BLEEDING DISORDERS
Prepared by: DR. SALMA ELGAZZAR
- MLO
- OSP6
- COSE Scenario

OBJECTIVES
- Recall the normal haemostasis.
- Classify bleeding disorders in pediatrics.
- Differentiate between platelet and coagulation defect based on the clinical presentation.
- Recognize the historical, physical and laboratory findings, and discuss the different treatment modalities in various coagulation disorders, including hemophilia, VWD and D.I.C.
Presentations
HEMOSTASIS
Hemostasis is a process to prevent and stop bleeding meaning to keep blood within a damaged blood vessel.
Stages of Hemostasis:
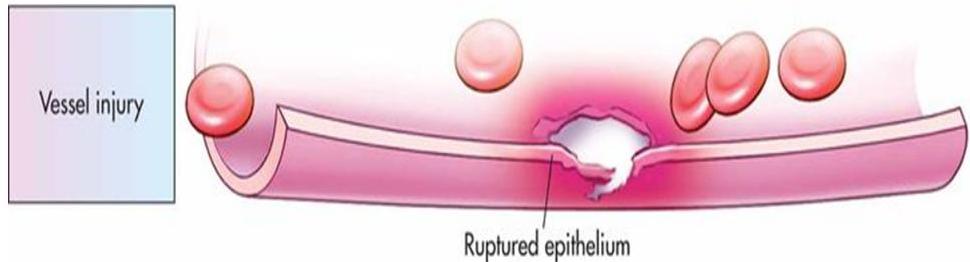
- Vessel spasm (Try hemostasis)
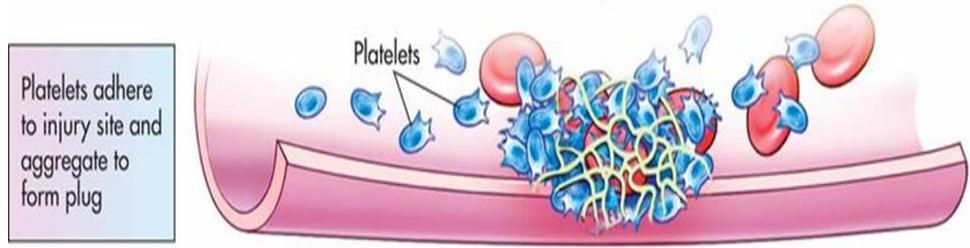
- Formation of the platelet plug
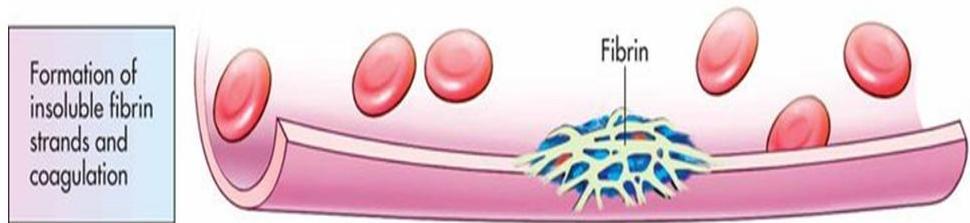
- Blood coagulation or development of insoluble fibrin
- Clot: Should be very stable in order to make sure the injured vessel is blocked once its formed and bleeding has stopped; should get rid of it to not form thrombus.
- Clot retraction.
- Clot dissolution (an important process).
Try hemostasis:
- When exposed to any injury there is always a balance between clot formation and dissolution.
- If there is imbalance, either bleeding or thrombus will occur.

CLOTTING FACTORS AND COAGULATION
Factor Identification
- Factor I: Fibrinogen
- Factor II: Prothrombin
- Factor III: Tissue Thromboplastin
- Factor IV: Calcium Ions (work in the Common Pathway)
- Factor V: Labile Factor
- Factor VII: Stable Factor
- Factor VIII: Antihemophilic Factor
- Factor IX: Christmas Factor, or Plasma Thromboplastin Component (PTC)
- Factor X: Stuart-Prower Factor
- Factor XI: Plasma Thromboplastin Antecedent (PTA)
- Factor XII: Hageman Factor
- Factor XIII: Fibrin Stabilizing Factor
Vitamin K Dependent Clotting Factors (1972): “Two plus seven is nine NOT ten!”


