting of severe asthma indicates respiratory fatigue (cannot hyperventilate to compensate)
Chronic Asthma Management
Pharmacological Agents Overview
| Drug | Mechanism of Action | Notes |
|---|---|---|
| Salbutamol | Beta receptor agonist | • Short-acting inhaled bronchodilator. Relaxes bronchial smooth muscle through effects on beta 2 receptors • Used in asthma and chronic obstructive pulmonary disease (COPD) • Salmeterol has similar effects but is long-acting |
| Corticosteroids | Anti-inflammatory | • Inhaled corticosteroids are used as maintenance therapy • Oral or intravenous corticosteroids are used following an acute exacerbation of asthma or COPD |
| Ipratropium | Blocks the muscarinic acetylcholine receptors | • Short-acting inhaled bronchodilator. Relaxes bronchial smooth muscle • Used primarily in COPD • Tiotropium has similar effects but is long-acting |
| Methylxanthines (e.g., theophylline) | Non-specific inhibitor of phosphodiesterase resulting in an increase in cAMP | • Given orally or intravenously • Has a narrow therapeutic index |
| Montelukast, zafirlukast | Blocks leukotriene receptors | • Usually taken orally • Useful in aspirin-induced asthma |
Stepwise Management Approach
| Step | Clinical Scenario | Treatment |
|---|---|---|
| 1 | Newly-diagnosed asthma | Short-acting beta agonist (SABA) |
| 2 | Not controlled on previous step OR newly-diagnosed with symptoms ≥ 3/week or night-time waking | SABA + low-dose inhaled corticosteroid (ICS) |
| 3 | Not controlled on Step 2 | SABA + low-dose ICS + leukotriene receptor antagonist (LTRA) |
| 4 | Not controlled on Step 3 | SABA + low-dose ICS + long-acting beta agonist (LABA) Continue LTRA depending on patient’s response |
| 5 | Not controlled on Step 4 | SABA +/- LTRA Switch ICS/LABA for a maintenance and reliever therapy (MART), that includes a low-dose ICS |
| 6 | Not controlled on Step 5 | SABA +/- LTRA + medium-dose ICS MART OR consider changing back to a fixed-dose of a moderate-dose ICS and a separate LABA (400-800 mcg) |
| 7 | Not controlled on Step 6 | SABA +/- LTRA + one of the following: • Increase ICS to high-dose (>800 mcg) - only as part of fixed-dose regime, not as MART • Trial of additional drug (e.g., LAMA or theophylline) • Seek expert advice |
Maintenance and Reliever Therapy (MART)
- A form of combined ICS and LABA treatment in which a single inhaler, containing both ICS and a fast-acting LABA, is used for both daily maintenance therapy and the relief of symptoms as required
- MART is only available for ICS and LABA combinations in which the LABA has a fast-acting component (e.g., formoterol)
Important Notes on Chronic Management
- Don’t change treatment in patients who have well-controlled asthma simply to adhere to the latest guidance
- In the step-down approach: aim for a reduction of 25-50% in the dose of inhaled corticosteroids
Inhaled Corticosteroid (ICS) Doses
| Dose Category | Budesonide Equivalent |
|---|---|
| Low dose | ≤ 400 micrograms |
| Moderate dose | 400-800 micrograms |
| High dose | > 800 micrograms |
Asthma Management Algorithm Summary
Diagnosed Adult Asthma - Evaluation Steps:
- Assess symptoms
- Measure lung function
- Check inhaler technique and adherence
- Adjust dose
- Update self-management plan
- Move up and down as appropriate
For Suspected Asthma:
- Consider monitored initiation of treatment with low-dose ICS
- Short-acting β₂ agonists as required (unless using MART)
- Consider moving up if using three doses a week or more
Special Populations
Occupational Asthma
Common Causative Agents
Exposure to the following chemicals is associated with occupational asthma:
- Isocyanates - the most common cause
- Spray painting and foam moulding using adhesives
- Platinum salts
- Soldering flux resin
- Glutaraldehyde
- Flour
- Epoxy resins
- Proteolytic enzymes
Clinical Clues
- Patient concerns: chemicals at work are worsening their asthma
- Doctor: history that symptoms seem better at weekends / when away from work
Investigations
- Serial measurements of peak expiratory flow are recommended at work and away from work (at home)
- Referral to respiratory specialist for suspected patients

Best investigation: Serial peak flows at home and at work
Asthma and Pregnancy
Management Principles
- Reassure the patient
- Guidelines emphasize good control of asthma during pregnancy
- Most drugs are safe during pregnancy and breastfeeding
Safe Medications
- Inhaled drugs: beclometasone and salmeterol
- Theophylline
- Prednisolone

Medication Adjustment When Planning Pregnancy
For a patient with well-controlled asthma trying for a baby:
- In the step-down approach: aim for a reduction of 25-50% in the dose of inhaled corticosteroids
Quick Facts and Key Knowledge Points
Beta-2 Adrenergic Agonists for Acute Asthma
Which beta-2 adrenergic agonist is used to treat acute asthma?
