FM
Symptom Scoring System
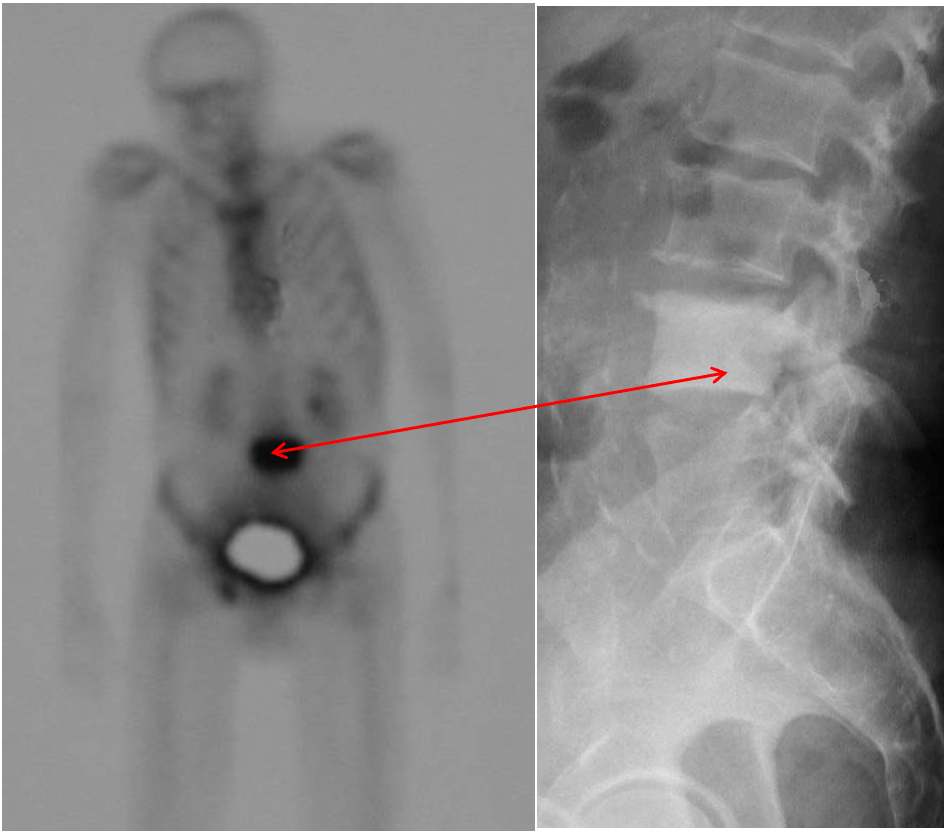
American Urological Association Symptom Index
Over the past month or so:
- How often have you had the sensation of not completely emptying your bladder after you finished urinating?
- How often have you had to urinate again less than two hours after you finished urinating?
- How often have you found that you stopped and started again when urinating?
- How often have you found it difficult to postpone urination?
- How often have you had a weak urinary stream?
- How often have you had to push or strain to begin urination?
How many times do you typically get up to urinate from the time you go to bed at night until the time you get up in the morning?
| Not at all | Less than one in five times | Less than one half of the time | About one half of the time | More than one half of the time | Almost always | |
|---|---|---|---|---|---|---|
| Question 1 | 0 | 1 | 2 | 3 | 4 | 5 |
| Question 2 | 0 | 1 | 2 | 3 | 4 | 5 |
| Question 3 | 0 | 1 | 2 | 3 | 4 | 5 |
| Question 4 | 0 | 1 | 2 | 3 | 4 | 5 |
| Question 5 | 0 | 1 | 2 | 3 | 4 | 5 |
| Question 6 | 0 | 1 | 2 | 3 | 4 | 5 |
Total score: __________
AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX
To assess the severity of benign prostatic hyperplasia (BPH):
- A score of 7 or less indicates mild BPH;
- A score of 8 to 19 indicates moderate BPH;
- A score of 20 to 35 indicates severe BPH.