Coagulation Cascade
- Injury
- Primary hemostasis
- Secondary hemostasis (Coagulation Cascade)
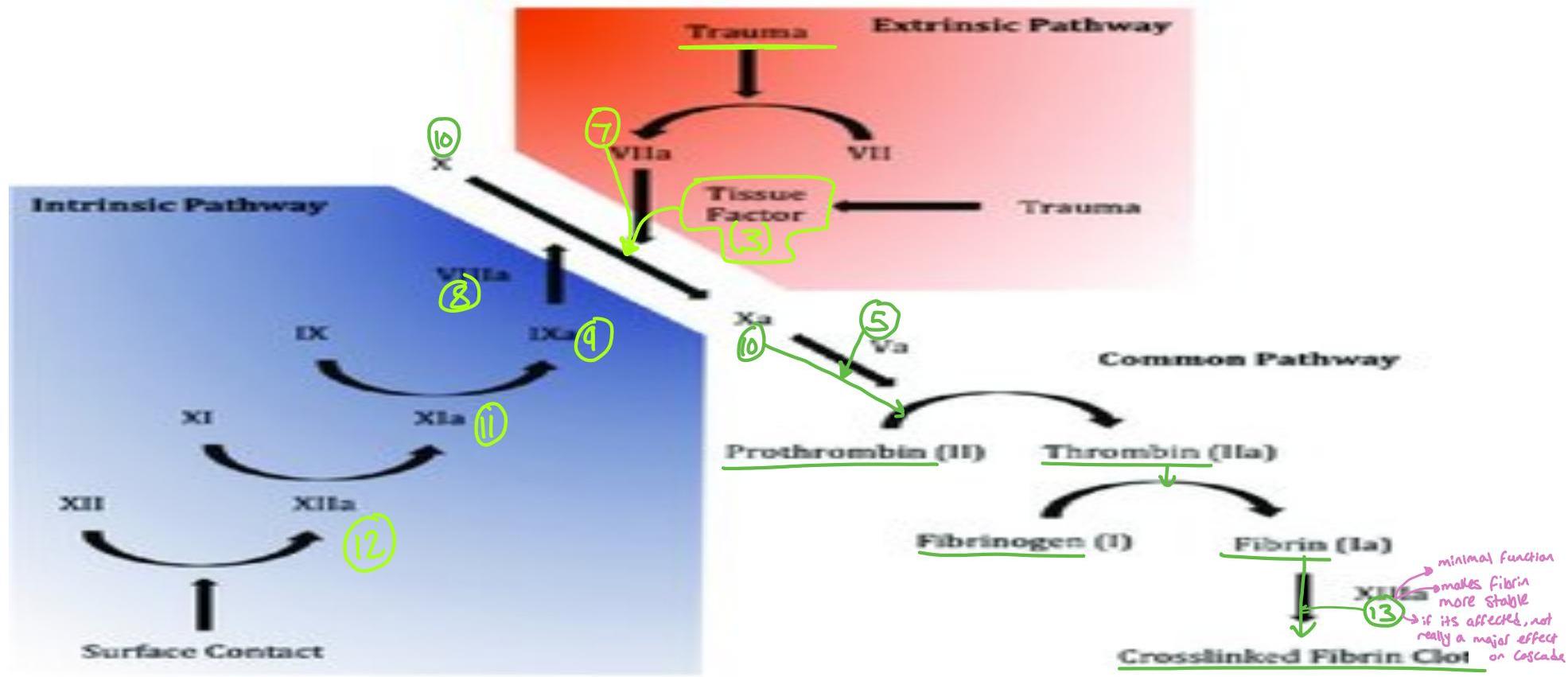
