Approach to Abdominal Pain in Children
Ibrahim Alsaif
Goals and Objectives
- Be Systematic
- Evaluate then identify the problem then intervene.
- Anatomic and Pathophysiology of pain
- Is the pain acute or chronic?
- Causes of abdominal pain
- Approach to reach the diagnosis
- Red flags
- Indications for Surgical consultation.
What is the Problem?
-
Mesenteric lymphadenitis
- Pain in left side
- With recurrent tonsillitis
- Diagnosed by US
-
Infantile colic Z
- Most common age of diagnosis is first few months
- Presentation: baby flexes hip joint with gases/flatus
- Pain started after changing from breast to formula
-
Mediterranean fever
- Fever - Recurrent abdominal pain
- More than one in the family
- Vasculitis - arthritis - jaundice
- +ve Consanguinity - Mediterranean origin
- In examination: normal
-
Most Common Cause of Abdominal Pain in Pediatric: “Gastrointestinism”
- Regardless of the age
- Then constipation
Systematic Approach to a Sick Child
Initial impression (appearance, work of breathing, circulation)
Is the child need Resuscitation (CPR)?
Yes → C A B
No →
Evaluate:
- Primary assessment (ABCDE approach)
- Secondary assessment (focused H&P)
- Diagnostic tests
Intervene
Identify
What is Abdominal Pain?
- Abdominal pain is a common complaint in all settings of medical practice.
