FM
DSM-5 Criteria for Major Depressive Disorder
Five or more of the following symptoms during the same 2-week period, with the symptoms representing a change from previous functioning and with at least one of the symptoms being either depressed mood or loss of interest or pleasure in activities of daily life (symptoms that are clearly attributable to another medical condition are not included).
- Depressed mood most of the day, nearly every day, as indicated by either subjective report (e.g., feels sad, empty, or hopeless) or observation made by others (e.g., appears tearful). (In children and adolescents, a depressed mood can be an irritable mood.)
- Markedly diminished interest or pleasure in all, or almost all, activities most of the day, nearly every day (as indicated by either subjective account or observation).
- Significant weight loss when not dieting or weight gain (e.g., a change of >5% of body weight in a month), or decrease or increase in appetite nearly every day. (In children, failure to gain expected weight should be considered.)
- Insomnia or hypersomnia nearly every day.
- Psychomotor agitation or retardation nearly every day (observable by others, not merely subjective feelings of restlessness or being slowed down).
- Fatigue or loss of energy nearly every day.
- Feelings of worthlessness or excessive or inappropriate guilt (which may be delusional) nearly every day (not merely self-reproach or guilt about being sick).
- Diminished ability to think or concentrate, or indecisiveness, nearly every day (either by subjective account or as observed by others).
- Recurrent thoughts of death (not just fear of dying), recurrent suicidal ideation without a specific plan, or a suicide attempt or a specific plan for committing suicide.
Diseases that may mimic depression
- Manifestations of dementia and delirium, including loss of social interactions, negative mood states, and cognitive dysfunction, may be similar to those of major depressive disorder.
- Multiple other medical conditions have been associated with depressive symptoms; these conditions include:
- Anemia
- Hypothyroidism
- Seizures
- Parkinson’s disease
- Sleep apnea
- Deficiencies of vitamins such as B12 and folate
- Infectious diseases such as human immunodeficiency virus (HIV) infection, syphilis, and Lyme disease
Screening for depression and suicide
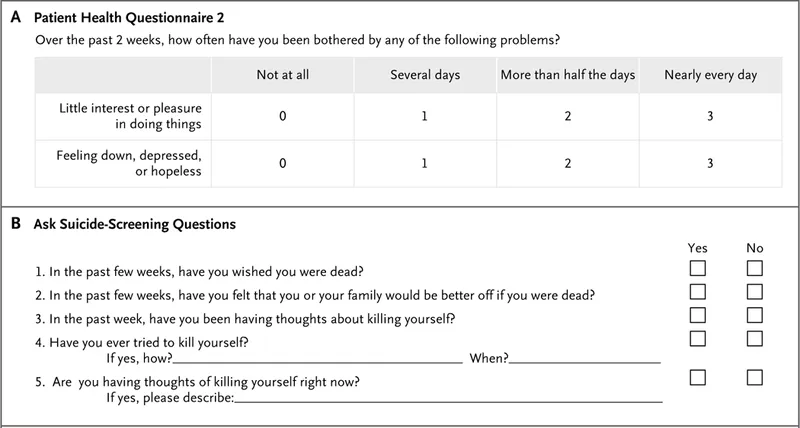
A. Patient Health Questionnaire 2
Over the past 2 weeks, how often have you been bothered by any of the following problems?
| Not at all | Several days | More than half the days | Nearly every day | |
|---|---|---|---|---|
| Little interest or pleasure in doing things | 0 | 1 | 2 | 3 |
| Feeling down, depressed, or hopeless | 0 | 1 | 2 | 3 |
B. Ask Suicide-Screening Questions
- In the past few weeks, have you wished you were dead?
- In the past few weeks, have you felt that you or your family would be better off if you were dead?
- In the past week, have you been having thoughts about killing yourself?
- Have you ever tried to kill yourself?
If yes, how? ____________________________ When? _______________ - Are you having thoughts of killing yourself right now?
If yes, please describe: ____________________________
Key Clinical Points (Depression)
- Screening for depression and suicidal thinking and behavior is important in the primary care setting.
- Distinguishing between bipolar disorder and major depressive disorder is critical for treatment selection.
- The first-line treatment for mild depression is psychotherapy and symptom monitoring.
- Antidepressant drugs have been shown to have a favorable benefit-risk profile in moderate-to-severe depression. Psychotherapy may also be a first-line choice for moderate depression.
- The choice of treatment depends on associated side effects, the presence of coexisting conditions, specific symptoms, and the patient’s history of response.
