C. Preventive Measures

Antibiotics for Asymptomatic Bacteriuria (ASB)
- C.1: A seven-day antibiotic regimen is recommended for all pregnant women with asymptomatic bacteriuria (ASB) to prevent persistent bacteriuria, preterm birth, and low birth weight.
- Type of recommendation: Recommended ★ Z
Antibiotic Prophylaxis to Prevent Recurrent Urinary Tract Infections
- C.2: Antibiotic prophylaxis is only recommended to prevent recurrent urinary tract infections in pregnant women in the context of rigorous research.
- Type of recommendation: Context-specific recommendation (research)
Antenatal Anti-D Immunoglobulin Administration
- C.3: Antenatal prophylaxis with anti-D immunoglobulin in non-sensitized Rh-negative pregnant women at 28 and 34 weeks of gestation to prevent RhD alloimmunization is only recommended in the context of rigorous research.
- Type of recommendation: Context-specific recommendation (research)
Preventive Anthelmintic Treatment
- C.4: In endemic areas, preventive anthelmintic treatment is recommended for pregnant women after the first trimester as part of worm infection reduction programmes.
- Type of recommendation: Context-specific recommendation (research)
Tetanus Toxoid Vaccination
- C.5: Tetanus toxoid vaccination is recommended for all pregnant women, depending on previous tetanus vaccination exposure, to prevent neonatal mortality from tetanus.
- Type of recommendation: Recommended ★ Z
FDA Approved Drugs
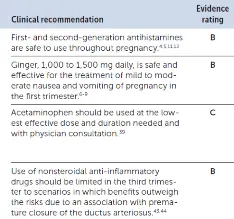
Clinical Recommendation
-
First- and second-generation antihistamines are safe to use throughout pregnancy. 4,5,11,12
-
Ginger, 1,000 to 1,500 mg daily, is safe and effective for the treatment of mild to moderate nausea and vomiting of pregnancy in the first trimester. 6-9
-
Acetaminophen should be used at the lowest effective dose and duration needed and with physician consultation. 39
-
Use of nonsteroidal anti-inflammatory drugs should be limited in the third trimester to scenarios in which benefits outweigh the risks due to an association with premature closure of the ductus arteriosus. 43,44
Table 5. Safety of Over-the-Counter Antacids, Antidiarrheals, and Laxatives in Pregnancy
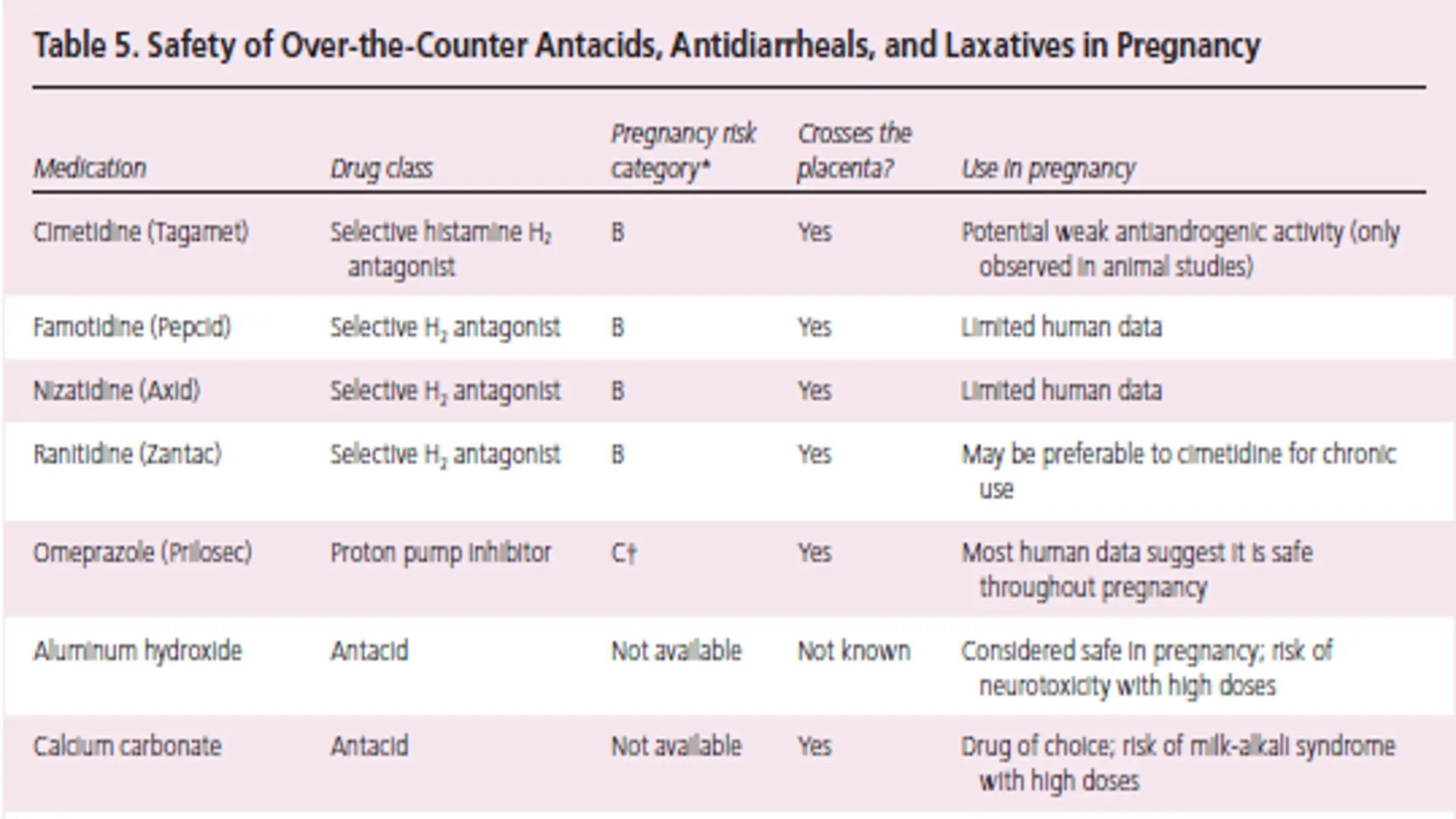
