IM
STEPWISE MANAGEMENT
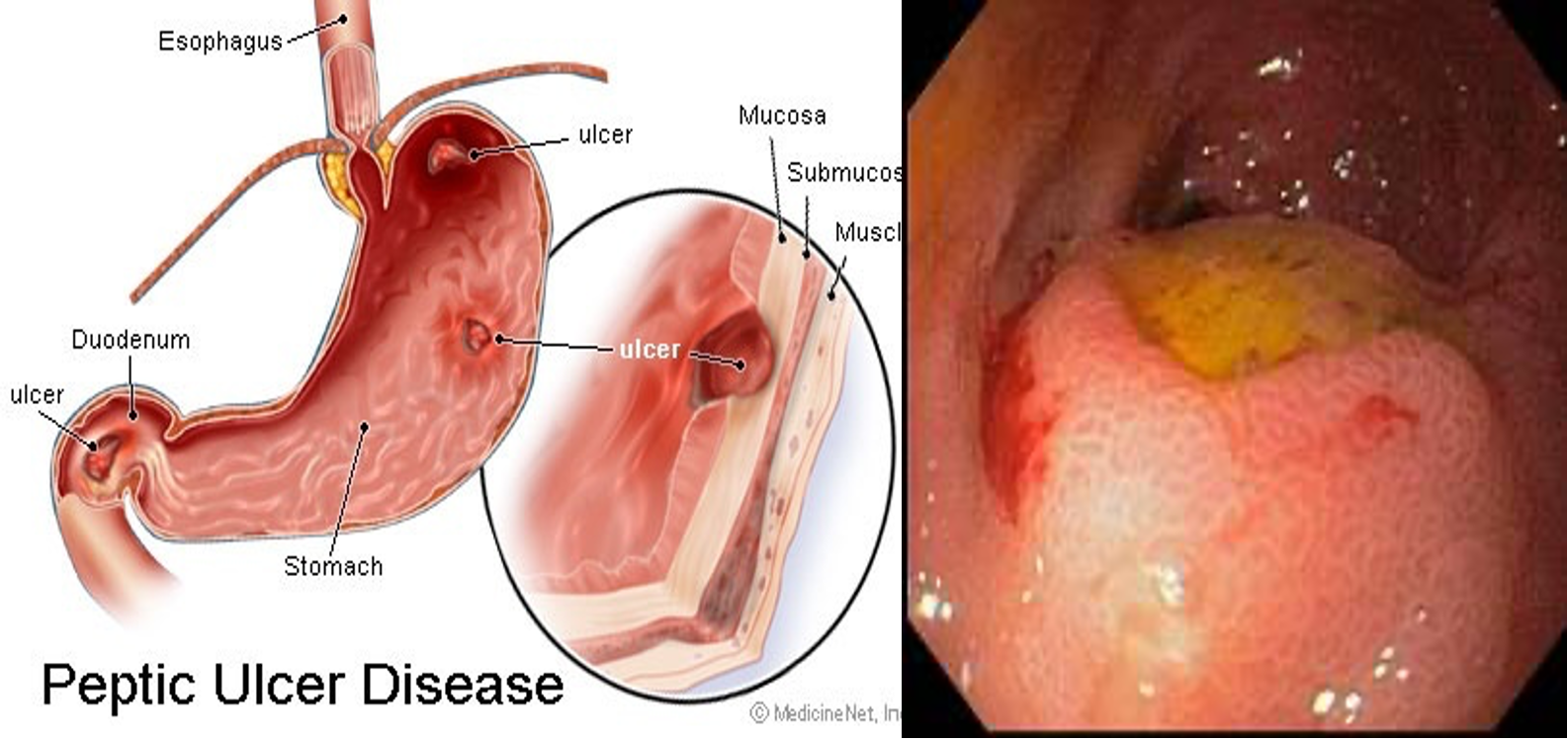
S/S SUGGESTING PEPTIC ULCER DISEASE
Patient less than 60 yrs. & no alarm symptoms( wt loss, dysphagia, hematemesis, melena) → Endosc. not LAAZIM. Check for H. pylori & treat. If neg., give PPIs for 1 month
If age more than 60 OR alarm symps. MOJOOD → endoscopy & H. pylori testing. Then treat accordingly
MANAGEMENT OF PUD
- Avoid smoking
- Avoid aspirin, NSAIDs and steroids
- No specific dietary restrictions but avoid things which cause hyperacidity (spices,caffiene)
MEDICAL TREATMENT
| Symptomatic | H. Pylori treatment |
|---|---|
| 1) Antacids (PPIs etc) 2) Mucosal protective agents | treat the pathogen directly |
MEDICINES For PUD
Antacids
- PPIs ( eg. omeprazole)
- H2 antagonists ( Zantac)
- Aluminium OH/Mg OH( tabs, liq) ( GAVISCON)
2) Mucosal protective agents ( Bismuth)
3) H. Pylori eradication meds.
