Recommendations for HTN Screening
- Class
- Recommendation
- Screening for hypertension is recommended for all adults (>18 years of age) at each visit to a healthcare facility, whenever feasible.
- Annual screening is recommended for individuals older than 40 years of age or those who have risk factors for hypertension.
- Screening for the general population is recommended every 3 to 5 years.

How to Measure BP?
-
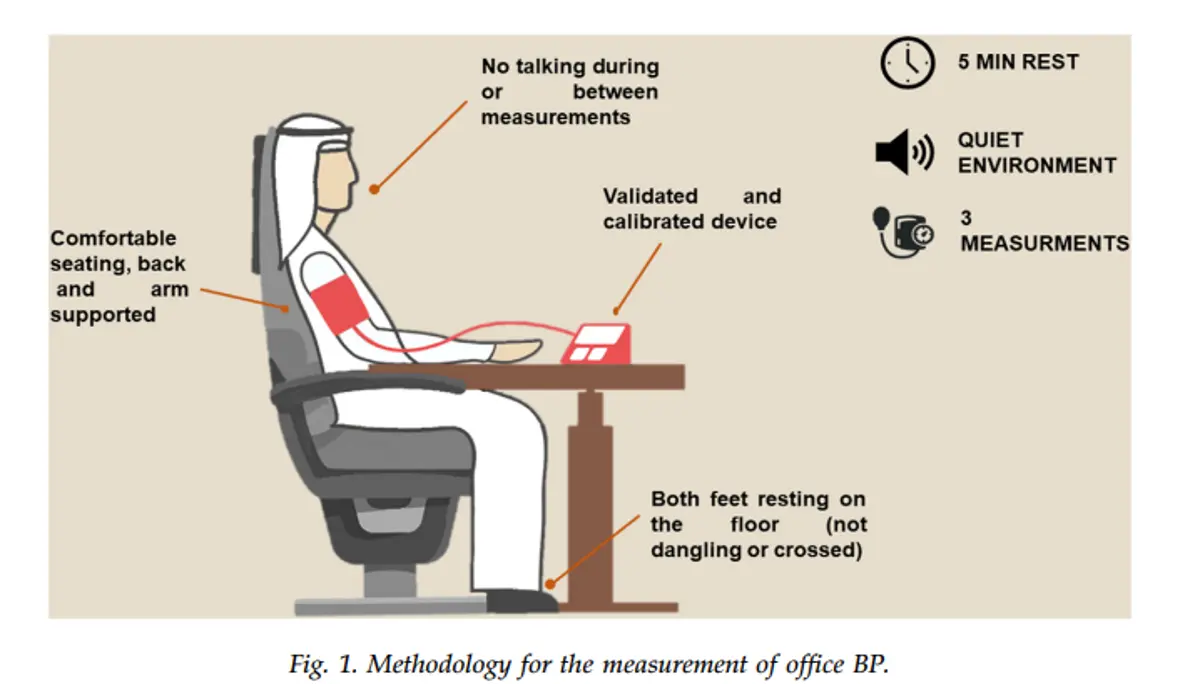
No talking during or between measurements
-
5 MIN REST
-
QUIET ENVIRONMENT
-
3 MEASUREMENTS
-
Comfortable seating, back and arm supported
-
Both feet resting on the floor (not dangling or crossed)
Validated and calibrated device
Fig. 1. Methodology for the measurement of office BP. OSPE
Standards for BP Measurement
For a reliable and valid BP measurement, it is essential to uphold the following standards:
I. Patient-Related Standards
-
Patient should have 3–5 minutes of physical rest before measuring BP.
-
Patient should relax (legs should not be crossed) in a quiet environment (no talking) before measurement.
-
BP should be measured in sitting position with back support.
-
BP measurement should be taken in both arms at initial visit. The arm with the higher BP values should be noted in the chart and follow up should be performed on this arm.
-
Upper arm should not be covered by clothing.
-
Elbow should be supported and cuffed at heart level.
-
BP should be measured in standing position, if postural hypotension is suspected (e.g., diabetics and elderly patients).
-
Patient should avoid nicotine and caffeine one hour before BP measurement.
-
Patients should avoid BPM while the urinary bladder is distended.
II. Equipment-Related Standards Z OSPE
-
Appropriate cuff size: The cuff bladder should encircle 80% of the arm, and the cuff width should be 40% of the arm circumference.
-
Correct cuff position:
- a. distance of 2.5 cm (2 fingers) should be maintained between the lower end of the cuff and the antecubital fossa.
- b. Cuff bladder should be centered over the brachial artery.
- c. Cuff should be wrapped around the upper arm, firmly in contact with the arm, but not too tight and not too loose, allowing 2 fingers to be put under the cuff comfortably.
-
Correct stethoscope position:- The bell orifice of the stethoscope should be placed just above and medial to the antecubital fossa but below the edge of the cuff. The stethoscope bell orifice should not touch the cuff bladder or tubing.
-
Correct manometer position: (for mercury BPM) The position of the mercury manometer should be upright at examiner’s eye level, and at zero level.
III. Examiner-Related Standards
- Inflate the cuff bladder rapidly to 30 mm Hg above the level of the estimated SBP.