| Medication | Drug Class | Pregnancy Risk Category | Crosses the Placenta? | Use in Pregnancy |
|---|---|---|---|---|
| Cimetidine (Tagamet) | Selective histamine H₂ antagonist | B | Yes | Potential weak antiandrogenic activity (only observed in animal studies) |
| Famotidine (Pepcid) | Selective H₂ antagonist | B | Yes | Limited human data |
| Nizatidine (Axid) | Selective H₂ antagonist | B | Yes | Limited human data |
| Ranitidine (Zantac) | Selective H₂ antagonist | B | Yes | May be preferable to cimetidine for chronic use |
| Omeprazole (Prilosec) | Proton pump inhibitor | C† | Yes | Most human data suggest it is safe throughout pregnancy |
| Aluminum hydroxide | Antacid | Not available | Not known | Considered safe in pregnancy; risk of neurotoxicity with high doses |
| Calcium carbonate | Antacid | Not available | Yes | Drug of choice; risk of milk-alkali syndrome with high doses |
Antibiotics
-
Antibiotics without known teratogenic effects include:
- cephalosporins
- penicillins
- erythromycin
- azithromycin
- clindamycin
- augmentin
- metronidazole.
-
Fluoroquinolones: contraindicated causing premature cartilage closure.
-
Trimethoprim: avoided in the first trimester; folic acid antagonist.
Tetanus Immunization Schedule Z
- TT1: After the 1st trimester
- TT2: At least 4 weeks after TT1 or during subsequent pregnancy
- TT3: At least 6 months after TT2 or during subsequent pregnancy
- TT4: At least one year after TT3 or during subsequent pregnancy
- TT5: At least one year after TT4 or during subsequent pregnancy
Screening for Genetic Abnormalities
Aneuploidy
Defined as an abnormal number of chromosomes.
-
All women, regardless of age, who present for antenatal care should be offered aneuploidy screening & for invasive antenatal testing (chorionic villus sampling [CVS] or amniocentesis) for diagnosis of fetal aneuploidy and other genetic anomalies.
-
First-trimester screening can generally be performed from 10 to 14 weeks’ gestation & second-trimester screening can generally be performed from 15 to 23 weeks’ gestation.
-
Fetal anatomical markers associated with aneuploidy include an echogenic intracardiac focus, absent nasal bone, short humerus or femur, and echogenic bowel.