- Albuterol (also known as Salbutamol)
Zileuton Mechanism of Action
What is the MOA of Zileuton?
- Inhibits 5-lipoxygenase and leukotrienes
Bronchial Provocation Testing
The muscarinic agonist methacholine is used in bronchial provocation challenges to diagnose asthma.
Ipratropium Mechanism of Action
What is the MOA of Ipratropium?
- Competitive inhibition of ACh muscarinic receptors
Omalizumab Mechanism
Omalizumab is indicated for the treatment of asthma by preventing IgE from binding to mast cells.
Side Effects of Long-acting Beta2-agonists
Tremor and cardiac arrhythmias are side effects of long-acting beta2-adrenergic agonists such as formoterol or salmeterol.
Differential Diagnosis Considerations
Remember
Asthma is not only asthma - always consider other possible diagnoses.

Churg-Strauss Syndrome (Eosinophilic Granulomatosis with Polyangiitis)
A 50-year-old man with late-onset asthma presents with:
- Malaise
- Weight loss
- Recurrent bouts of sinusitis
- Bloods show marked eosinophilia
This is a stereotypical history of Churg-Strauss syndrome (now called Eosinophilic Granulomatosis with Polyangiitis or EGPA).
Case Scenarios and Questions
Question 1: Features of Life-threatening Asthma
When assessing a patient with acute asthma they are classified as being moderate, severe or life-threatening. Which one of the following is a feature of life-threatening asthma?
- A. Pulse > 110 bpm (Feature of severe asthma)
- B. RR < 25/min (Feature of moderate asthma)
- C. Pulse < 110 bpm (Feature of moderate asthma)
- D. Speech normal (Feature of moderate asthma)
- E. RR > 25/min (Feature of severe asthma)
- F. Oxygen sats < 92% ✓ (CORRECT - Feature of life-threatening asthma)
Question 2: Features of Moderate Asthma (Version 1)
Which one of the following is a feature of moderate asthma?
- A. Oxygen sats < 92% (Life-threatening)
- B. Pulse > 110 bpm (Severe)
- C. RR > 25/min (Severe)
- D. PEFR 33-50% best or predicted (Severe)
- E. Speech normal ✓ (CORRECT - Feature of moderate asthma)
- F. Can’t complete sentences (Severe)
Question 3: Features of Moderate Asthma (Version 2)
Which one of the following is a feature of moderate asthma?
- A. RR > 25/min (Severe)
- B. Can’t complete sentences (Severe)
- C. Pulse > 110 bpm (Severe)
- D. PEFR 50-75% best or predicted ✓ (CORRECT - Feature of moderate asthma)
- E. Exhaustion, confusion or coma (Life-threatening)
- F. PEFR 33-50% best or predicted (Severe)
Question 4: Features NOT Seen in Severe Asthma
Which one of the following is NOT a feature of severe asthma?