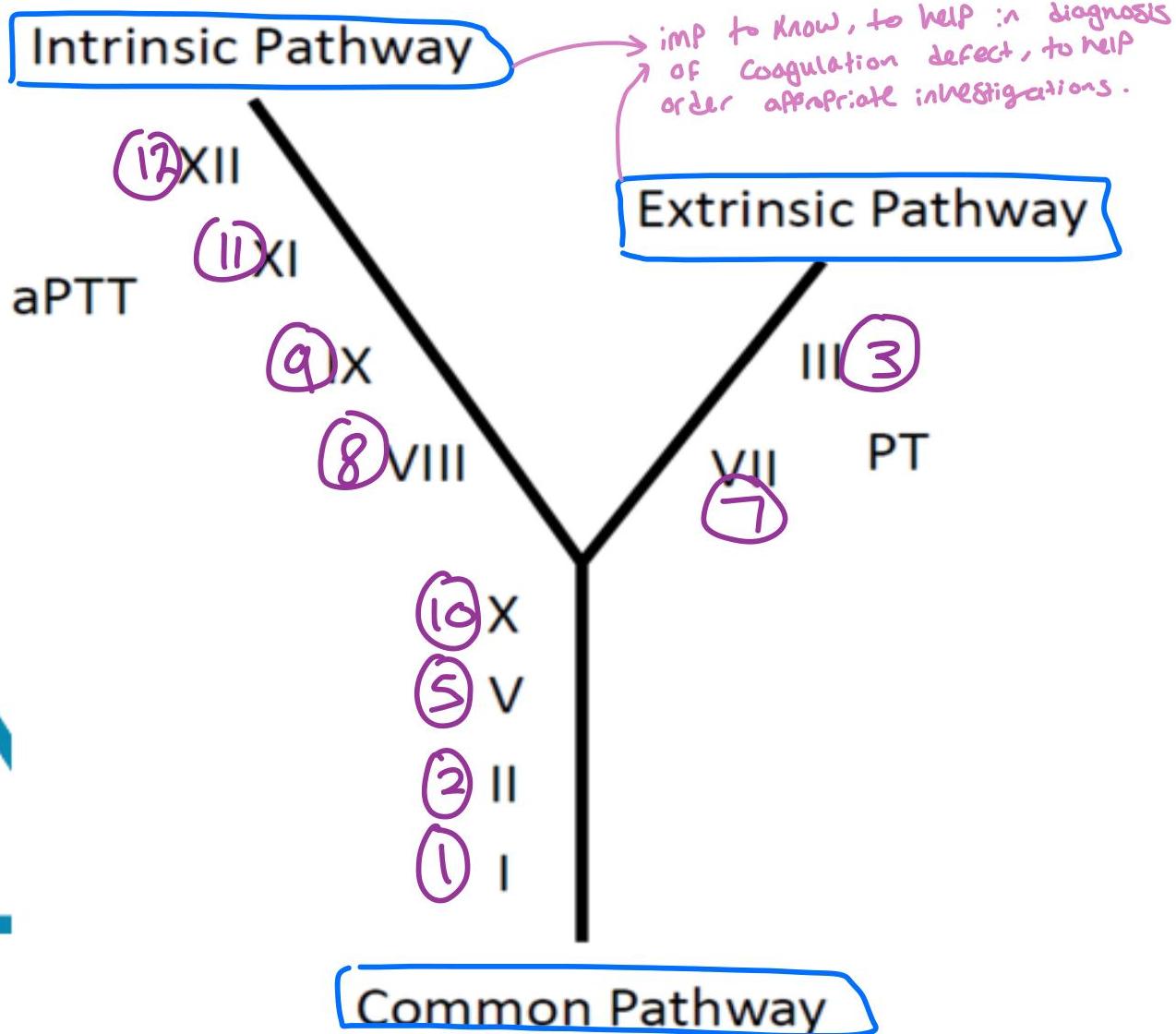
Pathway Defects and Screening:
-
Extrinsic Pathway:
- Involves Factors 7, 3, and 10.
