TREATMENT
A. General Instruction
- Self-directed behavioral management program
B. Pharmacological
- Alpha-adrenergic blockers
C. Surgical
- Transurethral resection
A. GENERAL
-
Self-directed behavioral management program
- Limitation of fluids
- Bladder training focused on timed and complete voiding
- Treatment of constipation, which may help patients to regulate urinary symptoms.
- Fluid avoidance after dinner, limitation of caffeinated beverages, and avoidance of diuretics
-
Review of the patient’s medication list will help to identify opportunities to modify or avoid medications that may impact symptoms of BPH.
SPECIFIC TREATMENT
A. Pharmacological
- Alpha-adrenergic blockers:
- Terazosin, Doxazosin, Tamsulosin, Alfuzosin, Silodosin
- 5 alpha-reductase inhibitors
- Finasteride, Dutasteride
- Phosphodiesterase type 5 inhibitor:
- Tadalafil
B. Surgical
- Transurethral resection of the prostate or others
PHARMACOLOGICAL TREATMENT
-
Alpha-adrenergic blockers:
- For patients with mild to moderate obstructive symptoms, decreases voiding problems.
-
5 alpha-reductase inhibitors:
-
Reduces prostate size, decreasing voiding problems over months, especially in patients with larger (> 30 mL or even >40 mL) glands.
-
A combination of both classes of drugs is superior to monotherapy.
-
-
Phosphodiesterase type 5 inhibitor:
- For men with concomitant erectile dysfunction, daily tadalafil may help relieve both conditions.
SURGICAL TREATMENT Y
Indications:
- No response to drug therapy
- Develop complications: 3. Recurrent UTI, Renal stones 4. Severe bladder dysfunction 5. Upper UTI
Transurethral resection of the prostate (TURP) is the standard.
-
Erectile function and continence are usually retained, although about 5 to 10% of patients experience some postsurgical problems, most commonly retrograde ejaculation.
-
The incidence of erectile dysfunction after TURP is between 1 and 35%. About 10% of men undergoing TURP need the procedure repeated within 10 years because the prostate continues to grow.
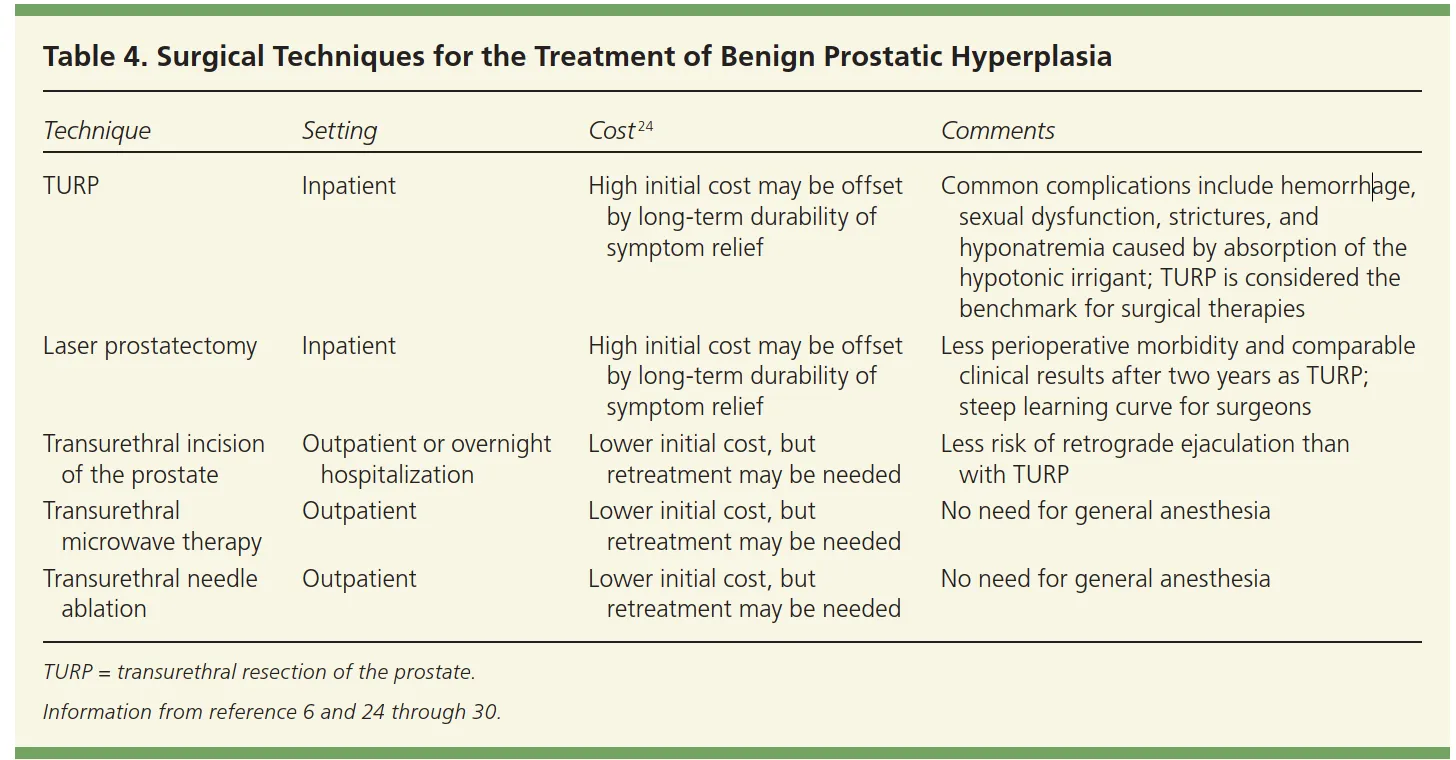
Surgical Techniques for the Treatment of Benign Prostatic Hyperplasia Y
| Technique | Setting | Cost | Comments |
|---|---|---|---|
| TURP | Inpatient | High initial cost may be offset by long-term durability of symptom relief | Common complications include hemorrhage, sexual dysfunction, strictures, and hyponatremia caused by absorption of the hypotonic irrigant; TURP is considered the benchmark for surgical therapies |
| Laser prostatectomy | Inpatient | High initial cost may be offset by long-term durability of symptom relief | Less perioperative morbidity and comparable clinical results after two years as TURP; steep learning curve for surgeons |
| Transurethral incision of the prostate | Outpatient or overnight hospitalization | Lower initial cost, but retreatment may be needed | Less risk of retrograde ejaculation than with TURP |
| Transurethral microwave therapy | Outpatient | Lower initial cost, but retreatment may be needed | No need for general anesthesia |
| Transurethral needle ablation | Outpatient | Lower initial cost, but retreatment may be needed | No need for general anesthesia |
TURP = transurethral resection of the prostate.
Information from reference 6 and 24 through 30.
Other Procedures Y