Psychiatry
Etiology and Pathogenesis of Depressive Disorders
- Biochemical: A deficit of specific neurotransmitters in the brain mainly Serotonin, Noradrenaline, and Dopamine
- Psychosocial: Factors like low self-esteem and dependent personalities
- Social: Life events and stress
- Developmental factors: Genetic and hereditary factors
- Integrative: Involves all previous factors
Areas in Brain Affected by Depression
- Limbic System
- Hypothalamus
DSM Qualifiers of Mood States (Coded with Main Diagnosis)
- Atypical features: Overeating, oversleeping while depressed; preserved reactivity to reward.
- Catatonic Features: Detachment from the environment while awake; negativism including immobility, mutism, refusal to eat or drink. May be life-threatening.
- Melancholic Features: Dense anhedonia, lack of response to reward, terminal insomnia (early morning awakening), diurnal variation (mornings worse).
- Postpartum onset: Depressive episode within 1 month of childbirth by definition. Clinically, this period of markedly increased risk may be ≥ 3 months. Often includes marked anxiety.
- Psychotic features: Mood congruent in depression: Delusions of poverty, guilt, nihilism, illness, self-disgust; derogatory auditory hallucinations.
- Mood congruent in mania: Delusions of special powers or unlimited resources, paranoia, auditory hallucinations.
A 21st Century View of Depression
- Environmental factors: (including external environment: psychosocial stressors, sleep deprivation, internal environment: gonadal/HPA steroids)
- Behavior: Cognitive/Affective/Sensorymotor
- Systems: Critical circuitry
- Cellular:
- Cell growth/survival/death
- Cell morphology: dendritic remodeling
- Molecular:
- Susceptibility genes
- Protective genes
- Transcription factors
- mRNA
BDNF, CREB, PKC, and other regulatory proteins
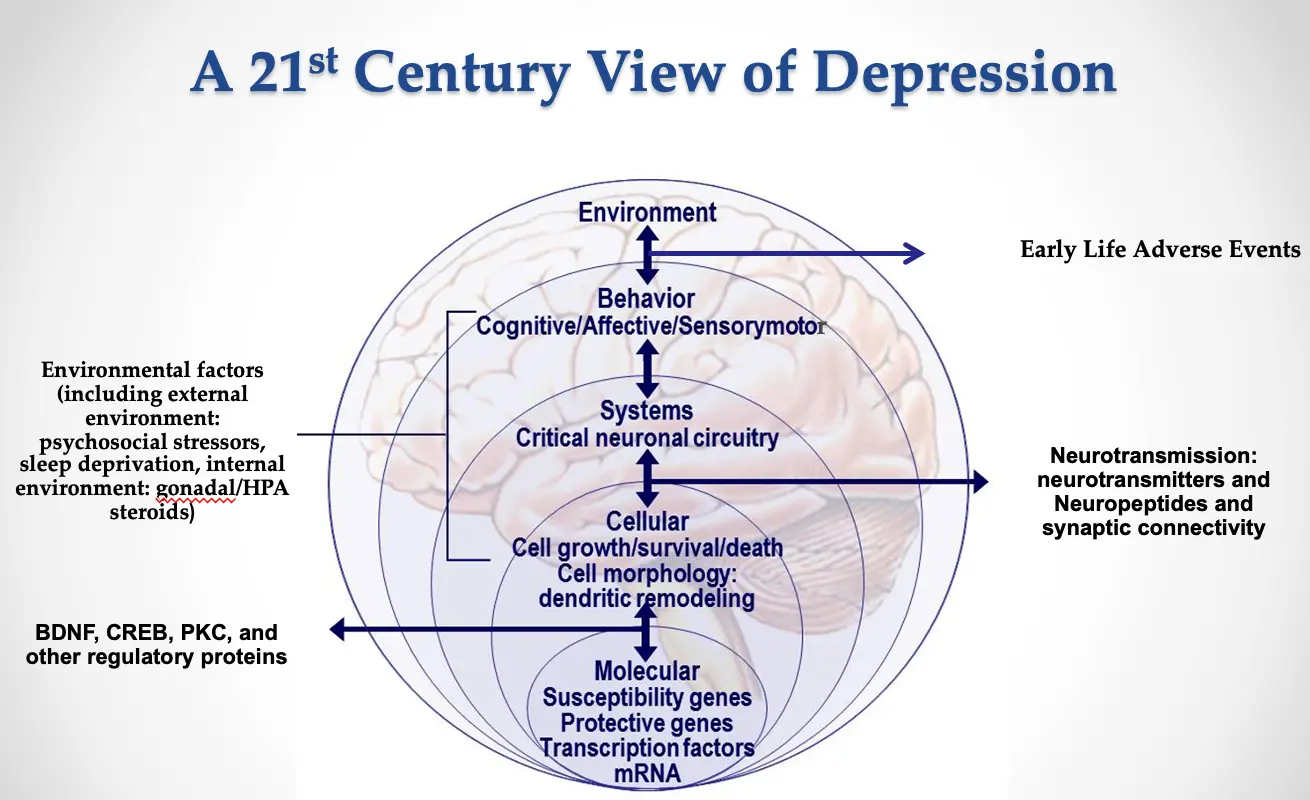 Key message:
From the neurobiological perspective, a new clinical outlook of depression encompasses the understanding of molecular, cellular, chemical, behavioral and environmental factors of depression.