- Defect prolongs Prothrombin Time (PT).
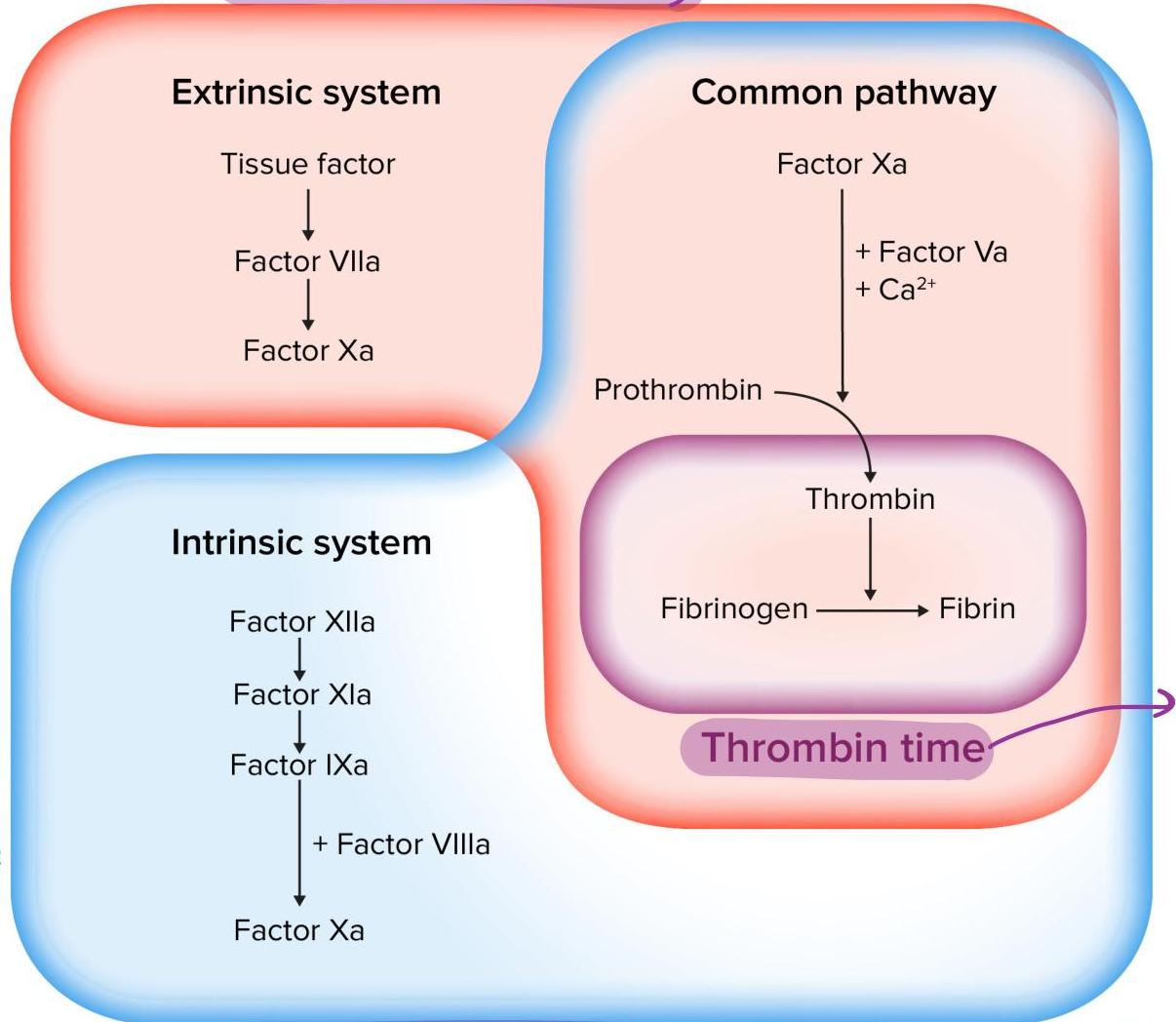
-
Intrinsic Pathway:
- Involves Factors 12, 11, 9, 8, and 10.
