Atopic Eczema
Dr Sami Billal - PhD, MD
Definition
-
AD is an itchy, chronic, relapsing, inflammatory skin condition.
-
Skin rash is characterized by itchy papules (occasionally vesicles in infants) which become excoriated and lichenified.
-
The eruption is associated with other atopic conditions in the individual or other family members
History
-
Ask about itching (no Atopic dermatitis without itching)
-
You have to ask about family or personal history of other atopic diseases as bronchial asthma ,rhinitis and hay fever
-
Ask about similar condition
Clinical Features
- Macular erythema, papules / papulo-vesicles
- crustations
- Lichenification and excoriation
- Dryness of the skin
- Secondary infection
Clinical features: Phases
- The type and distribution of the lesions varies with age:
- Infantile phase
- Childhood phase
- Adult phase
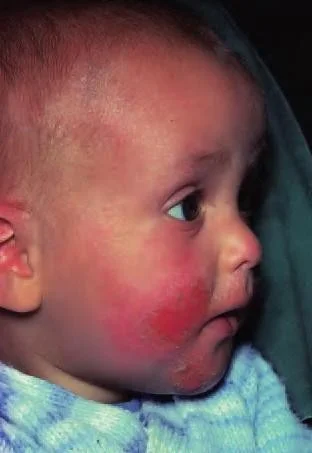
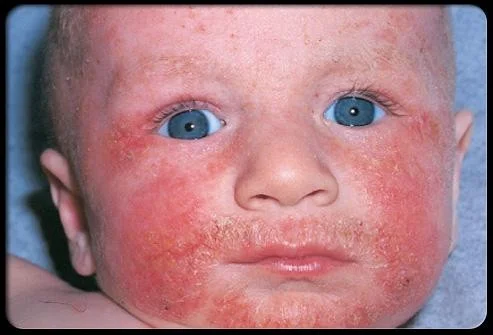
1. Infantile phase
-
From 2 months to 2 years
-
Site: Lesions usually start on the face (forehead, cheeks) - but may occur anywhere
-
The napkin area is usually spared
-
Extensor aspect of the knees, are most involved
-
Lesions consist of Erythema & oedematous papules
-
Intense itching
-
May become exudative & crusted
-
Secondary infection is not uncommon
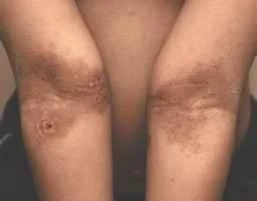
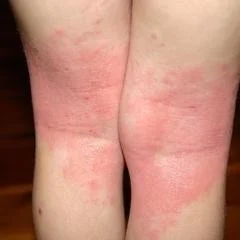
2. Childhood phase
-
From 2 years- 10 years
-
Site: Elbow and knee flexures (antecubital+ popliteal) sides of the neck, wrists and ankles
-
The erythematous and oedematous papules tend to be replaced by lichenification.
3. Adult phase
- Commonly the flexures of limbs and the back of neck (nape) are involved.
- Lichenification and excoriation
Management
- The aim is to:
- Decrease itching
- Improve sleeping and family interactions
- Improve school and work performance
Treatment
1- General advice
Education about AD.
Patients should be taught current knowledge of the disease, the types of trigger factors, the treatment options and their likely benefits and risks
2. Reduction of trigger factors
- Avoiding hot climate.
- Avoiding contact of wool with the skin (wearing cotton clothing).
- Aggravating foods (if the patient clearly identifies then).
- Stress aggravates atopic dermatitis (give simple reassurance).
3. Topical therapy
Bathing and emollients
- Bathing and immediate moisturizing is helpful
- Regular use of emollients will protect against inflammation.
- Emollients should be applied as frequent as possible throughout the day.
Topical corticosteroids
-
Are the predominant treatment for the inflammation of AD.
-
The strength and mode of application depends on the severity of the dermatitis, the sites to be treated, and the age of the patient.
-
Less potent topical steroids used on the: eyelids, face, axillae, groins and inner thighs.
-
Less potent topical steroids are used in children less than 1 year old (systemic absorption occurs, even 1% hydrocortisone ointment).