- Alternatives to TURP include:
- Microwave thermotherapy
- Electrovaporization
- Various laser techniques
- High-intensity focused ultrasonography
- Transurethral needle ablation
- Radiofrequency vaporization
- Pressurized heated water injection therapy
- Urethral lift
- Steam injection therapy
- Intraurethral stents
Urinary Retention
- Significant urinary retention requires immediate decompression.
- Passage of a standard urinary catheter is first attempted.
COMPLICATIONS OF LONG STANDING BPH
- Acute urinary retention
- Recurrent UTI
- Renal stones
- Severe bladder dysfunction
- Upper UTI
URGENT REFERRAL INDICATIONS
to UROLOGY
Clinical Indicators
- Microscopic or macroscopic hematuria
- Neurological disease (such as long-standing diabetes): may suggest neurogenic bladder
- H/O prior urological surgeries and urethral stricture
- History of recurrent infection
- Palpable bladder
- Renal impairment due to lower urinary tract dysfunction
- Abnormal digital rectal exam suggesting prostate cancer
- Abnormal PSA levels.
SUMMARY OF THE MANAGEMENT PLAN
Benign Prostatic Hyperplasia (BPH) Management Guidelines
Key Recommendations for Practice
Clinical Recommendations
- Men with suspected BPH can be evaluated with a validated questionnaire to quantify symptom severity.
- In men with symptoms of BPH, a digital rectal examination and urinalysis should be performed to screen for other urologic disorders.
- Watchful waiting with annual follow-up is appropriate for men with mild BPH.
- Alpha blockers provide symptomatic relief of moderate to severe BPH symptoms.
- In men with a prostate volume greater than 40 mL, 5-alpha reductase inhibitors should be considered for the treatment of BPH.
- Refer patients for a surgical consultation if:
- Medical therapy fails.
- The patient develops refractory urinary retention, persistent hematuria, or bladder stones.
- The patient chooses primary surgical therapy.
BPH = benign prostatic hyperplasia.
Evidence Rating System:
- A = consistent, good-quality patient-oriented evidence
- B = inconsistent or limited-quality patient-oriented evidence
- C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series
For information about the SORT evidence rating system, see page 1360 or www.aafp.org/afpsort.xml.

Tables
Table 1: Differential Diagnosis of Lower Urinary Tract Symptoms in Men
| Clinical Finding | Possible Diagnosis |
|---|---|
| Abnormal sphincter tone | Neurogenic bladder |
| Fever | Prostatitis |
| Hematuria | Bladder cancer |
| Prostate nodule or induration | Prostate cancer |
| Prostate tenderness | Prostatitis |

Table 2: Medications and Medical Conditions That May Contribute to Lower Urinary Tract Symptoms in Men
| Factor | Mechanism |
|---|---|
| Medications | |
| - Antihistamines | Decreased parasympathetic tone |
| - Decongestants | Increased sphincter tone via alpha₁-adrenergic receptor stimulation |
| - Diuretics | Increased urine production |
| - Opiates | Impaired autonomic function |
| - Tricyclic antidepressants | Anticholinergic effects |
| Medical Conditions | |
| - Bladder cancer | Mechanical obstruction |
| - Congestive heart failure | Diuresis |
| - Diabetes | Osmotic diuresis, autonomic neuropathy |
| - Parkinson’s disease | Autonomic neuropathy |
| - Prostate cancer | Mechanical obstruction |
