Acute Glaucoma Case
Glaucoma
Case Presentation
A 56-year-old woman presented to the emergency department with sudden loss of vision OD (right eye), intense eye pain, headache, and vomiting. There was no history of any eye problems except for glasses for hyperopia. The visual acuity was counting fingers OD and 6/6 OS (left eye) - OU (bilateral). The right eye showed circumcorneal injection, diffuse corneal haze, shallow AC and a mid-dilated, fixed pupil.
Chief of complaint - Acute painful visual loss
Further Examination Findings
The lens was clear. The left eye was normal except for a shallow AC. The IOP was 46 mmHg OD and 14 mmHg OS. Fundus examination and gonioscopy OD were not possible because of the corneal haze. Examination of the OS revealed a normal CD ratio of 0.2, and gonioscopy OS revealed a narrow angle.
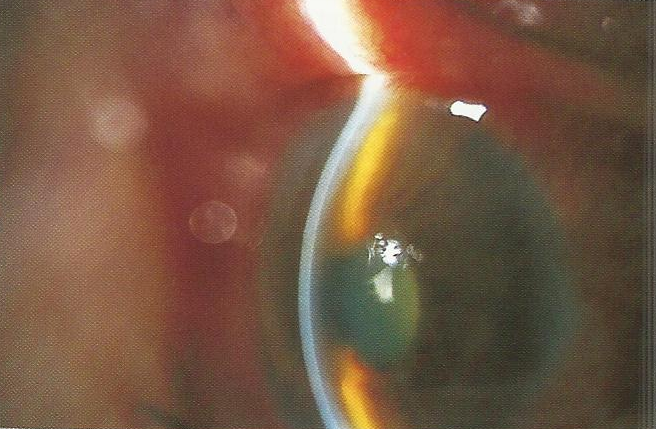
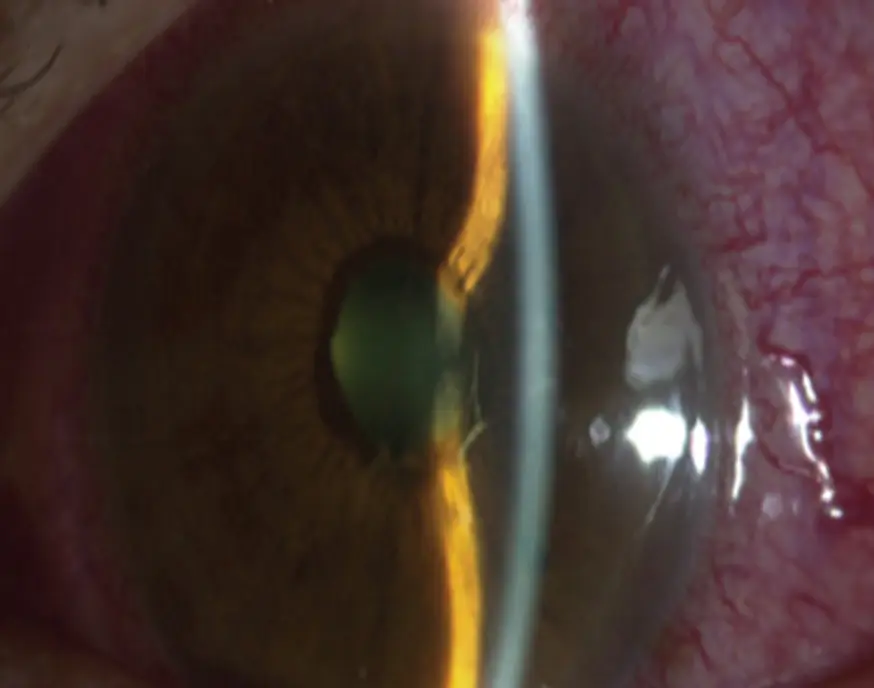
old age >40 diabetes myopia - narrow angle, ocoular pain, vomitting, mid dilated fixed pubil, gonioscopy shallow
1- What is diagnosis?