- A. RR < 25/min ✓ (CORRECT - This is a feature of MODERATE asthma, NOT severe)
- B. PEFR 33-50% best or predicted (This IS severe)
- C. Oxygen sats < 92% (Actually life-threatening, not just severe)
- D. RR > 25/min (This IS severe)
- E. Can’t complete sentences (This IS severe)
Question 5: Features of Severe Asthma
Which one of the following is a feature of severe asthma?
(Options same as above - correct answer would be: PEFR 33-50%, RR > 25/min, Pulse > 110 bpm, or Can’t complete sentences)
Question 6: Life-threatening Features (Reiteration)
Which one of the following is a feature of life-threatening asthma?
- A. PEFR 33-50% best or predicted (Severe)
- B. RR < 25/min (Moderate)
- C. Bradycardia, dysrhythmia or hypotension ✓ (CORRECT - Life-threatening)
- D. Pulse < 110 bpm (Moderate)
- E. Pulse > 110 bpm (Severe)
- F. Can’t complete sentences (Severe)
Question 7: Step 1 Management - Newly Diagnosed
What is the most appropriate next step in the following scenario: newly diagnosed adult with asthma (symptoms < 3 times/week)?
- A. Switch to either a MART regime with a moderate-dose ICS or to separate moderate-dose ICS and LABA inhalers
- B. Add a low-dose ICS ✓ (CORRECT - Step 2)
- C. Stop LABA + increase ICS to medium-dose
- D. Add a SABA (Already have this)
- E. Switch ICS/LABA for a MART regime with a low-dose ICS
- F. Add a LABA
Question 8: Step 2 Management - Not Controlled
What is the most appropriate next step in the following scenario: adult with asthma not controlled by a SABA + low-dose ICS?
- A. Add a leukotriene receptor antagonist ✓ (CORRECT - Step 3)
- B. Add a LABA
- C. Stop LABA + increase ICS to medium-dose
- D. Trial of either high-dose ICS as part of fixed-dose regime, additional drug (e.g. LAMA or theophylline) or referral
- E. Switch to either a MART regime with a moderate-dose ICS or to separate moderate-dose ICS and LABA inhalers
- F. Add a SABA
Question 9: Step 4 Management - Still Not Controlled
What is the most appropriate next step in the following scenario: adult with asthma not controlled by a SABA + low-dose ICS +/- leukotriene receptor antagonist + LABA?
Options table format:
- A. Add daily oral prednisolone
- B. Add a LABA (Already on LABA)
- C. Switch to either a MART regime with a moderate-dose ICS or to separate moderate-dose ICS and LABA inhalers ✓ (CORRECT)
- D. Stop LABA + increase ICS to medium-dose
- E. Switch ICS/LABA for a MART regime with a low-dose ICS (Step 5, not 4)
- F. Trial of either high-dose ICS as part of fixed-dose regime, additional drug (e.g. LAMA or theophylline) or referral (Step 7)
Question 10: Step 5 Management - MART Low-dose Not Controlled
What is the most appropriate next step in the following scenario: adult with asthma not controlled by a SABA +/- leukotriene receptor antagonist + MART regime with a low-dose ICS?
Options table format:
- A. Trial of either high-dose ICS as part of fixed-dose regime, additional drug (e.g. LAMA or theophylline) or referral ✓ (CORRECT - Step 7)
- B. Add a low-dose ICS (Already on ICS)
- C. Add a LABA (Already in MART)
- D. Switch to either a MART regime with a moderate-dose ICS or to separate moderate-dose ICS and LABA inhalers (Step 4)
- E. Stop LABA + increase ICS to medium-dose
- F. Add a leukotriene receptor antagonist
Question 11: Alternative Step 3 Management
What is the most appropriate next step in the following scenario: adult with asthma not controlled by a SABA + low-dose ICS + leukotriene receptor antagonist?