Digital Rectal Examination
- Assess anal sphincter tone, bladder palpation, and external meatus.
- Prostate usually is enlarged, nontender, and rubbery in consistency.
- In many cases, it has lost the median furrow.
- Prostate size as detected with digital rectal examination may be misleading; an apparently small prostate may cause obstruction.
- If the bladder is distended, the urinary bladder may be palpable or percussible during abdominal examination.
- Firm or hard areas in the prostate may indicate prostate cancer.
BPH
- Typical History
- Digital rectal examination
- Urinalysis and urine culture to exclude UTI
- Prostate-specific antigen level
- Bladder ultrasonography
- Uroflowmetry
Prostate-Specific Antigen (PSA) Levels
- Interpreting prostate-specific antigen (PSA) levels can be complex.
- It is moderately elevated in 30 to 50% of patients with BPH, depending on prostate size and degree of obstruction.
- It is elevated in 25 to 92% of patients with prostate cancer, depending on the tumor volume.
PSA Levels Interpretation
- In patients without cancer, serum PSA levels:
- >1.5 ng/mL (1.5 mcg/L) usually indicate a prostate volume ≥ 30 mL.
- > 4 ng/mL (4 mcg/L), further discussion/shared decision-making regarding other tests or biopsy is recommended.
- For men aged < 50 or those at high risk of prostate cancer:
- Lower cutoff (PSA > 2.5 ng/mL [2.5 mcg/L]) may be used.
Other Testing
- Per-abdomen Ultrasonography
- Transrectal ultrasonography is an accurate way to measure prostate volume.
- Transrectal biopsy is usually done with ultrasound guidance and is usually only indicated if there is suspicion of prostate cancer.
- Clinical judgment must be used to evaluate the need for further testing.
Alternative Testing
- Alternatively, multiparametric MRI, which is more sensitive than transrectal biopsy.
- Restricting biopsies to areas found to be suspect on multiparametric MRI may reduce the number of prostate biopsies and diagnoses of clinically insignificant prostate cancers.
- Cystoscopy may help determine the optimal surgical approach and rule out other obstructive causes such as strictures.
IMIG
Benign glandular and stromal hyperplasia of the transitional zone of the prostate Typically there is an increase in volume of the prostate with a calculated volume exceeding 30cc .
Post-micturition residual volume is typically elevated: More than 50 mL is usually considered abnormal.
Clinical presentation:
- To remember the symptoms of BPH, think “FUNWISE”: Frequency, Urgency, Nocturia, Weak stream /hesitancy, Intermittent stream, Straining to urinate, and Emptying (not emptying completely, terminal dribbling).
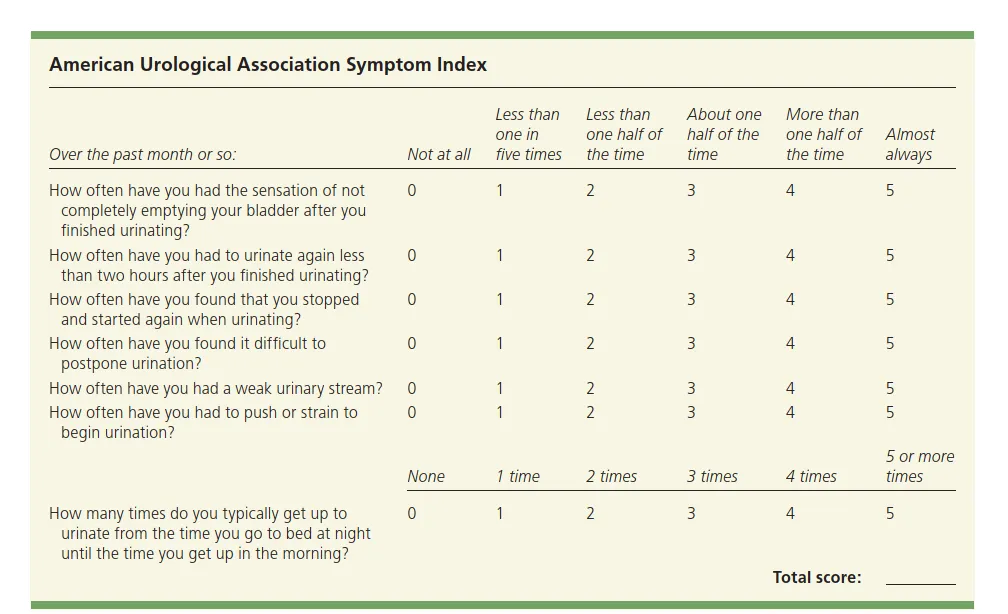
Ultrasound : Transabdominal ultrasound (TAUS)
Indications: Ultrasound pelvis: Consider prior to initiating treatment to assess the size of the prostate.