1) Antacids
a) PPIs are the most effective & safest
- Omeprazole, es-omeprazole, pantoprazole
- Once daily before breakfast
- Usually given for 1 month to heal the ulcer, then stopped
- Long term use only in some patients
b) H2 receptor antagonists:
- Ranitidine( zantac), Nizatidine, famotidine
- Zantac has been withdrawn in the U.S.
c) Aluminium/Mg hydroxide: provides acute symptomatic relief of ulcer pain. ( Gaviscon tabs / syrup)
2) Mucosal protective agents (Bismuth) :
They “coat” the ulcer
3) Treatment of H. Pylori
Till recently, the following was the most common regimen used but now it is not the first line therapy:
Amoxicillin + Clarithromycin + PPI (all for 10 to 14 days)
FIRST LINE REGIMENS (American coll. of Gastroentero.)
QUADRUPLE THERAPIES 1) 14 Days
- PPI bid
- Bismuth tablets (4 times daily) (14 days)
- Tetracycline tabs( 4 times daily) (14 days)
- Metronidazole (Flagyl) tid (2 antacids + 2 antibiotics)
OR
2) 14 Days
- PPI (bid) (14 days)
- Amoxicillin(bid) (14 days)
- Flagyl
- Clarithromycin (1 antacid + 3 antibiotics)
HOW TO REMEMBER?
Patchi Chocolate For Ahmed
- P: PPI
- C: Clarithromycin
- F: Flagyl
- A: Amoxicillin
These regimens have a high eradication rate and low recurrence of symptoms After this treatment, continuous PPI treatment is not needed in most cases( some may need)
To confirm eradication, do one of these:
- a) Urea breath test after 1 month
- b) H. Pylori stool antigen test after 1 month
Failure to eradicate with these regimens or recurrence of symptoms may need other regimens or surgery Never use the same regimen twice
Ulcer prevention in special situations
Patients on long term NSAIDs, aspirin or corticosteroids → high risk of PUD → so, give prophylactic PPI & use gastroprotective NSAIDs( eg celecoxib)
Hospitalised patients → more chances of stress ulcers → so PPI routinely given
Surgery
Treatment:
Medical Measures
-
Cessation of smoking and intake of NSAIDs, steroids, etc.
-
A period of bed rest and a change to less stressful life style and small frequent meals without spices (i.e. No hurry, curry and warry).
-
Drug therapy: a. Antacid (liquid)—1, 2 and 3 hours after meal. b. H2 Blocker—Famotidine 40mg/day. c. Proton pump inhibitor—e.g. omeprazale 20mg/day. d. Cytoprotective agent, e.g. sucralfate, colloidal bismuth, etc.
Surgical Treatment:
Indications: Z