-
In infected or crusted dermatitis: steroid/antibiotic should be used
4. Systemic therapy
Antihistamines
-
H1-receptor antagonists are used for their sedative effect for nocturnal itching
-
Given 1 hour before bedtime.
-
Are best used in short courses (10-14 days)
-
Non-sedating antihistamines are of little value for the pruritus of atopic dermatitis.
Antibiotics
-
Exudation and pustule formation indicates staphylococcal infection.
-
Colonization of bacteria may exacerbate the dermatitis.
-
In Atopic Dermatitis , antibiotics may be helpful even if frank infection is not apparent.
-
Antibiotics as erythromycin are indicated.
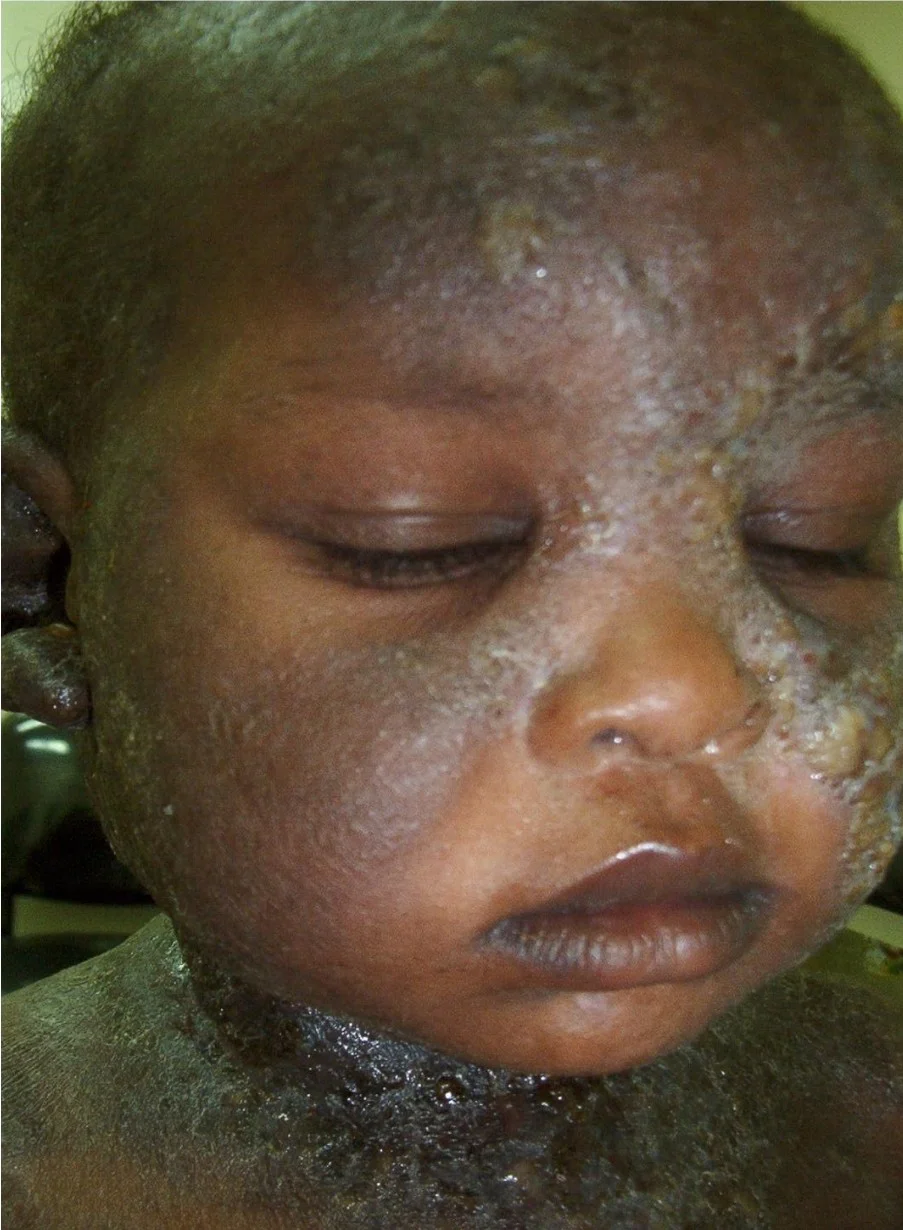
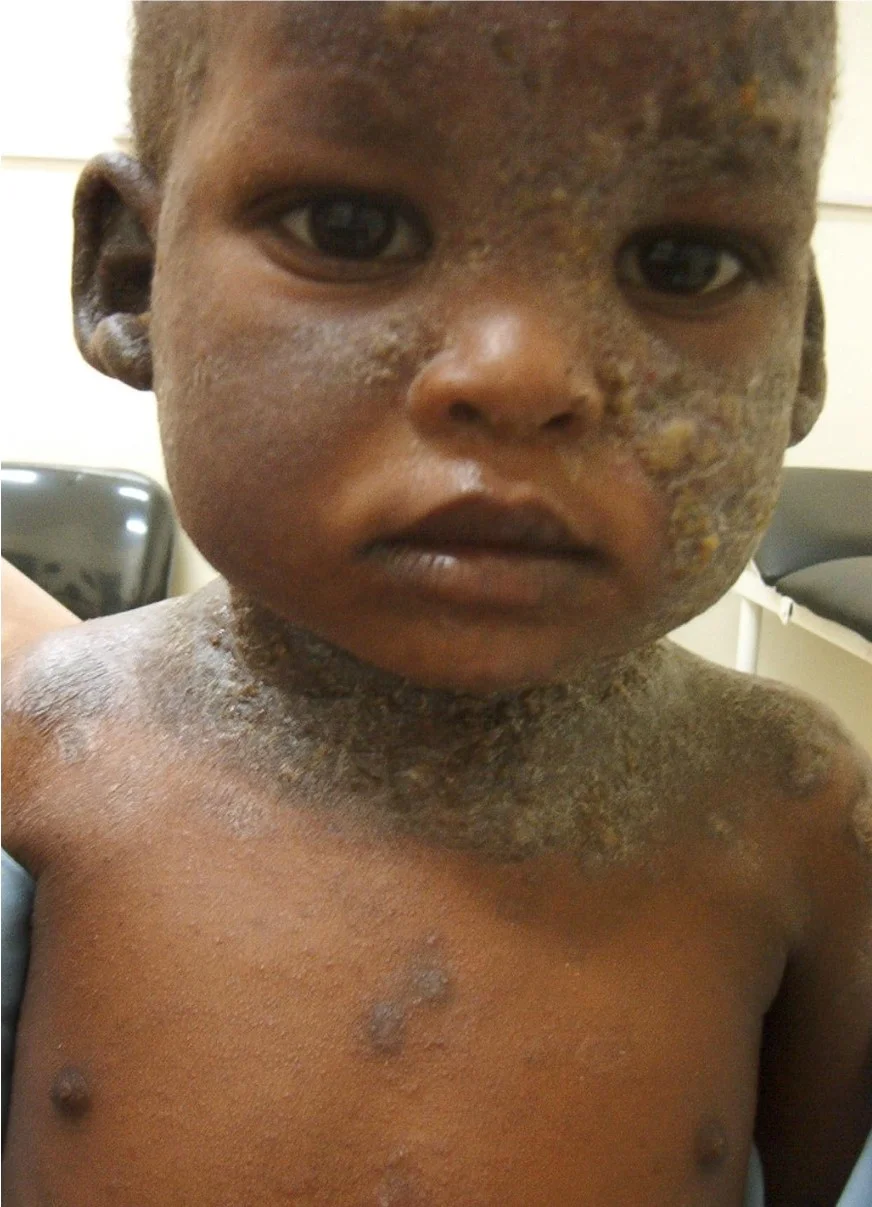
