IM
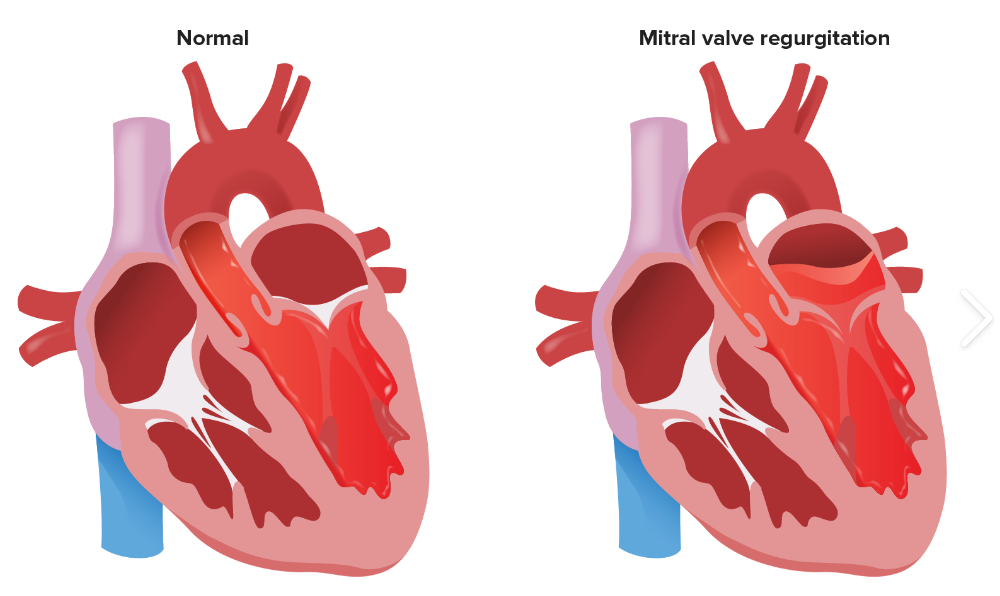
Mitral Regurgitation
Chronic Mitral Regurgitation Overview
Definition: Backflow of blood from the LV to the LA during systole
Mild (physiological)
MR is seen in 80% of normal individuals.
Pathophysiology
Acute MR: ↑ LV end-diastolic volume → rapid ↑ LA and pulmonary pressure → pulmonary venous congestion → pulmonary edema
Chronic (compensated) MR: progressive dilation of the LV (via eccentric hypertrophy) → ↑ volume capacity of