- Pain may be a symptom of a severe, life-threatening disease or of a benign underlying condition.
- A general understanding of abdominal anatomy, physiology, and pathophysiology is vital when formulating a differential diagnosis for abdominal pain.
Anatomic Origin of Pain
The classic division of abdomen:
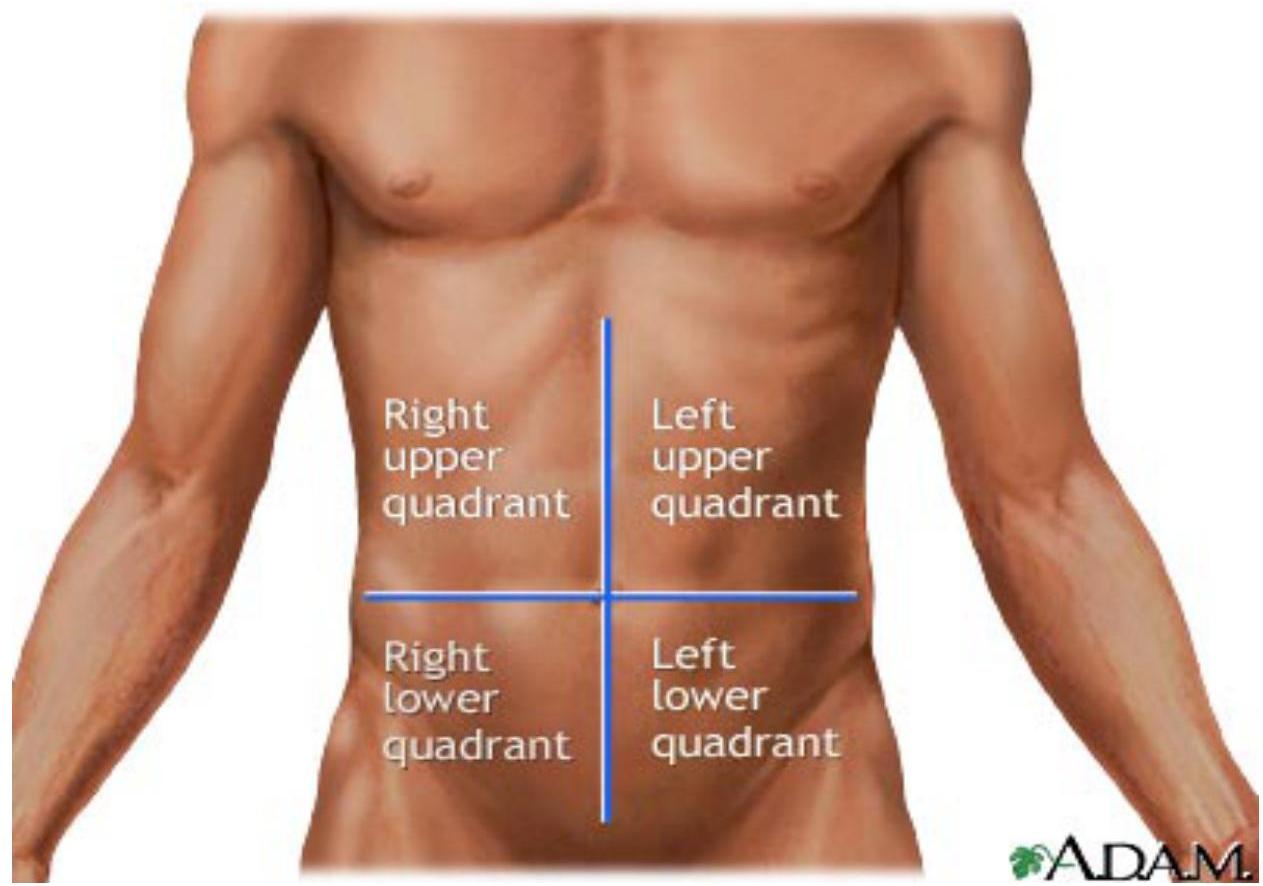
Abdomen is divided into 9 regions:
- 2 vertical lines (RT & LT midclavicular)
- 2 horizontal lines (subcostal and intertubercular)
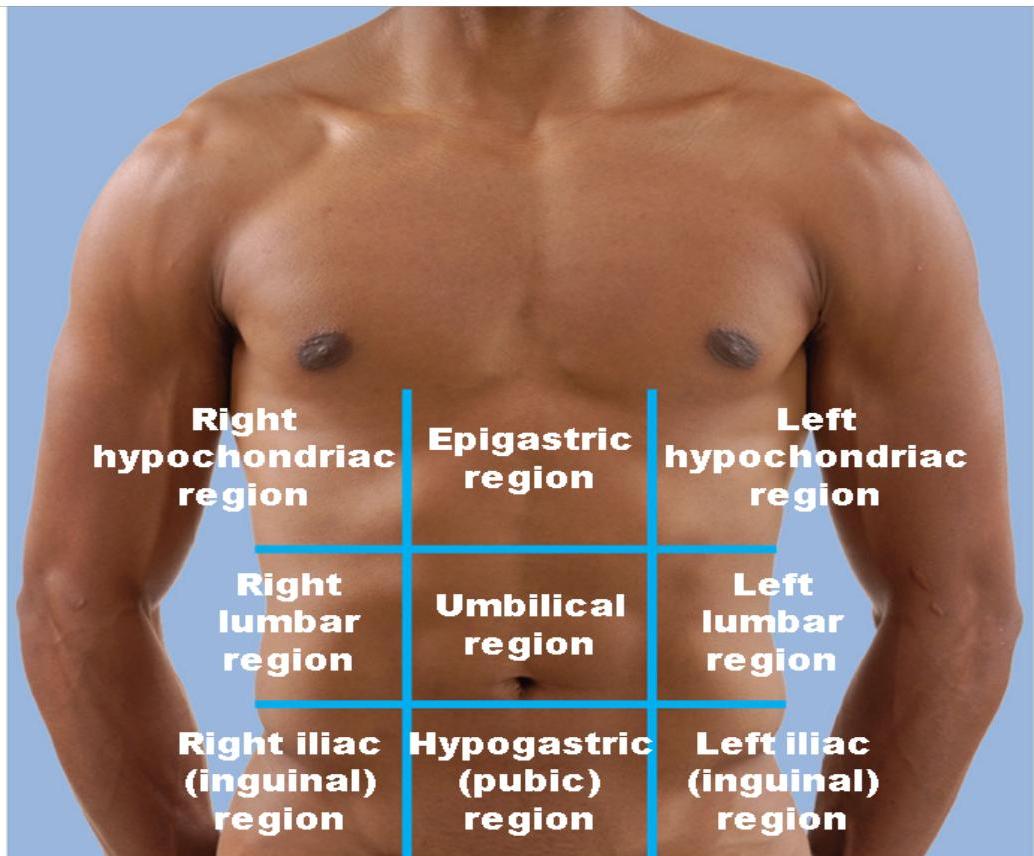 (a) Nine regions delineated by four planes
(a) Nine regions delineated by four planes
ped.emergency.Dr.AIsaif 9/25/22
Pathophysiology
Types of Pain
Visceral Pain
- Due to irritation of visceral peritoneum
- Dull
- Poorly localized
- Usually periumbilical
Parietal (Somatic) Pain
- Due to irritation of parietal peritoneum
- Sharp
- Intense
- Discrete
- Localized
- Aggravated by coughing or movement
Referred Pain
- Same features as parietal pain
- Results from shared central pathways for afferent neurons from different sites
- Classic example: Pneumonia (the T9 dermatome distribution is shared by the lung and the abdomen)
Classification: Acute vs. Chronic Pain
Acute Abdominal Pain
A sudden, severe abdominal pain of unclear cause lasting less than one week.