Acute congestive glaucoma (AACG) OR Acute closed angle glaucoma
2- differential diagnosis
- Keratitis
- Corneal ulcer
- Corneal FB
- Corneal wound
- Uveitis
- Orbital cellulitis
- Endophthalmitis or pan ophthalmitis
3- Clinical Examination & Investigations
Clinical Exam Full ophthalmic examination (VA, Visual field, Optic disc evaluation, Genioscopy, IOP measurement, Slit lamp examination, Gonioscopy) (Triad of glaucoma - IOP OD EX) NVL examination
Investigations
- ERG (Electroretinography)
- OCT
- Perimetry
4- Treatments
First thing Admission of patient Affected eye
- Cholinergic agents (such as pilocarpine) is given every 5 minutes in affected eye till pupil constricts.
- Topical beta-blocker and/or topical alpha-2 agonist to decrease IOP
- Oral carbonic anhydrase inhibitors and/or hyperosmotic agents if IOP more than 50 mmHg.
- Following resolution of the acute attack, definitive surgical treatment should be performed within 24 to 48 hours with the aim of achieving a persistently open angle.
Other eye -Yag Laser peripheral iridotomy
Clinical Features Y
Glaucoma
-
Age
-
History
-
Vomiting
-
Headache
-
Visual acuity
-
Ocular pain
-
IOP
-
Gonioscopy
-
Pupil
-
AC
-
CD ratio
-
Cornea
Chronic Glaucoma Case
Case Presentation
A 67-year-old farmer presented to the eye unit of a teaching hospital with a history of gradual, painless vision loss, and he was searching for his glasses change. History of headache, intermittent pain, redness. He is a cardiac patient and hypertensive 20 years ago. His presenting aided visual acuity was 6/60 in the right eye and 6/24 in the left eye. Both corneas were clear, and the pupils had a slow reaction to light. The right eye had a nuclear sclerotic cataract which precluded a good view of the optic nerve head, and a vertical cup :disc ratio (VCDR) of about 0.7, barely visible through the dilated pupil with the binocular indirect ophthalmoscope. The left eye VCDR was 0.5. Intraocular pressure (IOP) was 32 mmHg (right eye) and 27 mmHg (left eye) by applanation tonometry. Gonioscopy showed narrow angles in both eyes. Slit lamp examination shows atrophic iris patches. Patient was heavy smoker.
RT = 0.7
LT = 0.5’
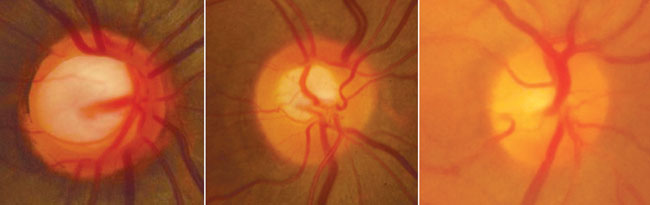
1- What is diagnosis?
Chronic narrow or open angle glaucoma
2- Differential diagnosis
- Cataract
- Error of refraction
- DR
- Retinitis pigmentosa
- Macular degeneration or dystrophy.
3- Clinical Examination & Investigations
Clinical Exam
- ophthalmic examination
- IOP measurement
- Gonioscopy
- Optic disc evaluation
- Visual field examination
Investigations
- OCT
- ERG
4- Treatments
To stop the progression of visual loss by lowering intraocular pressure (IOP).
-
Medical Therapy
- Topical medications:
- Beta blockers
- Alpha-2 agonists
- Oral medications:
- Carbonic anhydrase inhibitors
- Topical medications:
-
Laser Therapy
- Argon laser trabeculoplasty (if medical therapy is insufficient)
-
Surgical Intervention
- Filtering surgery: Trabeculectomy (if laser therapy fails)
- Drainage implant surgery: Valve implantation (if trabeculectomy fails)
Clinical Features Y
Glaucoma
-
Age
-
History
-
Headache
-
Visual acuity
-
Ocular pain
-
IOP
-
Gonioscopy
-
Pupil
-
AC
-
CD ratio
-
Cornea