the LV (preload and afterload return to normal values) → ↑ end-diastolic volume → maintains ↑ stroke volume (normal EF)
Chronic (decompensated) MR: progressive LV enlargement and myocardial dysfunction → ↓ stroke volume → ↑ end-systolic and end-diastolic volume → ↑ LV and LA pressure → pulmonary congestion, possible acute pulmonary edema, pulmonary hypertension, and right heart strain
Acute MR
-
Endocarditis
-
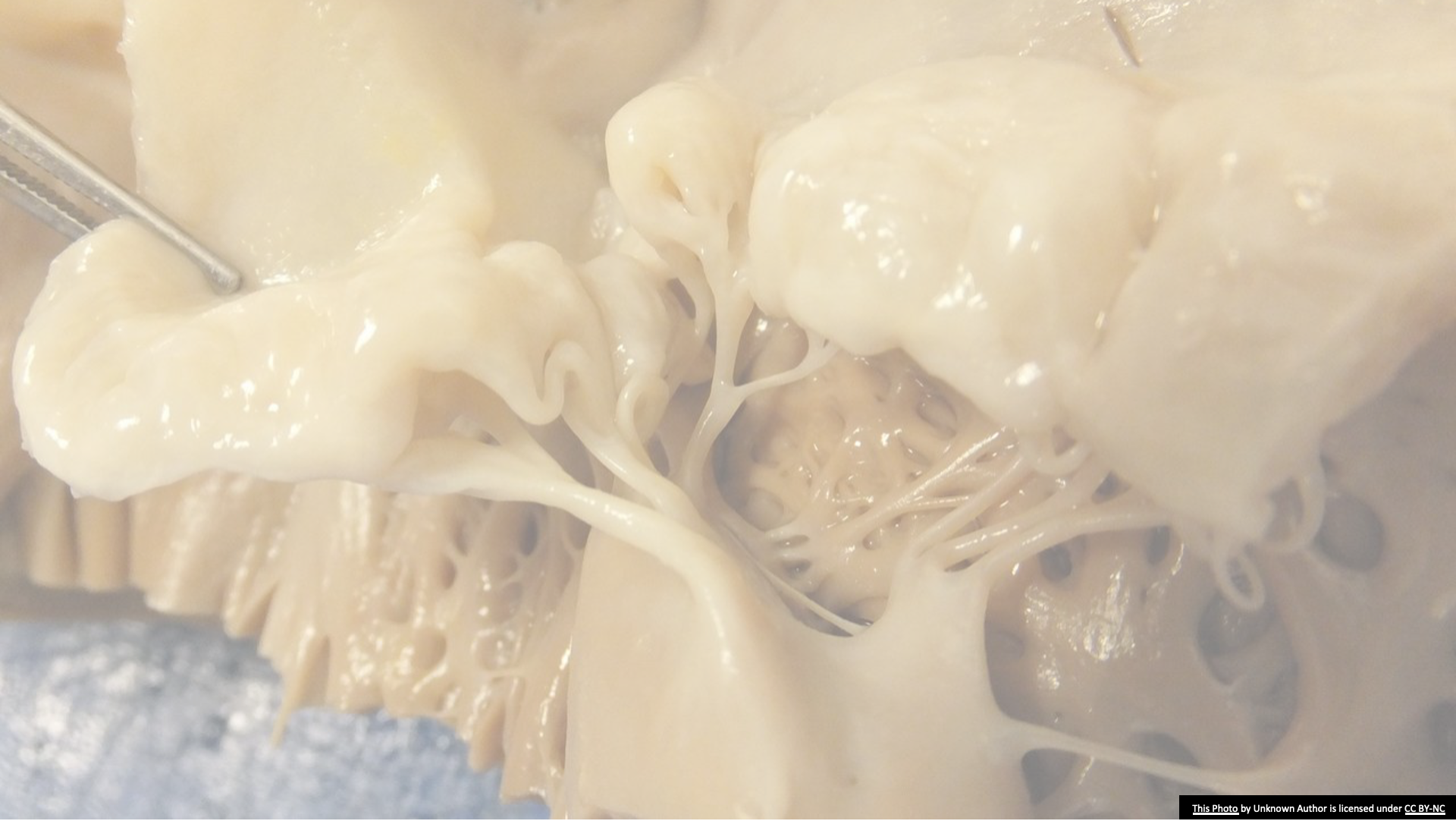