Key message:
From the neurobiological perspective, a new clinical outlook of depression encompasses the understanding of molecular, cellular, chemical, behavioral and environmental factors of depression.
BDNF = brain-derived neurotrophic factor; CREB = cAMP responsive element binding;
HPA = hypothalamic-pituitary-adrenal; mRNA = messenger ribonucleic acid; PKC = protein kinase C;
Schloesser RJ et al. 2008. Neuropsychopharmacol Rev. 2008;33:110-33.
Depression: A Disease of the Mind, Brain, and Body
- Prefrontal cortex
- Hypothalamus
- Amygdala
- Locus ceruleus
- Cytokines
- Cortisol
- Increased sympathetic outflow
- ACTH
- Adipose tissue
- Bone
- Adrenal gland
Gold PW, Charney DS. Am J Psychiatry. 2002;159(11):1826.

It is known that depression is an illness that affects the mind and mood of a sufferer, altering that person’s core experience of others and the world around them. There is emerging evidence that depressed patients have a significant loss of cells in the prefrontal cortex. An increase in cortisol and norepinephrine secretion represents a highly adverse biochemical environment, a condition that is likely to contribute to many different adverse outcomes, including increased
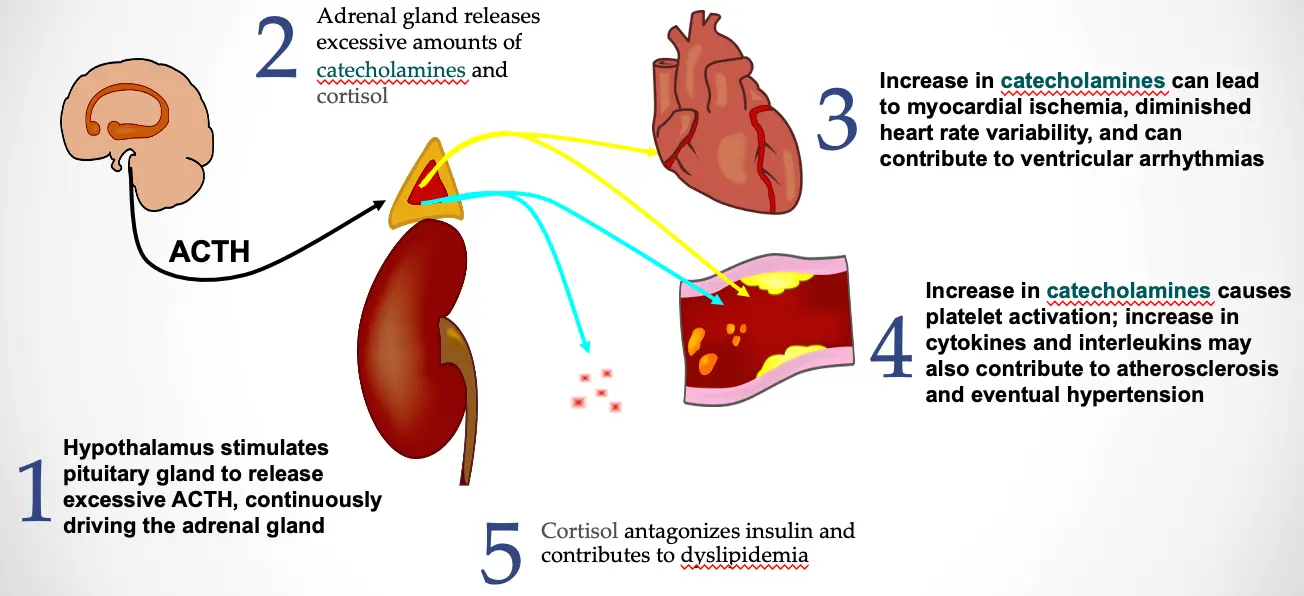
Major Depressive Disorder May Have Systemic Consequences
- Hypothalamus stimulates pituitary gland to release excessive ACTH, continuously driving the adrenal gland
- Adrenal gland releases excessive amounts of catecholamines and cortisol
- Increase in catecholamines can lead to myocardial ischemia, diminished heart rate variability, and can contribute to ventricular arrhythmias
- Increase in catecholamines causes platelet activation; increase in cytokines and interleukins may also contribute to atherosclerosis and eventual hypertension
- Cortisol antagonizes insulin and contributes to dyslipidemia
ACTH=Adrenocorticotropic hormone
Adapted from Musselman DL et al. Arch Gen Psychiatry 1998;55(7):580-92.