Screening for Neural Tube Defects (NTDs)
There are 2 approaches for NTD screening:
-
Maternal serum alpha-fetoprotein (MS-AFP) in the second-trimester (optimal at 15 to 18 weeks)
-
Ultrasound (optimal at 18 to 22 weeks).
- Amniocentesis can be performed to determine if amniotic fluid AFP is elevated and acetylcholinesterase is present, which are considered diagnostic of a NTD.
Screening for Hypertensive Disorders of Pregnancy
Most pregnant women with hypertensive disorders of pregnancy (gestational hypertension, pre-eclampsia or haemolysis, elevated liver enzymes, and low platelets [HELLP] syndrome) are asymptomatic.
- All pregnant women should be screened by having their blood pressure (BP) measured and testing for the presence of protein in their urine at every routine antenatal appointment.
- If the BP reading is >140/90 mmHg, a follow-up measurement must be obtained. All women with suspected pre-eclampsia, including those with non-specific symptoms such as nausea, vomiting or malaise, should be evaluated for possible HELLP syndrome.
Screening for Gestational Diabetes Mellitus (GDM)
The following risk factors are recommended:
- BMI (kg/m²) >30
- Previous macroscopic baby weighing ≥ 4.5 kg
- Previous pregnancy involving gestational diabetes
- Family history of diabetes in a first-degree relative
- Ethnicity with a high prevalence of diabetes.
Gestational Diabetes Testing Recommendations
- All women with at least one risk factor be tested for gestational diabetes using:
- 2-hour, 75 g oral glucose tolerance test (OGTT).
- If the early screening test is negative, further screening with an OGTT between 24 and 28 weeks is recommended.
- For women with all other risk factors, a single OGTT at 24 to 28 weeks is recommended.
- Additionally, glycosuria of 2+ any time in pregnancy or 1+ on two or more visits should prompt further testing to exclude gestational diabetes.
Anti-D Immunoglobulin Administration Z
- Rhesus (Rh)-negative women should receive anti-D immunoglobulin within 72 hours of exposure to Rh D positive fetal blood or fetal blood of unknown Rh status if they have any of the following potentially sensitising events in the first-or-second-trimester.
Sensitising Events
- An ectopic pregnancy
- Evacuation of molar pregnancy
- Threatened miscarriage or miscarriage
- Termination of pregnancy (medical or surgical)
- Any invasive procedures (amniocentesis, chorionic villus sampling)
- if the baby is Rh-positive.
Antenatal Considerations
-
Antenatal fetal-maternal haemorrhage (abdominal trauma, placental abruption)
-
Intrauterine fetal death
-
External cephalic version
-
If they deliver a neonate who is Rh-positive.
-
Rh-negative women should routinely be given a single antenatal dose of anti-D immunoglobulin at 28 weeks’ gestation, followed by a second dose after delivery.
Diagnosis and Treatment of Anaemia in Pregnancy
-
Anaemia in pregnancy has been defined as Hb levels <110 g/L and haematocrit (Hct) levels <33% in first & third trimester and Hb levels < 105 g/l (< 10.5 g/dl) – Hct < 32% in 2nd trimester.
-
Anaemia in pregnancy can be dilutational (physiological), due to iron, folate or other vitamin deficiency, a result of thalassemia, or result from other causes.
-
Iron deficiency is the most common cause of anaemia in pregnancy, thus the risk of iron deficiency should be considered in all pregnant women.
Obesity
-
Obese women are at risk for pregnancy complications, including gestational hypertension, gestational diabetes mellitus, cardiac disease, pulmonary disease, obstructive sleep apnoea, and caesarean delivery.
-
Regular aerobic exercise during pregnancy may reduce some of these risks.
-
Antenatal dietary modifications in obese pregnant women can reduce maternal weight gain during pregnancy without adversely influencing neonatal birth weight.
-
Obese patients may also be at increased risk for venous thromboembolism, particularly if other risk factors are present.
Management of Post-Term Pregnancy
Post-term pregnancy is defined as a gestation that has extended to or beyond 42+0 weeks’ gestation.
- The risks of a prolonged pregnancy should be discussed with the pregnant woman so they can make a decision between induction or waiting for spontaneous onset of labour.
- There is a significantly reduced likelihood of perinatal mortality at 41 weeks’ gestation, compared with 42 weeks’ gestation, with risks increasing as the length of the post-term.
- Women may be offered induction of labour by 41 weeks’ gestation (late-term) to avoid risks of post-term pregnancy.