Acute MI: papillary muscle infarction ruptured chordae tendineae
-
Malfunction or disruption of prosthetic valve
-
Acute rheumatic fever
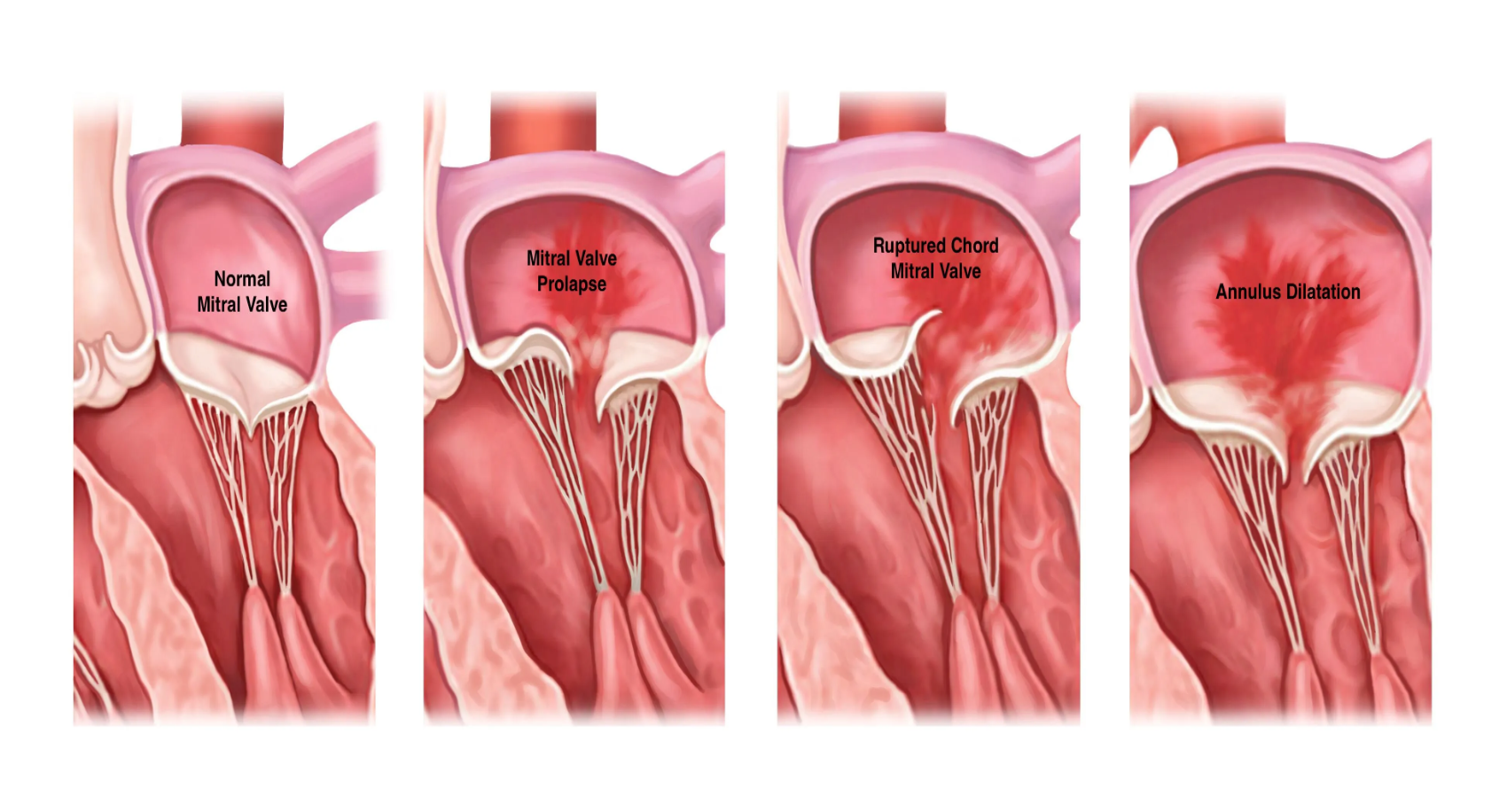
Etiologies of Chronic Mitral Regurgitation
-
Myxomatous degeneration (MVP)
-
Ischemic MR
-
Rheumatic heart disease
-
Infective Endocarditis
-
Connective tissue disease (Ehlers–Danlos syndrome, Marfan’s syndrome)
-
Coronary heart disease: ischemic mitral regurgitation
-
Left ventricular dilatation: cardiomyopathy.