Supportive findings of BPH:
- Increased total prostate volume
- Elevated PVR volume
- Evidence of bladder outlet obstruction (e.g., bladder wall thickening and hydronephrosis ).
Transrectal ultrasound (TRUS):
TRUS is not required for the initial evaluation of BPH.
Indications
- Suspected prostate cancer to guide biopsy
Case . 75 years old male with retention of urine
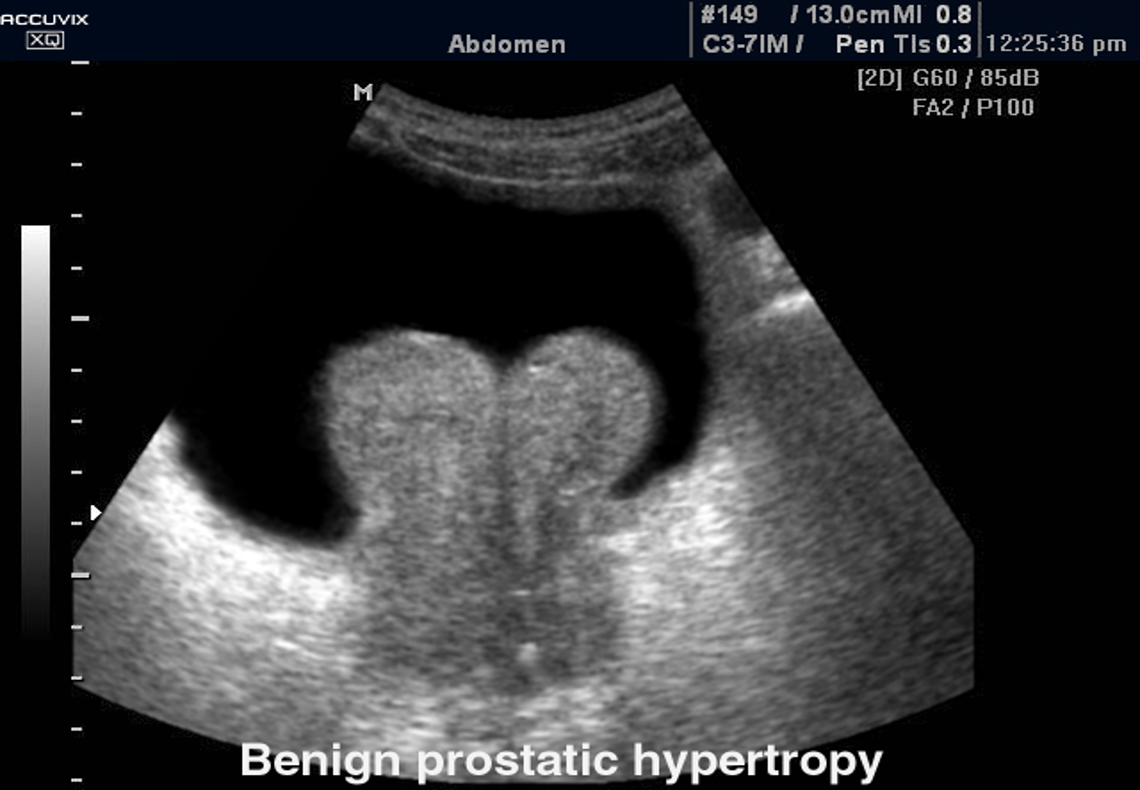
Transrectal ultrasound images of prostate
MRI and CT pelvis
-
Commonly used for preprocedural assessment of prostate volume and localization of enlarged tissue
-
MRI can potentially differentiate BPH from prostate cancer.