- Failure of medical treatment, i.e. failure of the ulcer to heal or recurrence, after rigid medical treatment (6 months for duodenal ulcer and 3 to 4 weeks for gastric ulcer).
- Appearance of complications, e.g. pyloric stenosis, repeated hemorrhage.
- Ulcer of > 5 years standing.
- Very large ulcers (> 5 cm size).
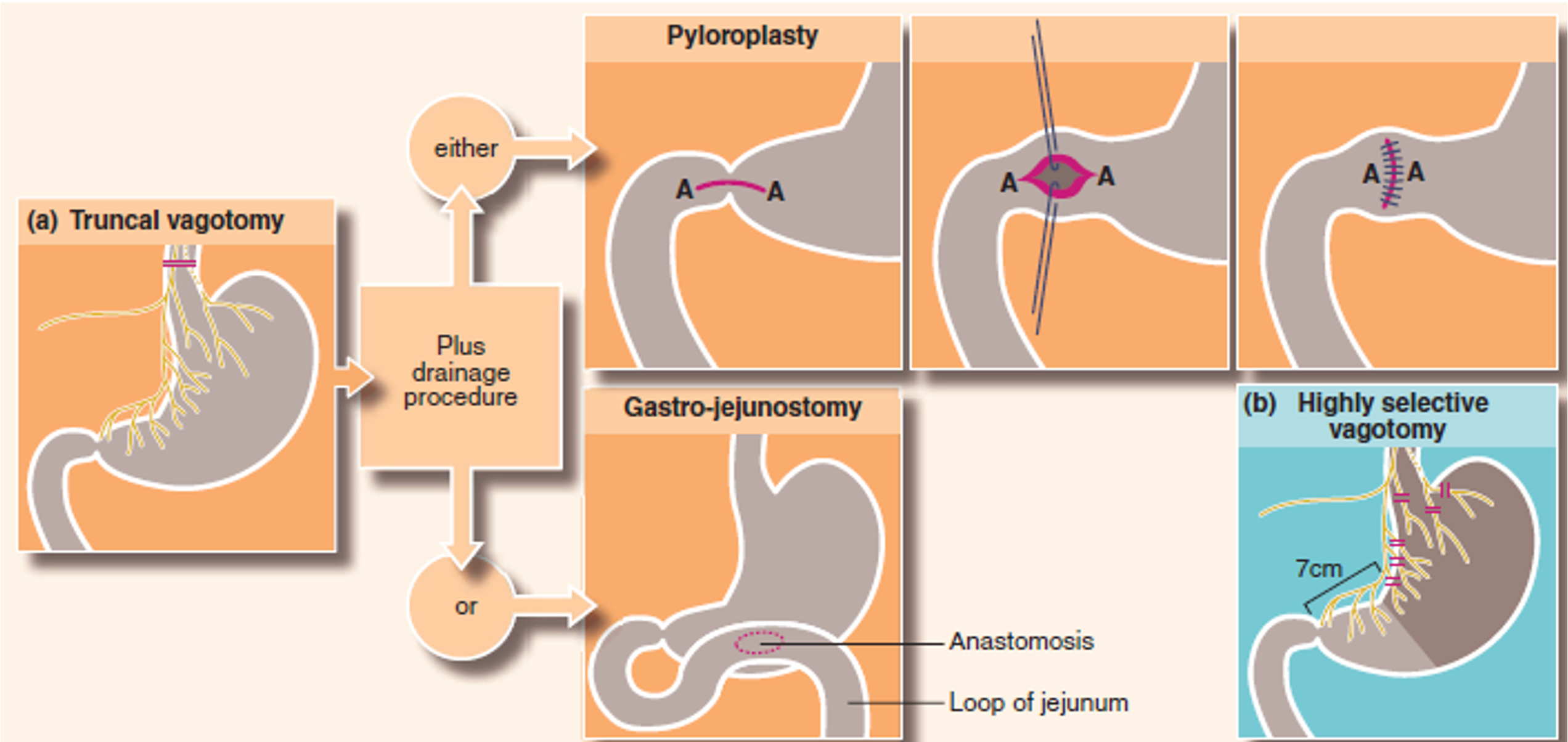
Type of operation: 5. Truncal vagotomy with a drainage procedure (TV + D) e.g. pyloroplasty or gastrojejunostomy.
-
Truncal vagotomy and antrectomy, bowel continuity is maintained by Billroth I or Billroth II anastomosis. Billroth II gastrectomy has higher mortality and morbidity.
-
Highly selective vagotomy (HSV) without any drainage procedure.
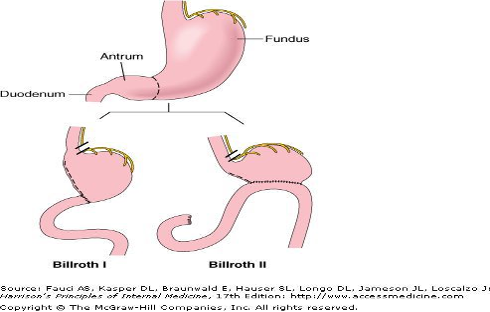 Billroth Z
Billroth Z
Treatment: GU
-
Medical treatment is effective and is the first line of approach for most patients. Surgery is usually reserved for cases where medical treatment fails or if there are complications such as bleeding, perforation, or obstruction.
-
Combined gastric ulcer + Duodenal ulcer, treatment of choice is partial gastrectomy that includes the entire antrum and the ulcer plus truncal vagotomy of both vagus nerves.
-
For gastric ulcer–Treatment is only partial gastrectomy (Billroth-1) that includes the entire antrum and the ulcer without vagotomy.
-
Billroth-I is preferred to Billroth-II operation if the duodenum is not badly deformed.
Complications of gastric ulcer:
-
Complications are same as in case of chronic duodenal ulcer. But bleeding occurs more commonly and perforation less frequently than duodenal ulcers.
-
An unusual complication of perforation is a gastrocolic fistula, when ulcers on the greater curvature penetrate the colon. Here surgical intervention is necessary.
-
Delayed healing, are more common in smokers than in non-smokers.
-
Obstruction
-
Weight loss
FM
Treatment Regimen
- Triple regimen:
- Proton pump inhibitor +
- Two antibiotics
Treatment of Peptic Ulcer Disease
The aims of management are to relieve symptoms, induce healing, and prevent recurrence.
All patients who are H.pylori-positive: eradication as primary therapy. PPI taken simultaneously with two antibiotics (from amoxicillin, clarithromycinand metronidazole) for 7 days.
First-line therapy is a proton pump inhibitor (12-hourly), clarithromycin 500 mg 12-hourly, and amoxicillin 1 g 12-hourly or metronidazole 400 mg 12-hourly, for 7 days.