Chronic Abdominal Pain
- Intermittent or constant abdominal pain (of functional or organic etiology) lasting for at least two months
- Chronic abdominal pain occurs in 10 to 20% of children
Classically defined by four criteria:
- ≥3 episodes of abdominal pain
- Episodes occur over a period of ≥2 months
- Pain sufficiently severe to affect activities
- No known organic cause
Causes of Abdominal Pain
Age is a key factor in the evaluation of abdominal pain.
Causes by Age Group
| Birth to One Year | Two to Five Years | Six to 11 Years | 12 to 18 Years |
|---|---|---|---|
| Infantile colic Z | Gastroenteritis | Gastroenteritis | Appendicitis |
| Gastroenteritis | Appendicitis | Appendicitis | Gastroenteritis |
| Constipation | Constipation | Constipation | Constipation |
| Urinary tract infection | Urinary tract infection | Functional pain | Dysmenorrhea |
| Intussusception | Intussusception | Urinary tract infection | Mittelschmerz |
| Volvulus | Volvulus | Trauma | Pelvic inflammatory disease |
| Incarcerated hernia | Trauma | Pharyngitis | Threatened abortion |
| Hirschsprung’s disease | Pharyngitis | Pneumonia | Ectopic pregnancy |
| Sickle cell crisis | Sickle cell crisis | Ovarian/testicular torsion | |
| Henoch-Schönlein purpura | Henoch-Schönlein purpura | ||
| Mesenteric lymphadenitis | Mesenteric lymphadenitis |
Categorical Classification
| Gastrointestinal Causes | Genitourinary Causes | Drugs and Toxins |
|---|---|---|
| Gastroenteritis | Urinary tract infection | Erythromycin |
| Appendicitis | Urinary calculi | Salicylates |
| Mesenteric lymphadenitis | Dysmenorrhea | Lead poisoning |
| Constipation | Mittelschmerz | Venoms |
| Abdominal trauma | Pelvic inflammatory disease | Pulmonary Causes |
| Intestinal obstruction | Threatened abortion | Pneumonia |
| Peritonitis | Ectopic pregnancy | Diaphragmatic |
| Food poisoning | Ovarian/testicular torsion | Pleurisy |
| Peptic ulcer | Endometriosis | Miscellaneous |
| Meckel’s diverticulum | Hematocolpos | Infantile colic |
| Inflammatory bowel disease | Metabolic Disorders | Functional pain |
| Lactose intolerance | Diabetic ketoacidosis | Pharyngitis |
| Liver, spleen, and biliary tract disorders | Hypoglycemia | Angioneurotic edema |
| Hepatitis | Porphyria | Familial Mediterranean fever |
| Cholecystitis | Acute adrenal insufficiency | |
| Cholelithiasis | Hematologic Disorders | |
| Splenic infarction | Sickle cell anemia | |
| Rupture of the spleen | Henoch-Schönlein purpura | |
| Pancreatitis | Hemolytic uremic syndrome |
Approach to Diagnosis
Key Fact
Based on history and physical exam alone, physicians were able to correctly differentiate between organic and nonorganic causes of abdominal pain nearly 80% of the time.