- Apply mild pressure on the stethoscope bell (steadily and gently, without excessive pressure).
- Deflate the cuff bladder pressure at the rate of 2 mm Hg/sec.
- Deflate the cuff bladder rapidly and completely at DBP to avoid venous congestion.
- Avoid reinflation and correction of stethoscope position during the measurement.
- BP should be measured at least twice at each visit and the mean value documented.
- Record SBP and DBP immediately, rounded off to 2 mm Hg.
- Repeat BP measurement if necessary after a break of 1 min.
- BP measurements should always be associated with measurement of heart rate.
Home Blood Pressure Monitoring (HBPM)
- HBP may be used for both diagnosis and monitoring of BP.
- Home SBP values ≥135 mmHg or DBP values ≥85 mmHg should be considered as elevated.
- Home BPM should be based on duplicate measurements (one minute apart), morning and evening, for an initial 7-day period. First-day home BP values should not be considered.
- SHMS strongly supports the use of HBPM as adjunctive in hypertension follow-up. It is cost-effective and improves adherence and control.
Ambulatory BP Monitoring (ABPM)
-
It is performed by a validated automated device over a period of 24 hours.
-
BP is measured at repeated intervals (every 15–30 mins while awake, and every 30–60 mins during sleep).
-
The patient is instructed to engage in normal activities but to refrain from strenuous exercise and, at the time of cuff inflation, to stop moving and talking and keep the arm still with the cuff at heart level.
Blood Pressure Guidelines
-
At least 70% of BPs during daytime and nighttime periods should be satisfactory.
-
ABPM is a more sensitive risk predictor of CV outcome than is office BPM.
-
The incidence of CV events is higher in non-dippers.
-
Normal average daytime BP is <135/85 mm Hg.
-
Nocturnal BP is 10%–20% less than the average daytime BP (<120/75 mm Hg).
-
A 24-hour average value of 130/80 mm Hg corresponds to a 140/90 mm Hg of office value.
-
Possible reasons for the absence of dipping are: - Non Dippers ±±±
- sleep disturbance
- obstructive sleep apnea (OSA)
- CKD
- obesity
Indications for ABPM
- Suspected white-coat HTN
- Confirm diagnosis, if available
- Suspected masked HTN
- Resistance to drug therapy
- Suspicion of nocturnal HTN
- Obstructive sleep apnea
- Assessing hypertension in children and adolescents
- Assessing hypertension in pregnancy
- Assessing hypertension in high-risk patients
- Suspected drug-induced hypotension
- Assessment of BP variability
- Assessing hypertension in the elderly
How to Diagnose Hypertension?
- Should be based on the average of two or more readings taken at each of two or more clinical encounters
- The funduscopic examination.
- Cardiopulmonary examination.
- Peripheral vascular examination can detect evidence of atherosclerosis.
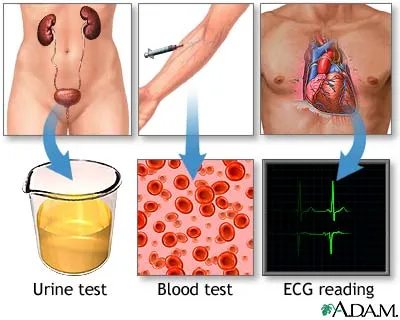
Investigations
-
ECG
-
Fasting blood- HDL cholesterol, LDL cholesterol, triglycerides
- lipid profile
-
Urine for protein and blood
- Serum urea, creatinine & electrolytic
White-Coat Hypertension (Isolated Office HTN, Isolated Clinic HTN)
-
White coat HTN is defined as an elevated BP in the office at repeated visits, while it is normal out of the office, using either ABPM or HBPM.
-
Prevalence of white-coat hypertension averages 13%.
Masked (Isolated Ambulatory) Hypertension
-
Masked HTN is defined as normal BP in the office at repeated visits and elevated out of the office, either on ABPM or HBPM.
-
Possible causes: anxiety, stress.
-
Prevalence of masked hypertension averages about 13%.
-
CV events are 2 times higher than those in true normotension.
Optional Laboratory Tests
Aortic Coarctation
- Arm to leg systolic Blood Pressure difference (abnormal if >20 mmHg)
- Chest X-Ray (notching of the lower rib borders)
- Echocardiogram (Children)
- MRI Chest (Adults)
Cushing’s Disease
- 24-hour Urine Cortisol
- Late night Salivary cortisol
- Low dose Dexamethasone Suppression Test
Pheochromocytoma
- 24h Urine Metanephrine
- Plasma free metanephrines
Note:
- Patients with pheochromocytoma may have a history of paroxysmal headaches, sweating, tachycardia, palpitations, and orthostatic hypotension.
Specialist Investigations
-
Refer people to specialist care the same day if they have ●
-
Accelerated hypertension (BP > 180/110 mmHg) with signs –
- (of papill oedema and/or retinal haemorrhage)
-
Suspected phaeochromocytoma (labile or postural –
- hypotension, headache, palpitations, pallor and diaphoresis)
-
If needed, more investigations for secondary cause of ●
- hypertension could be performed