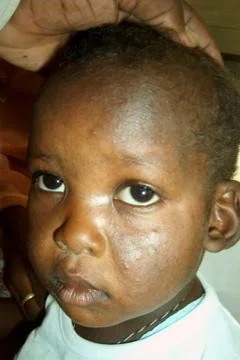
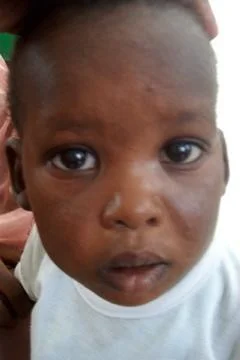
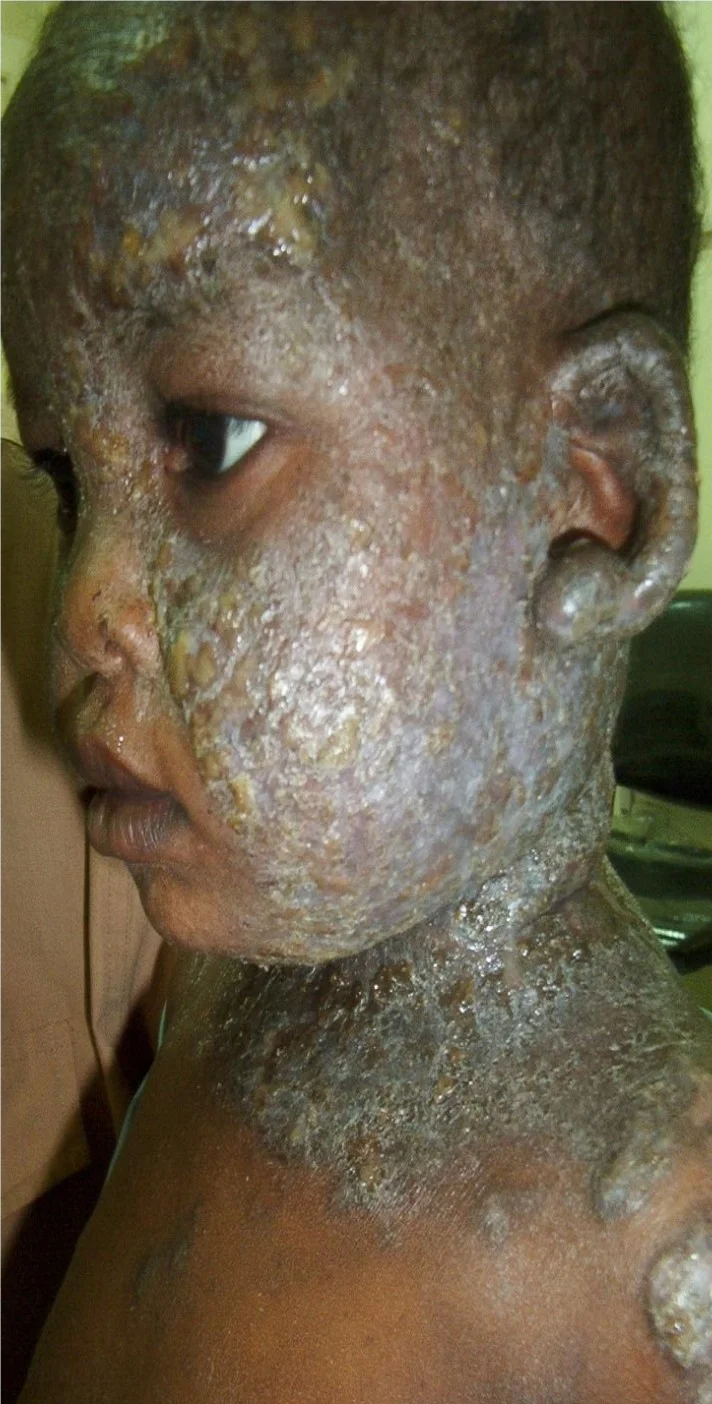
Complications of atopic dermatitis Z C
Case Three
Case Three: History
- HPI: Magid is a healthy 5-month-old boy whose mother reports a scaly rash on the face that she says he scratches. She wants to make sure it’s not infected.