History
Record history in the chronological order of symptoms.
Analyzing the Abdominal Pain
Place/Location:
- Ask child to use one finger to locate the pain
Quality:
- Pain can be a sharp stabbing pain (i.e., trauma) or diffuse, poorly localized pain (i.e., chronic or visceral pain)
Radiation:
- Pain can radiate from its point of origin in any direction
Timing/Onset:
- Onset of the pain
- Duration of pain
- Course during the day
- Does it wake them at night?
- Frequency of episodes
Severity:
- Degree of pain on a scale of 10
Alleviating Factors
Anything that reduces the pain:
- Body position
- Movements
- Medications
Aggravating Factors
Anything that increases the pain:
- Body position
- Movements
- Relation to food intake
Associated Symptoms
Hematemesis, vomiting, nausea, melena, diarrhea, fever, and weight loss.
Associated Symptoms Reference Table
| Associated Symptom | Relevance |
|---|---|
| Diarrhea | Gastroenteritis, Protein losing enteropathy |
| Bloody stool | Ulcerative colitis, necrotizing enterocolitis, dysentery, constipation |
| Hematemesis | Peptic Ulcer Disease, Gastritis |
| Bilious emesis | Small bowel obstruction |
| Jaundice | Hepatitis or Biliary obstruction |
| Joint pain/swelling | IBD, HSP |
| Skin Lesions | IBD, HSP, Liver disease |
| Testicular pain | Testicular torsion |
| Dysuria/polyuria/hematuria | Urinary tract infection/Pyelonephritis |
| Vaginal/Penile discharge | STI |
| Dysmenorrhea | Endometriosis |
| Shortness of breath | Pneumonia or empyema |
Additional History Components
Bowel Patterns and Diet
- Bowel movement patterns and stool quality (size, hard/soft, odour)
- Ingestion of toxin or foreign object
- Accidental or non-accidental trauma
- Dietary history: in young children, too much milk can lead to constipation
Past Medical History
Medical illnesses that predispose to abdominal pain:
- Cystic fibrosis → predisposes to gallstones
- Spina bifida/cerebral palsy/developmental delay → predisposes to constipation
- Sickle cell disease → predisposes to splenic autoinfarction
- Recurrent respiratory tract infections → suggest mesenteric adenitis
Family and Social History
- Family medical history, especially inflammatory bowel disease
- Travel history
- Social and psychiatric history (potential stressors)
Physical Examination
General Examination
- ABCDE approach
- Vital signs and growth parameters
- Evidence of failure to thrive?
Inspection
Look for:
- Contour, symmetry, pulsations, peristalsis
- Skin markings, wall protrusions (hernias)
- Signs of trauma (bruising, swelling)
- Abdominal distension
Auscultation
Important: Auscultate before palpation in the abdominal exam.
- Listen for bowel sounds, abdominal bruits
- Pressure of the stethoscope also tests for tenderness
Percussion
- Tympanic vs non-tympanic
- Percuss for liver span and spleen tip
- Assess for ascites
Palpation
- Tenderness with light and deep palpation
- Guarding and rebound tenderness
- Palpate for liver, spleen, kidney, and abdominal masses (including fecal mass)
Digital Rectal Exam
- First examine the anus for fissures and skin tags
- Then assess for tone, stool, and blood
Special Tests
There are a number of special tests for each differential diagnosis.