Depression and Chronic Disease
- Chronic illness has been associated with increased prevalence of depression
- Diseases include:
- Diabetes
- Hypertension
- Cardiovascular diseases
- Mild cognitive impairment prior to onset of dementia
- Cancer
- HIV
- COPD
- Rheumatoid arthritis
HIV = human immunodeficiency virus; COPD = chronic obstructive pulmonary disease
Simon GE. West J Med 2001;175:292-3; de Groot et al., Diabetes Spectrum 2010;23:15-8;
Scalco et al. Clinics 2005;60:241-50; Barnes DE et al. Arch Gen Psychiatry 2006;63:273-80; Lin HB et al. Ann Fam Med 2009;7:414-21.
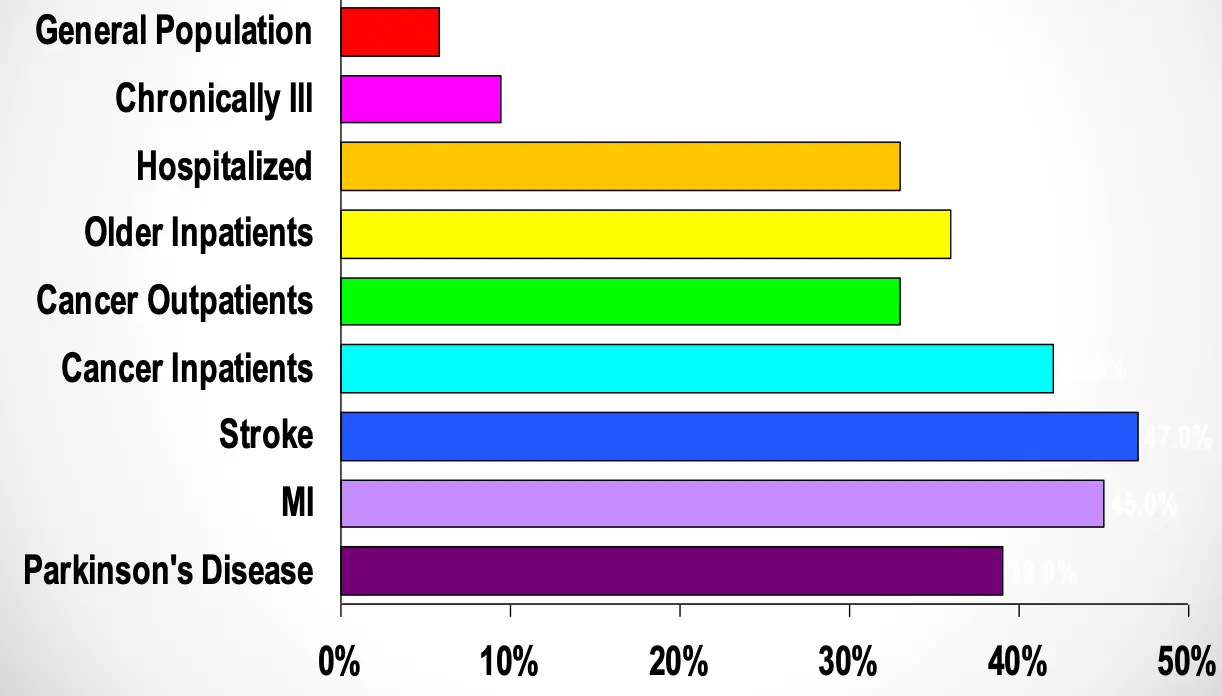
Prevalence Rates of Depression in Chronic Medical Disorder
- General Population
- Chronically III
- Hospitalized
- Older Inpatients
- Cancer Outpatients
- Cancer Inpatients
- Stroke
- MI
- Parkinson’s Disease
… I FEEL SO DEPRESSED!