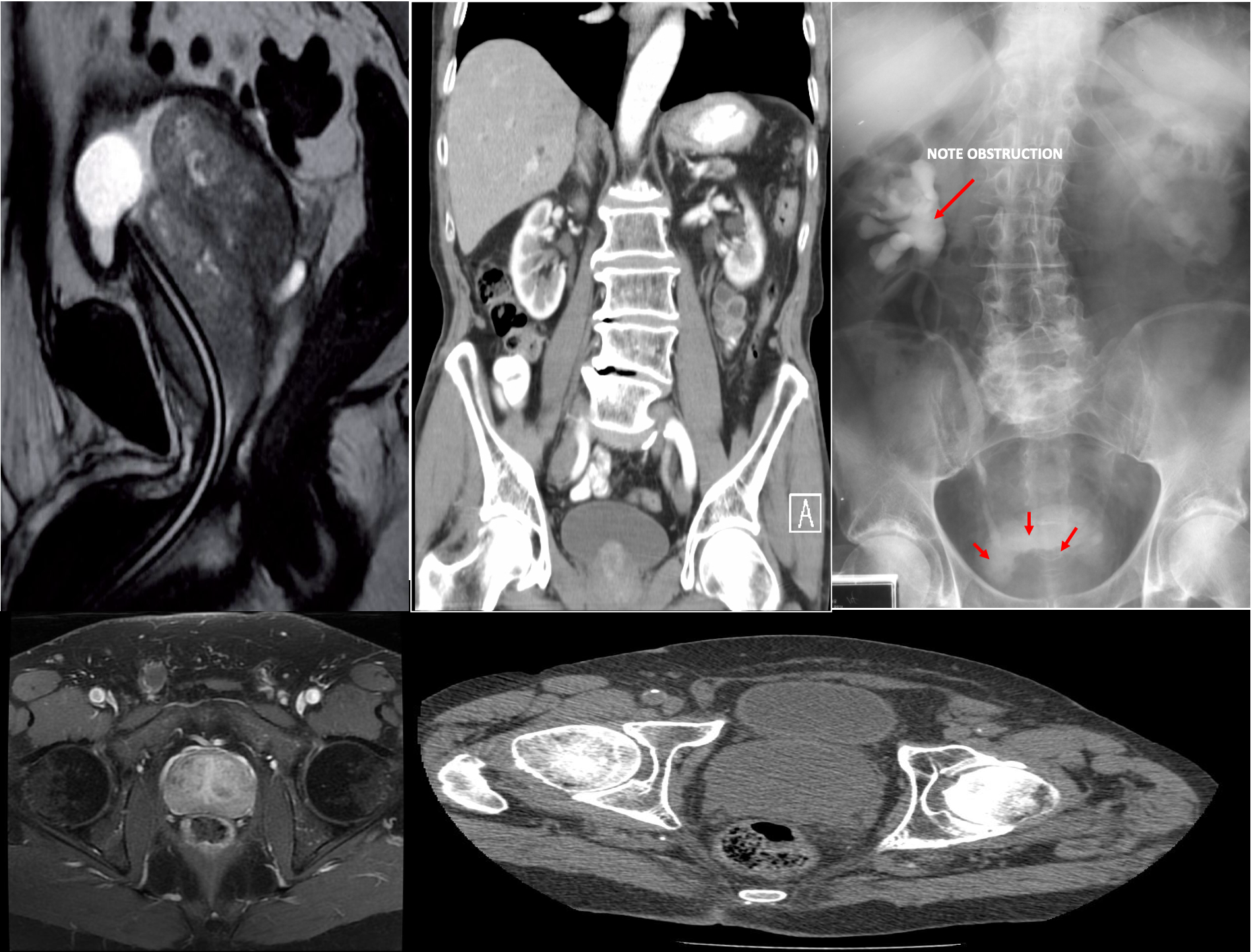
Enlarged prostate gland - MRI pelvis (T2-weighted, sagittal plane) The enlarged prostate gland is lobulated and heterogeneous. The bladder base is elevated. A foley catheter is in place.