Second-line therapy should be offered to those patients who remain infected after initial therapy once the reasons for failure of first-line therapy have been established. For those who are still colonised after two treatments, the choice lies between a third attempt with quadruple therapy (bismuth, PPI and two antibiotics) or long-term maintenance therapy with acid suppression.
Success is achieved in over 90% of patients, although compliance, side-effects and metronidazole resistance influence the success of therapy.
Helicobacter Eradication
- Eradication e.g., short-term triple therapy:
- Amoxicillin (2 x 1000 mg) for 7 days
- Clarithromycin (2 x 500 mg) for 7 days
- Omeprazole (2 x 20 mg) for 7 days

Eradication of H. Pylori
- Patients who are not allergic to penicillin:
- Standard dose PPI, clarithromycin, and amoxicillin for 10-14 days
- Patients who are allergic to penicillin:
- Standard dose PPI, clarithromycin, metronidazole for 10-14 days
- Patients who are allergic to penicillin or failed one course (above) of H. pylori treatment:
- Bismuth subsalicylate, metronidazole, tetracycline, standard dose PPI for 10-14 days
Patients who are not allergic to penicillin and have not previously received a macrolide Standard dose PPI (Lansoprazole 30 mg twice daily, omeprazole 20 mg twice daily, pantoprazole 40 mg twice daily, or rabeprazole 20 mg twice daily) twice daily (or esomeprazole 40 mg once daily) plus clarithromycin 500 mg twice daily, and amoxicillin 1000 mg twice daily for 10-14 days¶ Patients who are allergic to penicillin, and who have not previously received a macrolide or metronidazole or are unable to tolerate bismuth quadruple therapy Standard dose PPI twice daily, clarithromycin 500 mg twice daily, metronidazole 500 mg twice daily for 10-14 days Patients who are allergic to penicillin or failed one course (above) of H. pylori treatment Bismuth subsalicylate 525 mg four times daily, metronidazole 250 mg four times daily, tetracycline 500 mg four times daily, standard dose PPI twice daily for 10-14 daysΔ* Bismuth subcitrate 420 mg four times daily, metronidazole 375 mg four times daily, tetracycline 375 mg four times daily◊, standard dose PPI twice daily for 10-14 days*
Amboss Reference for Treatment
- General measures
- Nonpharmacological measures
- Follow-up
- H. pylori diagnostics
- Positive
- H. pylori eradication therapy with antibiotics and a PPI
- Continue acid suppression medication (i.e., PPIs) for 4–8 weeks.
- Negative: Trial of acid suppression medication (i.e., PPIs) for 4–8 weeks, followed by reevaluation
- Positive
Importance of H. Pylori Eradication
- H. pylori eradication is the cornerstone of therapy for peptic ulcers as this will successfully:
- Prevent relapse
- Eliminate the need for long-term therapy in the majority of patients
Benefits
- Cure rate
- Recurrence
- Bleeding
- All cases of dyspepsia ??
General Management
- Management of symptoms in primary care is appropriate for most patients rather than routinely seeking a pathological diagnosis.
- Alarm signals and signs are the major determinant of the need for endoscopy, not age on its own.
- Long-term care should emphasize patient empowerment with ‘on demand’ use of the lowest effective dose PPI.
Non-Drug Treatment
- Cigarette smoking cessation
- Aspirin and NSAIDs should be avoided
- Alcohol consumption to be stopped
- No special dietary advice is required
Lifestyle Advice
- Simple lifestyle advice:
- Healthy eating
- Weight reduction
- Smoking cessation
- Offer empirical antacid, H2A, or therapy for one month to patients with dyspepsia.
Reasons for Referral
- Cancer suspected or proven
- Diagnostic uncertainty
- Treatments not available
- Failure of treatment, symptoms persisting
- Patients’ wishes
Age Consideration
-
In patients aged 55 years and older with unexplained and persistent recent onset dyspepsia alone, an urgent referral for endoscopy should be made.
Indicated for patients with dyspepsia of any age with any of the following conditions:
- Chronic gastrointestinal bleeding,
- Progressive unintentional weight loss,
- Progressive difficulty swallowing,
- Persistent vomiting,
- Iron deficiency anaemia,
- Epigastric mass
- Suspicious barium meal.
Alarm Features – Absent
Two approaches are acceptable:
- Test for H. pylori infection
- Empiric Therapy
- A 4-week course of a histamine-2 receptor antagonist or PPI
Failure to respond to treatment justifies further investigation and/or referral.
Eradication therapy:
All patients with duodenal and gastric ulcers should have H. pylori eradication therapy. - There are several protocols for eradication but the most widely accepted is done by one week triple therapy including:
- Omeprazole (20 mg bid)+ Clarithromycin (500 mg bid) + Metronidazole (500 mg bid or amoxicillin (1 gm bid)
- NB: However recurrence is common.