- YES, YES, YES - but has there been any family history of asthma, diabetes, high blood pressure?
- What about heart disease, liver disease, kidney trouble?
Martin Davis 1997

Signs
-
Depressed For
- No Reason
- Depressed For
- A Good Reason
-
JUST DEPRESSED,
- DON’T WANT TO
- ANALYZE IT
Structural Changes in Brain in Depression
- Depression
- Decrease in neurogenesis
- Decrease in hippocampal volume
- Cellular atrophy
Cellular Atrophy in Depression
- Rat hippocampal neurone before (A) and after (B)
- 3-week repeated stress
Evidence of Hippocampal Atrophy and Loss in Patients With MDD
- **Compared to controls, patients with depression had smaller hippocampal volumes (n=16)**1
- Decreased hippocampal volume may be related to the duration of depression2−4
- Brenner JD, et al. Am J Psychiatry. 2000;157(1):115-118.
- Sheline YI, et al. J Neurosci. 1999;19(12):5034-5043.
- Sheline YI, et al. Proc Natl Acad Sci USA. 1996;93(9):3908-3913.
- Sheline YI, et al. Am J Psychiatry. 2003;160(8):1516-1518.
Images courtesy of JD Bremner.

Barriers to Diagnosis and Treatment in the Arab Countries
- Lack of education about depression
- Lack of availability of appropriate therapies
- Competing clinical demands
- Social issues
- Lack of patient acceptance of the diagnosis
Depression is one of the most common causes of morbidity in developing countries. It is believed that there are many barriers to diagnosis and treatment in the primary care setting. Through a sample of 50 primary health care providers working in the public health clinics of the Jordanian Ministry of Health (MOH), it was identified that the lack of education about depression, lack of availability of appropriate therapies, competing clinical demands, social issues, and the lack of patient acceptance of the diagnosis were among the most important barriers to the identification, diagnosis, and treatment of patients with depression in this population. REFERENCE: Nasir LS, Al-Qutob R. Barriers to the diagnosis and treatment of depression in Jordan. A nationwide qualitative study. Am Board Fam Pract. 2005 Mar-Apr;18(2):125-31.
Freud
“Melancholia, whose definition fluctuates even in descriptive psychiatry, takes on various clinical forms the grouping together of which into a single unity does not seem to be established with certainty; and some of these forms suggest somatic rather than psychogenic affections.”
Mourning and Melancholia (1917)
Are Depressed Patients More Likely to Be Medically Ill?
- 1500 Depressed Patients were evaluated for General Medical Conditions
- Total prevalence was 53%
- Those with older age, lower income, unemployment, limited education and longer duration of depression were at higher risk
| Disease / System | Prevalence % |
|---|---|
| Musculoskeletal | 43% |
| Respiratory | 32% |
| Heart | 29% |
| Upper GI | 26% |
| Neurological | 25% |
| Endocrine | 24% |
Yates et al, Gen Hosp Psych 2004
STAR-D Study
Likelihood of Depression Increases with No. of Physical Symptoms at Presentation
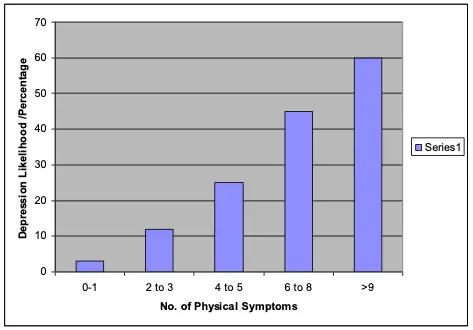
Kroenke K, et al. Arch Fam Med 1994
Out patient data. High utilizers are ususally depressed, anxious or somatization d/o or substance abuser
Medical Screening for Mood Episodes Should Include:
- Review of systems, physical exam, blood count and chemistries, thyroid function tests, and tests for auto-immune factors. Other studies (EKG, neuroimaging) should be obtained only if indicated by specific symptoms, not just abnormal mood.
Differential Diagnosis of Depression
- Grief
- Medical causes
- Other psychiatric disorders
What is Grief?
- Grief is the physical, emotional, somatic, cognitive and spiritual response to actual or threatened loss of a person, thing or place to which we are emotionally attached. We grieve because we are biologically willed to attach. (John Bowlby, Father of Attachment Theory)