Mitral valve prolapse
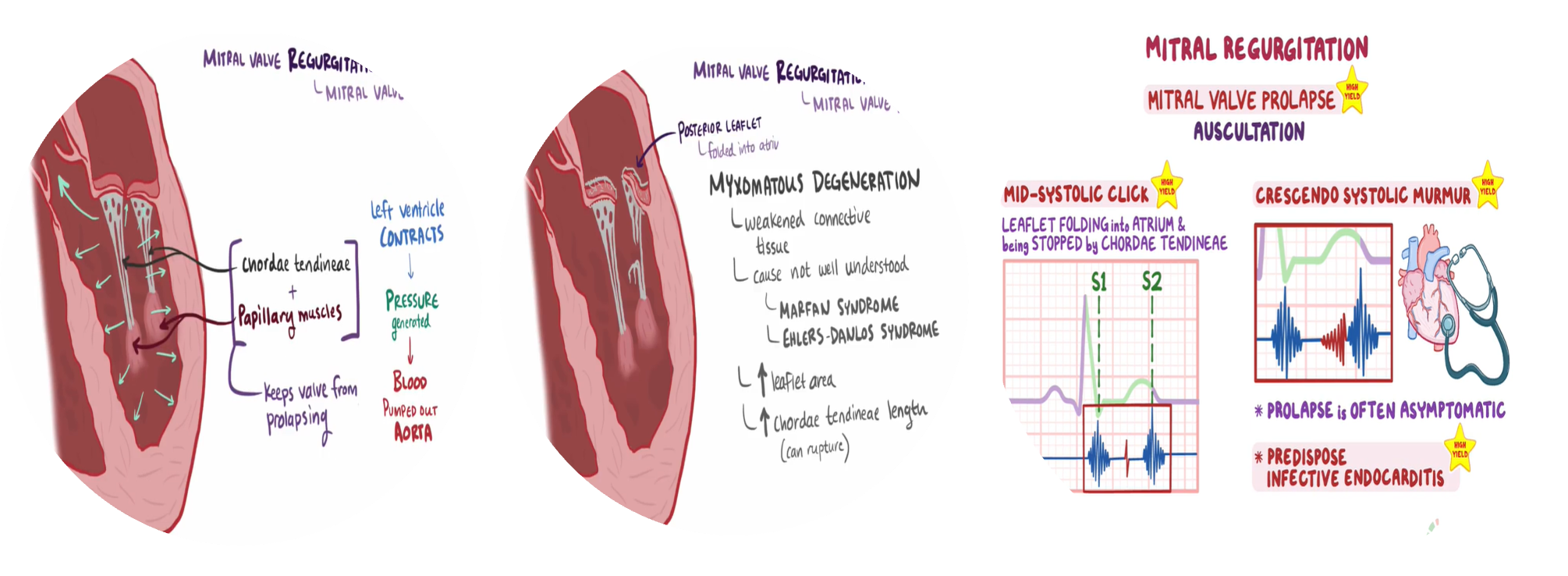
Clinical features
Key features
Acute mitral regurgitation
-
Emergency: Sudden onset severe dyspnea & rapidly progressive pulmonary edema
-
Hypotension and cardiogenic shock
Chronic mitral regurgitation
-
Asymptomatic if mild or moderate
-
Symptoms: when left HF develops (severe MR dyspnea on exertion
-
Fatigue
-
Atrial fibrillation
-
At risk of developing infective endocarditis
Physical Exam findings in MR
-
Exertion Dyspnea: (Exercise intolerance)
-
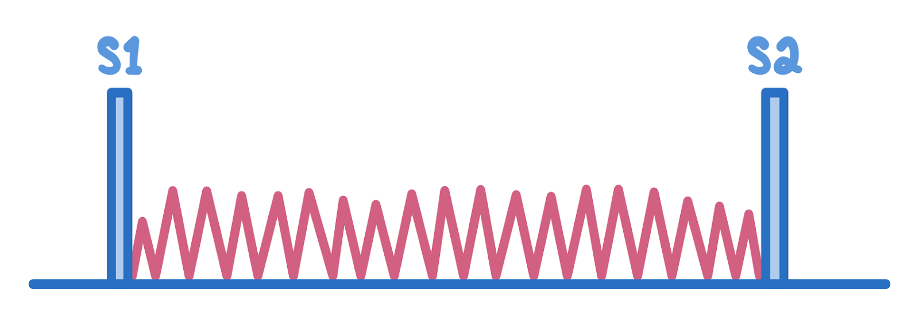
Auscultation: Soft S1 and a holosystolic murmur at the apex radiating to the axilla
-
S3 (CHF/LA overload)
-
In chronic MR, the intensity of the murmur does correlate with the severity.