- Defect prolongs Activated Partial Thromboplastin Time (aPTT).
- Could be defect in all factors, some factors, or one factor.
-
Common Pathway:
- Prolonged if defect in Factor 10, Prothrombin, Fibrinogen, or Thrombin.

CLASSIFICATION OF BLEEDING DISORDERS
Disorders characterized by abnormal hemorrhagic tendency due to hemostatic defect:
- Coagulation defect
- Platelet defect
- Vascular defect
In disorders of primary hemostasis, platelet aggregation is impaired, whereas in disorders of secondary hemostasis it is the coagulation cascade that is impaired.
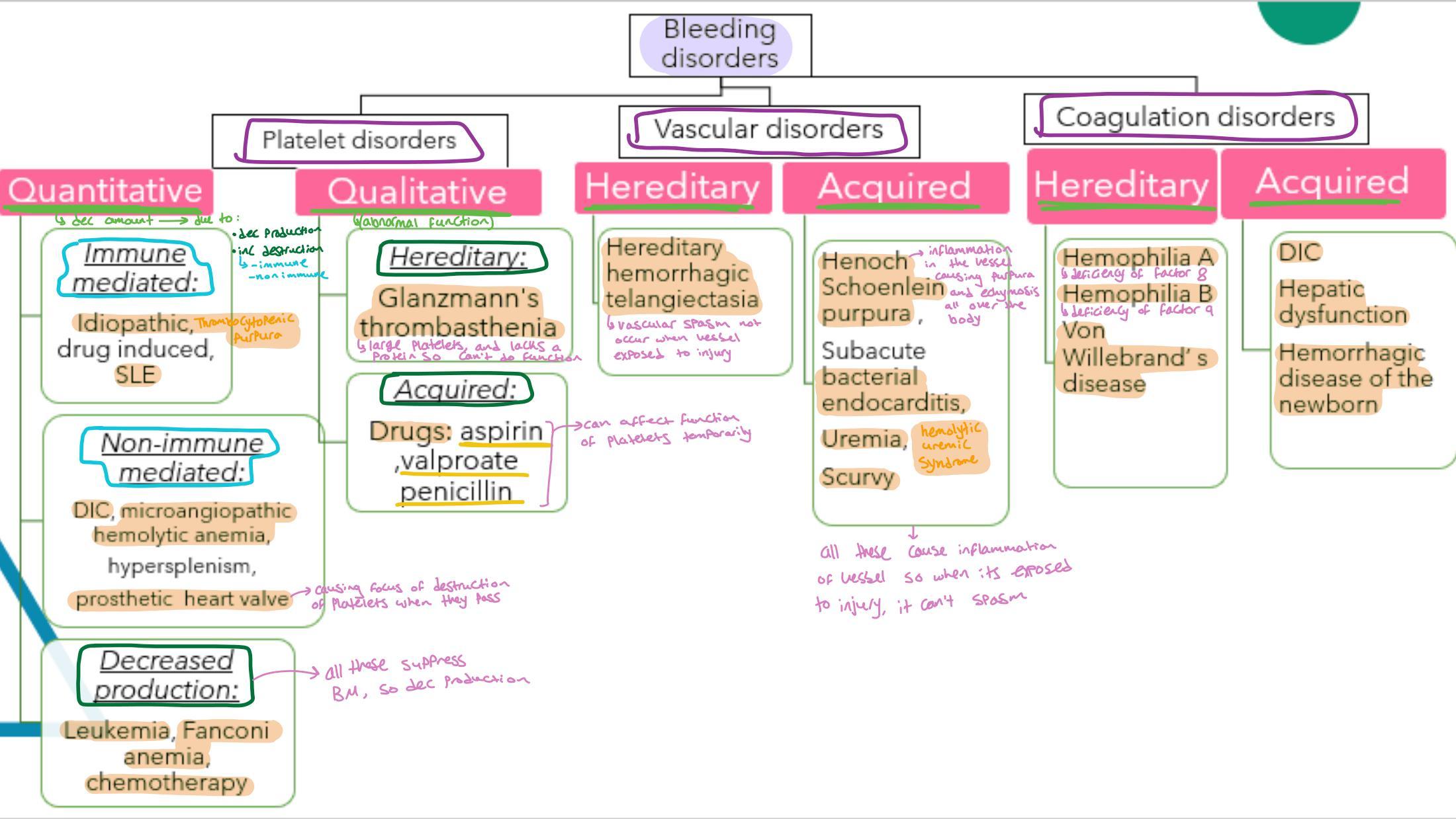
Platelet Disorders
Quantitative (Thrombocytopenia)
Decreased amount due to:
- Immune mediated: Idiopathic (ITP), drug induced, SLE.