This can obstruct the ureters entering the bladder leading to hydronephrosis and renal failure.
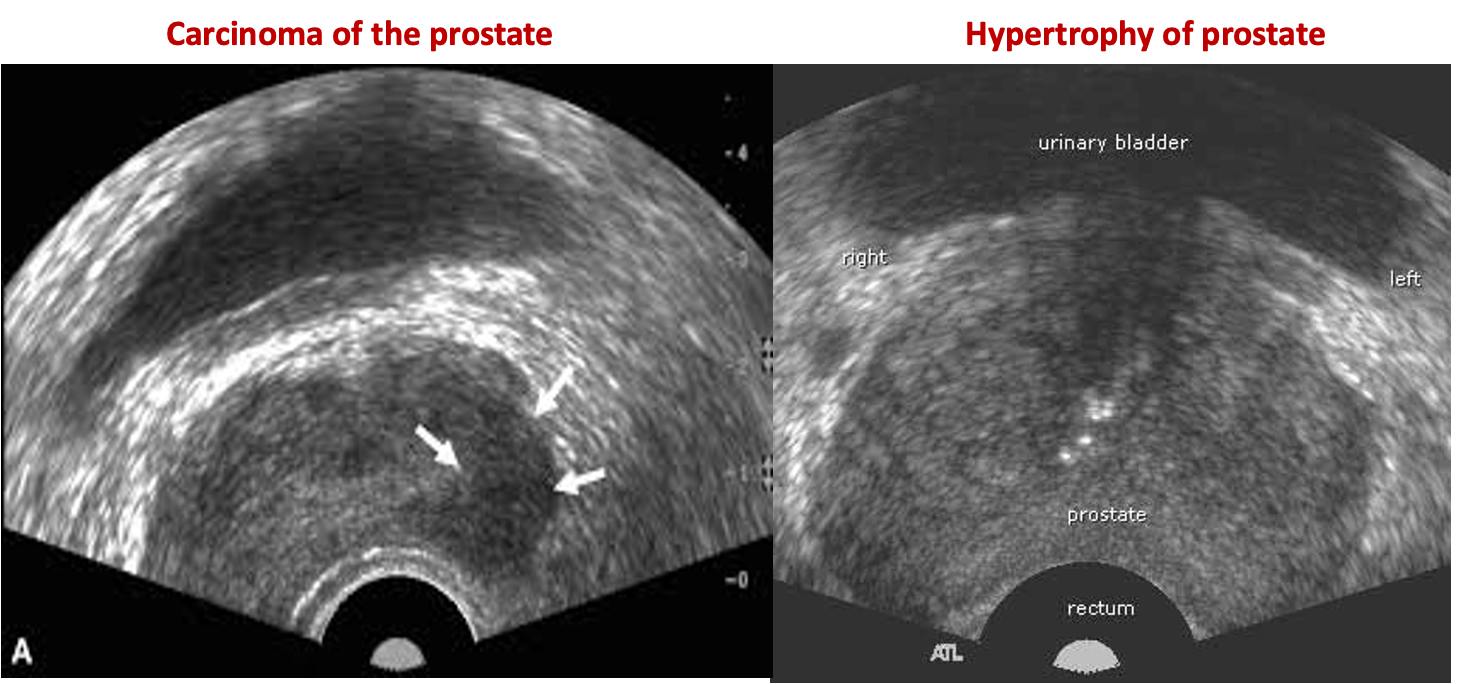
The nuclear bone scan
shows increased activity at site. Prostate malignancy often metastasizes to the skeleton and is usually sclerotic (dense) .