Physical Exam Findings by Condition
| Medical Condition | Findings on Physical Exam |
|---|---|
| Constipation | Abdominal tenderness, palpable fecal mass, look for imperforate anus or stenosis, spina bifida, developmental delay, cerebral palsy |
| Acute appendicitis | Patient avoids movement, rebound tenderness, McBurney sign (pain at 2/3 between umbilicus and right ASIS), Rovsing sign (pain in right lower quadrant on left-sided palpation), Psoas sign (pain in right lower quadrant when child on left and right hip hyperextended), Obturator sign (pain in right lower quadrant on internal rotation of flexed right thigh) |
| Gastroenteritis | Diffuse pain with no rebound tenderness, abdominal distension, hyperactive bowel sounds |
| Irritable bowel syndrome | Periumbilical tenderness, no rebound tenderness |
| Trauma | Signs of bruising and tenderness |
| Celiac Disease | Growth failure, distended abdomen, diffuse abdominal tenderness |
| Inflammatory bowel disease | Appears thin, abdominal tenderness, anal skin tags, possible sign of bloody stool on DRE, examine for skin lesions (erythema nodosum, pyoderma gangrenosum), iritis, and joint inflammation |
| Urinary tract infection | Fever, suprapubic and costovertebral angle tenderness, irritability, foul-smelling urine, gross hematuria |
| Primary dysmenorrhea | Lower abdominal tenderness |
| Pneumonia and Empyema | Tachypnea, cyanosis, decreased breath sounds, crackles and rales, dullness on percussion, febrile |
Associated Signs
General Associated Signs
- Jaundice suggests hemolysis or liver disease
- Pallor and jaundice point to sickle cell crisis
Psoas & Obturator Test
If positive, suggests:
- Inflamed retrocecal appendix
- Ruptured appendix
- Iliopsoas abscess
Murphy’s Sign
Definition: Interruption of deep inspiration by pain when the physician’s fingers are pressed beneath the right costal margin
Clinical Significance: Suggests acute cholecystitis
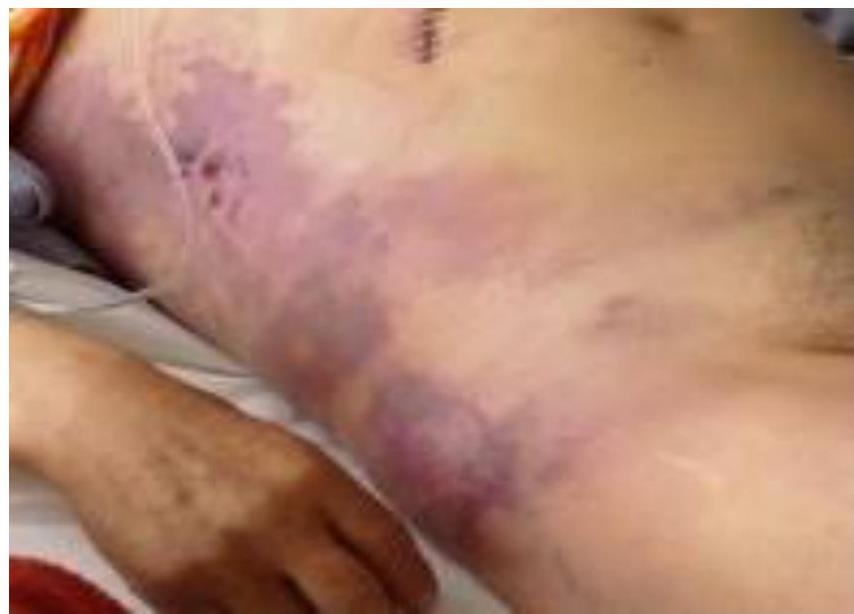
Hemorrhage Signs
- Cullen’s sign: Bluish discoloration of the umbilicus
- Grey Turner’s sign: Discoloration in the flank
Unusual signs of internal hemorrhage
