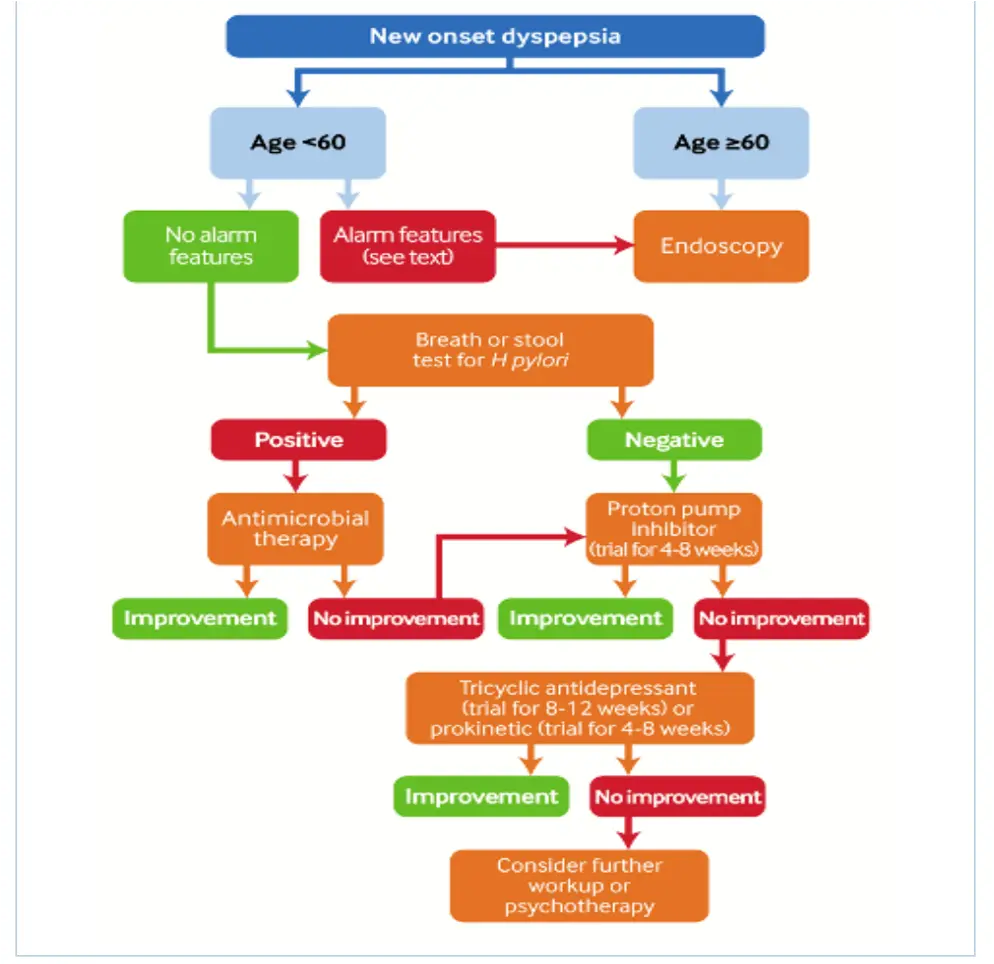
Approach to Patient with Dyspepsia
OBJECTIVES OF THE SESSION:
At the end of this session, students will be able to:
- Identify differential diagnosis of a case presented with the symptoms of dyspepsia.
- Differentiate between different causes of dyspepsia.
- Identify non-ulcer dyspepsia.
- Discuss briefly about Gastro-esophageal reflux disease (GERD).
- Describe peptic ulcer diseases.
- Identify importance of ALARM signs and symptoms in patients with dyspepsia.
- Investigate appropriately a patient with dyspepsia.
- Advise initial management plan for a patient with dyspepsia.
- Discuss non-drug management of GERD.
- Identify long term complications of dyspepsia.
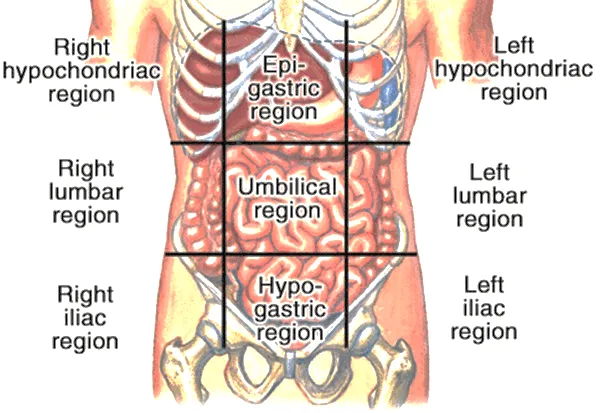
What is Dyspepsia?
Definition?
- Group of symptoms consist of:
- upper abdominal /epigastric pain
- or discomfort, heartburn,
- or acid regurgitation.
- Often associated with belching, bloating, nausea or vomiting.
FIVE COMMON DIAGNOSIS
- NUD 60-70%
- GERD 15-20%
- Gastritis
- Gastric Ulcer
- Duodenal Ulcer
Rare causes??
DRUGS ASSOCIATED WITH DYSPEPSIA
- NSAID
- Iron
- Metformin
- Codeine
- Digoxin
- Colchicine
- Alendronate
- Nitrates
- Antibiotic
- Orlistat
- Corticosteroid
- Theophyllin
- Quinidine
- Gemfibrozil
- Ca Antagonist
1. Functional Dyspepsia (non-ulcer) Most common functional gastrointestinal disorder.
-
Epigastric pain or discomfort, postprandial fullness Z, and early satiety within the last 3 months with symptom onset at least 6 months earlier.
-
Patients cannot have any evidence of structural disease to explain symptoms and predominant symptoms.
- Younger age group more than later life
- Causes?
- GI motility?
- Gastric secretion ⇔ normal
- Presence of H-Pylori
- Incidence decrease with advancing age
Possible Explanations of FD
- Motility abnormalities
- Visceral sensory abnormalities
- Psychological factors
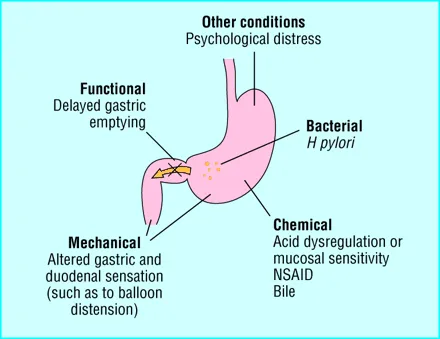 Other Conditions
Other Conditions
- Psychological distress Functional
- Delayed gastric emptying Mechanical
- Altered gastric and duodenal sensation
(such as to balloon distension) Bacterial - H pylori Chemical
- Acid dysregulation or mucosal sensitivity
- NSAID
- Bile
Diagnosis
When there is no evidence of structural disease and there have been at least three months of one or more of the following (with onset at least six months earlier):
- bothersome post-meal (postprandial) fullness
- early satiation
- epigastric pain
- epigastric burning
Management
A. Dietary and Lifestyle Modifications:
- Avoiding large portions at mealtime and eating smaller, more frequent meals is important to normalize upper gut motility
- Overweight individuals might find relief when they lose weight
- Quit smoking advice if available.
B. Resistant cases (failed initial treatment):
- Antacid
- Antispasmodic agent (such as mebeverine)
- H2 blocker or PPI
- Antidepressant (such as SSRI or tricyclic drug)
- Behavioral therapy or psychotherapy
- H pylori eradication
- No treatment is proved to be fully beneficial in these patients