- A. Switch to either a MART regime with a moderate-dose ICS or to separate moderate-dose ICS and LABA inhalers ✓ (CORRECT - Step 4)
- B. Add a LABA (This is essentially what the answer means)
- C. Stop LABA + increase ICS to medium-dose
- D. Trial of either high-dose ICS as part of fixed-dose regime, additional drug (e.g. LAMA or theophylline) or referral
- E. Add daily oral prednisolone
- F. Add a low-dose ICS (Already on ICS)
Question 12: Step 1 - Not Controlled by SABA Only
What is the most appropriate next step in the following scenario: adult with asthma not controlled by a SABA?
- A. Add daily oral prednisolone
- B. Add a LABA (Without ICS is not recommended)
- C. Add a SABA (Already on this)
- D. Add a low-dose ICS ✓ (CORRECT - Step 2)
- E. Add a leukotriene receptor antagonist (Step 3)
- F. Switch ICS/LABA for a MART regime with a low-dose ICS
Question 13: Step 6 Management - MART Moderate-dose Not Controlled
What is the most appropriate next step in the following scenario: adult with asthma not controlled by a SABA +/- leukotriene receptor antagonist + MART regime with a moderate-dose ICS?
- A. Add daily oral prednisolone
- B. Stop LABA + increase ICS to medium-dose
- C. Add a LABA
- D. Switch ICS/LABA for a MART regime with a low-dose ICS
- E. Trial of either high-dose ICS as part of fixed-dose regime, additional drug (e.g. LAMA or theophylline) or referral ✓ (CORRECT - Step 7)
- F. Switch to either a MART regime with a moderate-dose ICS or to separate moderate-dose ICS and LABA inhalers
Question 14: Acute Severe Asthma - Additional Medication
An 18-year-old man is admitted to the emergency department with an episode of acute asthma. He is:
- Unable to complete sentences
- Tachycardic (118 beats per minute)
- Tachypnoeic (respiratory rate 30)
- Has received salbutamol, ipratropium bromide nebulisers and intravenous hydrocortisone through a large bore cannula in the right antecubital fossa
- Despite another salbutamol nebuliser, there is no improvement
What medication would be most appropriate to add?
- A. Beclomethasone (Already on systemic steroids)
- B. Magnesium sulphate ✓ (CORRECT - For severe/life-threatening not responding to initial treatment)
- C. Amoxicillin (No indication of infection)
- D. Nifedipine (Not indicated)
- E. Adrenaline (Not first-line)
Question 15: Occupational Asthma - Best Investigation
Which one of the following is the best investigation for occupational asthma?
- A. Spirometry (Useful but not best for occupational)
- B. Serum IgE (Non-specific)
- C. Schirmer’s test (For Sjögren’s syndrome)
- D. Serial peak flows at home and at work ✓ (CORRECT - Best test)
- E. Overnight dexamethasone suppression test (For Cushing’s)
- F. Serum tryptase (For mastocytosis/anaphylaxis)
Question 16: Occupational Asthma - Causative Agent
A 45-year-old man presents with a three-month history of wheezing and dyspnoea whilst at work. His symptoms improve significantly when at home and at weekends.
What is the likely causative agent?
- A. Simple coal worker’s lung (Pneumoconiosis)
- B. Silica (Silicosis)
- C. Cotton dust (Byssinosis)
- D. Asbestos (Asbestosis/mesothelioma)
- E. Isocyanates ✓ (CORRECT - Most common cause of occupational asthma)
Question 17: Pregnancy Planning - Medication Adjustment
A 28-year-old woman is attending her annual asthma review. She is currently prescribed:
- Salbutamol inhaler 100μg
- Budesonide 400μg
Her asthma is well controlled and she hasn’t needed to use her ‘blue inhaler’ over the past year. She is currently trying for a baby and is concerned about taking her asthma medications during pregnancy.
What is the most appropriate change to her medications?
- A. Add leukotriene receptor antagonist
- B. Reduce budesonide dose ✓ (CORRECT - Step down by 25-50%)
- C. Reduce salbutamol dose (Not needed - she doesn’t use it)
- D. Stop budesonide (Too drastic - maintain control)
- E. Stop salbutamol (Keep for rescue)
References
- Kumar: Pages 949-954
Document improved and restructured for educational purposes
Original date: 3/4/2024