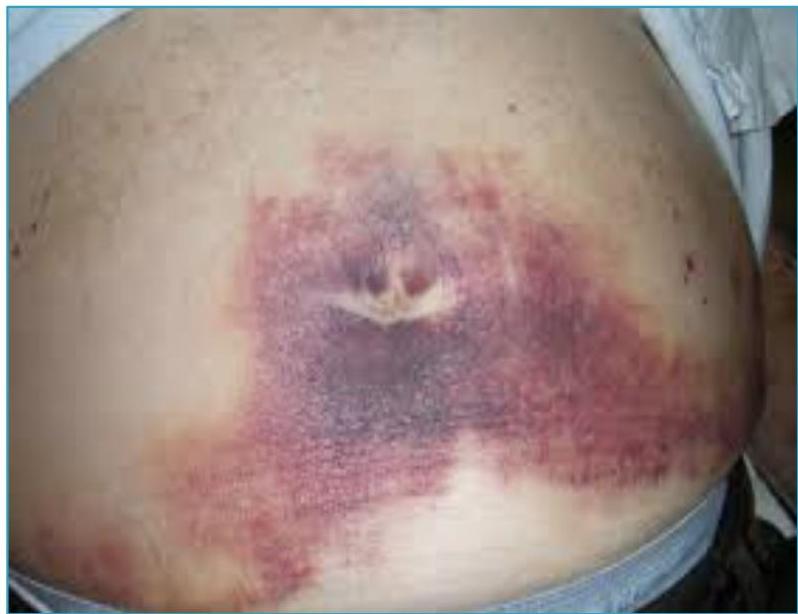
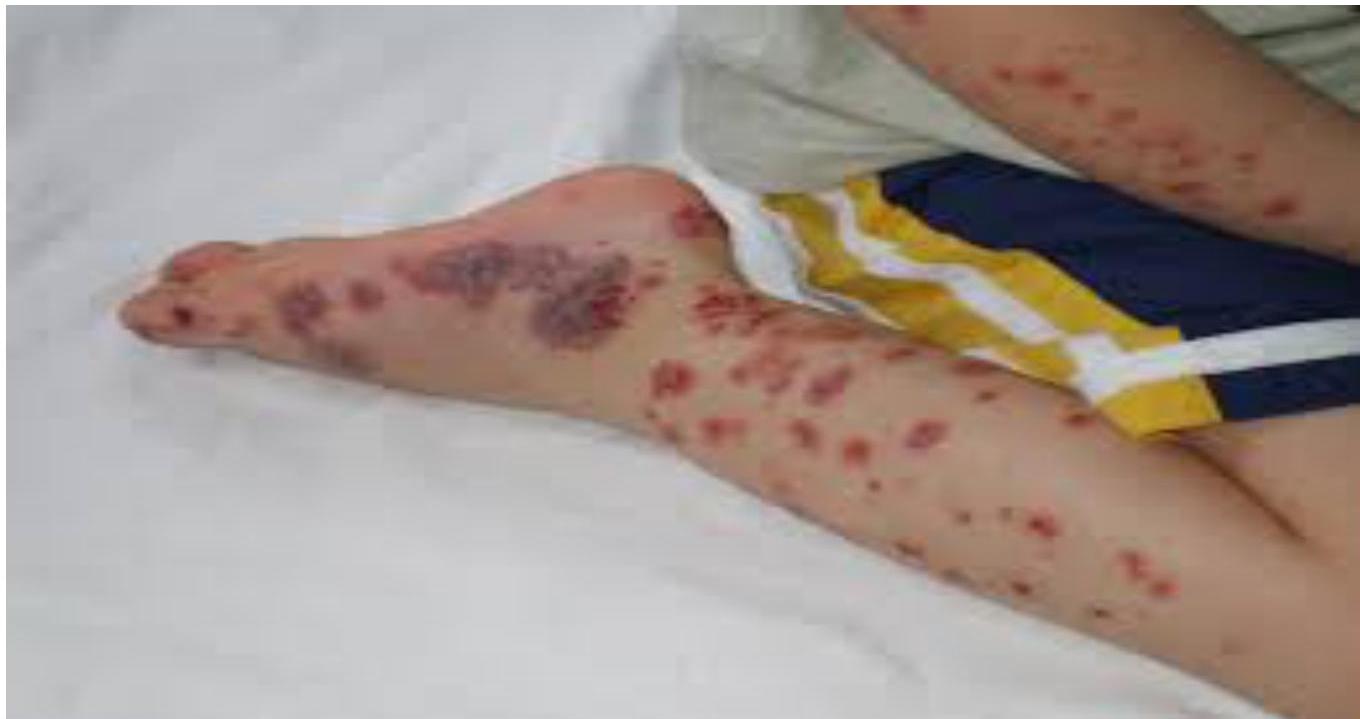
Purpura and Arthritis
Clinical Significance: Henoch-Schönlein purpura
Uncommon Differential Diagnoses and Potential Complications
| Medical Condition | Relevant Findings and Potential Complications |
|---|---|
| Intussusception | Colicky pain, flexing of legs, fever, lethargy, vomiting, peak incidence in children at 6 months of age |
| Meckel’s diverticulum | Similar presentation to appendicitis, profuse GI bleeding, can develop to diverticulitis |
| Mesenteric adenitis | Can present like acute appendicitis, recurrent respiratory tract infections |
| Hirschsprung disease | Vomiting, abdominal distension, enterocolitis, primarily in first year of life |
| Small bowel obstruction | Bloating, vomiting, failure to pass flatus or stool, bilious emesis |
| Volvulus | Can present like small bowel obstruction, due to intestinal twisting |
| Large bowel obstruction | Abdominal distension, hard feces and rectal bleeding, can lead to bowel perforation |
| Necrotizing enterocolitis | Feeding intolerance, apnea, lethargy, bloody stools, abdominal distension and tenderness, abdominal erythema, bradycardia, primarily in premature infants |
| Peptic ulcer disease | Epigastric tenderness, pain related to eating a meal, ulcer can perforate |
| Viral hepatitis | Fever, malaise and jaundice, consider fecal-oral or vertical transmission |
| Acute pancreatitis | Steady and sudden-onset pain radiating to the back, nausea, vomiting |
| Splenic infarction | Personal or family history of sickle cell disease |
| Nephrolithiasis | Acute renal colic, flank pain radiating to groin |
| Testicular torsion | Testicular pain with acute onset, nausea, vomiting |
Laboratory Investigations
| Medical Condition | Relevant Diagnostic Tests |
|---|---|
| Constipation | None if history does not suggest an alternative diagnosis |
| Acute appendicitis | CBC (WBC normal or elevated), urinalysis, urine pregnancy |
| Gastroenteritis | Serum electrolytes, stool culture, stool for virology |
| Irritable bowel syndrome | None, based on history and clinical findings |