- Non-immune mediated: DIC, microangiopathic hemolytic anemia, hypersplenism, prosthetic heart valve.
- Decreased production: Leukemia, Fanconi anemia, chemotherapy.
Qualitative (Thrombocytopathy)
Abnormal function:
- Hereditary: Glanzmann’s thrombasthenia (large platelets, lacks positive S-Ac function).
- Acquired: Drugs (aspirin, valproate, penicillin).
Coagulation Disorders
Hereditary
- Hemophilia A (deficiency of factor VIII)
- Hemophilia B (deficiency of factor IX)
- Von Willebrand’s disease
Acquired
- DIC
- Hepatic dysfunction
- Hemorrhagic disease of the newborn
Note: Developmental features like Hemoglobin, Hepatic issues, and Hypopituitarism were noted in clinical context.
CLINICAL DIFFERENTIATION
| BLEEDING CHARACTERISTICS | PLATELET DISORDERS | CLOTTING FACTOR DEFICIENCIES |
|---|---|---|
| Major sites of bleeding | Mucocutaneous (mouth, nose, GIT, urinary tract, menorrhagia) | Deep tissue (joints, muscles) or soft tissue hematomas (sneezes, etc.) |
| Petechiae | Common | Uncommon |
| Ecchymoses | Generally small and superficial. | May develop large ecchymoses deep. |
| Minor cuts | Excessive bleeding (platelets are the 100 specific melanomas) | Not usually |
| Surgery/Procedures | Often immediate; variable severity. (no excess bleeding with mild thrombocytopenia, severe bleeding with certain platelet function disorders such as GT) | Often delayed (Factor XIII) or during procedure. |
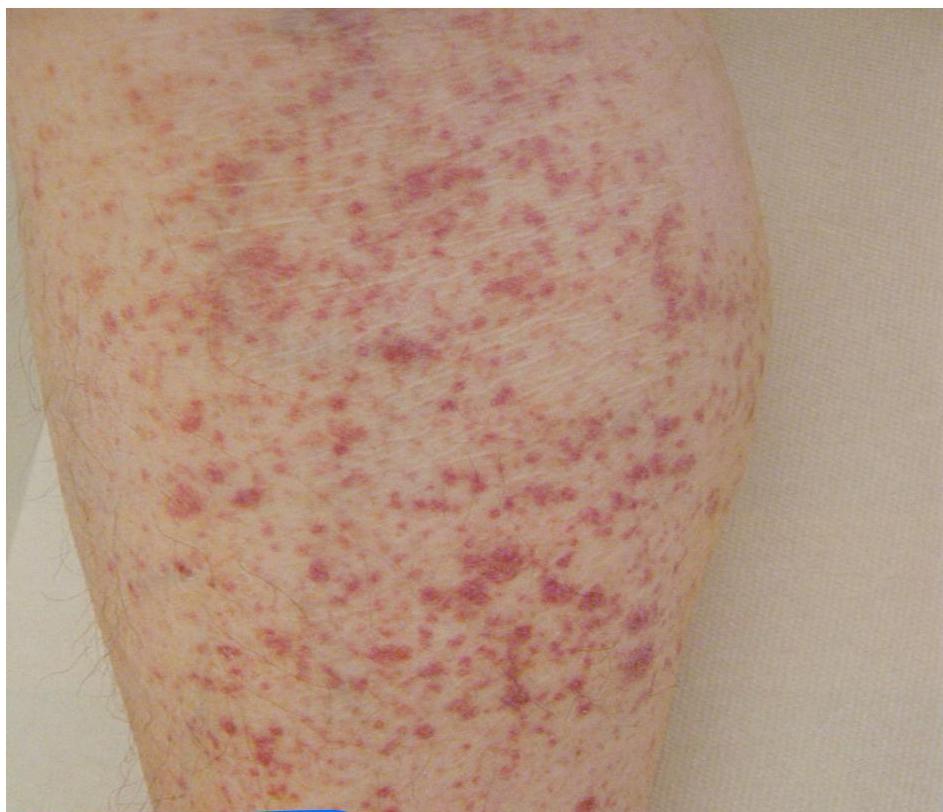 *Petechial bleeding (thrombocytopenia)
*Petechial bleeding (thrombocytopenia)
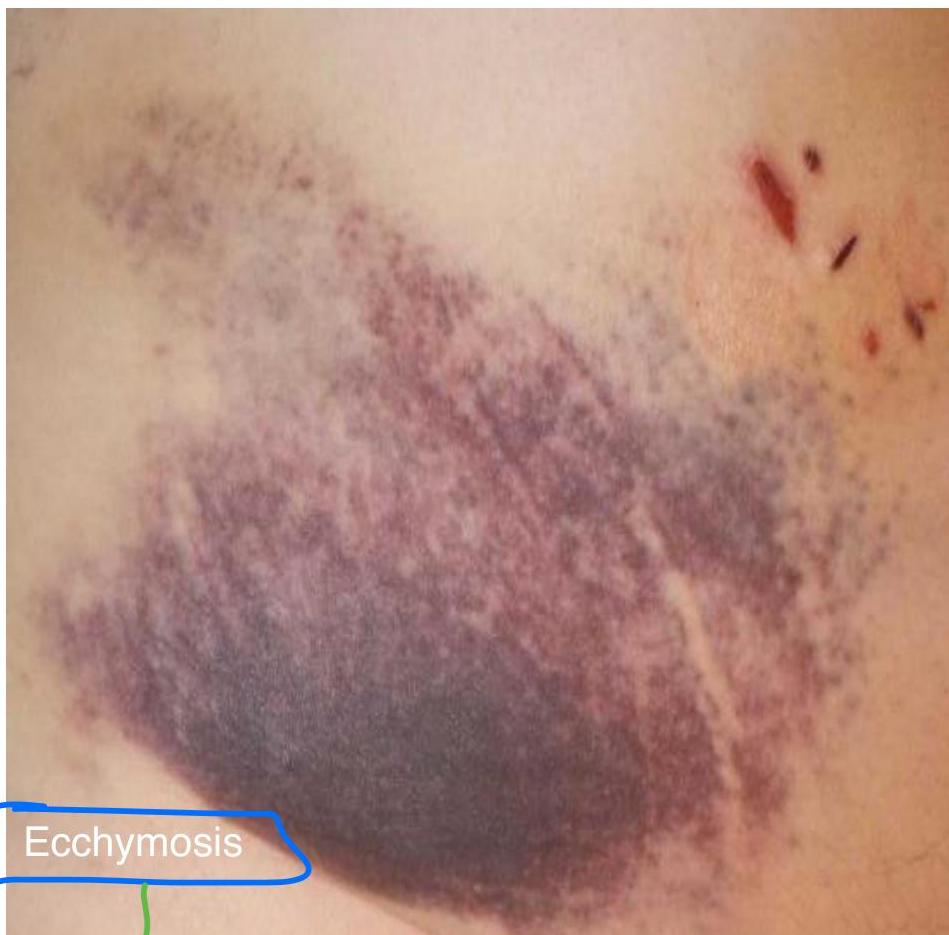 vs Ecchymosis (common in both).*
vs Ecchymosis (common in both).*