- PMH: normal birth history
- Allergies: none
- Medications: none
- Family history: brother with asthma, mother with seasonal allergic rhinitis
- Social history: lives at home; does not attend daycare
- ROS: negative
Case Three: Skin Exam
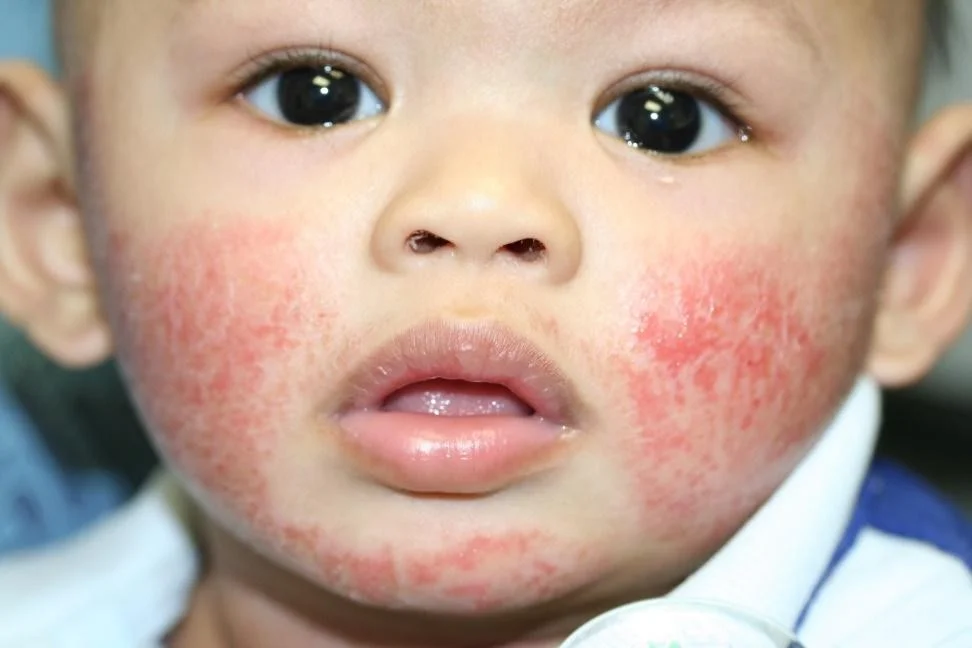
Case Three, Question 1
- What is the most likely diagnosis? a. Atopic dermatitis b. Bacterial cellulitis (more indurated and tender, not usually itchy or bilateral) c. Neonatal lupus (erythematous annular patches and plaques, usually periorbital) d. Tinea faciei (rare in infants, not symmetric) e. Seborrheic dermatitis (wrong distribution)
Atopic Dermatitis Basics
- Atopic dermatitis is a chronic, itchy, eczematous condition in patients with a personal or family history of atopy
- The “atopic triad” includes seasonal allergic rhinitis, asthma, and atopic dermatitis
- Distribution of involvement varies by age
- In infants and toddlers, eczematous plaques appear on the cheeks and chin and dorsal hands and feet
- Older children and adolescents develop more classic lichenified, eczematous plaques in flexural areas such as antecubital and popliteal fossae and posterior neck
- Itch is the primary symptom of atopic dermatitis
- Atopic dermatitis is often called “the itch that rashes”
Case Three, Question 2
- Which of the following treatments would you recommend to Magid’s parents? a. Astringent facial scrubs b. Clindamycin gel c. Hydrocortisone valerate ointment d. Ketoconazole cream e. Tretinoin cream
Treatment for Atopic Dermatitis
-
Patients with atopic dermatitis have a deficient lipid barrier that has to be replaced
- Emollients (moisturizers) are critical to treatment of the underlying dry skin of atopic dermatitis
- Atopic patients are sensitive to irritants, so recommend fragrance-free products and moisturizing soaps
-
Some patients have flares to irritants (wool clothes, etc.)
-
Food allergies may rarely exacerbate infantile atopic dermatitis
- If this is suspected, refer to allergist for a food antigen challenge
-
Topical corticosteroids are the mainstay of therapy for acute flares of atopic dermatitis
- Using stronger steroid for short periods and milder steroid for maintenance helps reduce risk of steroid atrophy
-
Antimicrobials may be needed for bacterial or viral infections that complicate atopic dermatitis
- Impetigo often complicates atopic dermatitis in infants, as does widespread herpes infections (eczema herpeticum)
-
Antihistamines are used for their sedative effect to control nighttime itching
-
Refer patients who do not respond to standard therapy, or have extensive involvement