| Trauma | CBC for blood loss, abdominal CT with contrast |
| Celiac Disease | IgA |
| Inflammatory Bowel Disease | CBC, ESR/CRP, electrolytes, albumin, LFTs, Bilirubin, Stool culture, AXR |
| Urinary tract infection | Urine dipstick (for leukocyte esterase and nitrite), urine microscopy, urine culture (best if suprapubic aspirate) |
| Primary dysmenorrhea | None, based on history and clinical findings |
| Pneumonia and Empyema | CBC, Chest x-ray, sputum culture |
Red Flags in Abdominal Pain
Certain historical and examination findings should raise “red flags” that a severe life-threatening underlying abdominal process is present and prompt early triage to an emergency department.
Historical Red Flags
- Inability to maintain oral intake
- Projectile vomiting
- Overt gastrointestinal blood loss
- Syncope
- Pregnancy
- Recent surgery or endoscopic procedure
- Fever
- Caustic or foreign body ingestion
Physical Examination Red Flags
- Pathologic changes in vital signs
- Bloody, melenic stool
- Hernia (incarcerated and tender)
- Hypoxia
- Cyanosis
- Change in level of consciousness
- Jaundice
- Peritoneal signs
- Abdominal pain out of proportion to examination
Laboratory Red Flags
- Renal failure
- Metabolic acidosis
- Leukocytosis
- Elevated transaminases
- Elevated alkaline phosphatase and bilirubin
- Anemia or polycythemia
- Hyperlipasemia/hyperamylasemia
- Hyperglycemia/hypoglycemia
Radiography Red Flags
- Abdominal free air
- Gallbladder wall thickening
- Pericholecystic fluid
- Dilated biliary tree
- Bowel obstruction
- Dilated small bowel loops ± air fluid levels
- Intra-abdominal abscess
- Bowel wall thickening
- Air in the portal venous system
- Pneumatosis intestinalis
Indications for Surgical Consultation
- Severe or increasing abdominal pain with progressive signs of deterioration
- Bile-stained or feculent vomitus
- Involuntary abdominal guarding/rigidity
- Rebound abdominal tenderness
- Marked abdominal distension with diffuse tympany
- Signs of acute fluid or blood loss into the abdomen
- Significant abdominal trauma
- Suspected surgical cause for the pain
- Abdominal pain without an obvious etiology