-
Heart Failure: coincide with increased hemodynamic burden e.g., pregnancy, infection or atrial fibrillation
Investigations
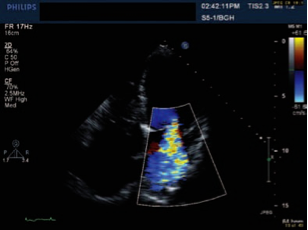
Echocardiography and Doppler
ALL patients: Trans-thoracic echocardiography with Doppler; determine left and right ventricular function and pulmonary artery pressures
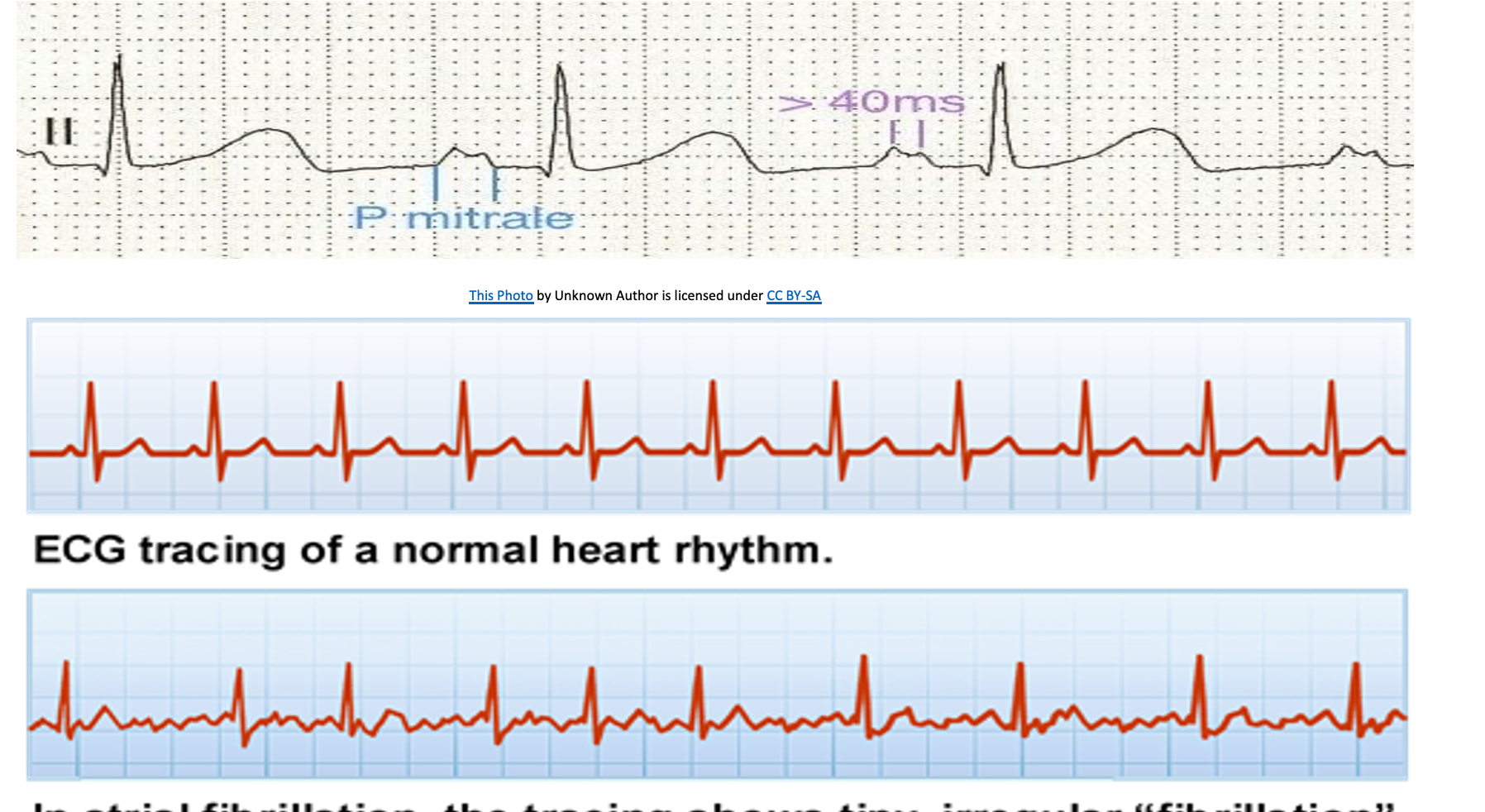
ECG
- AF common
- P-mitrale (bifid P waves) due to left atrial enlargement
- Changes uncommon in acute mitral regurgitation
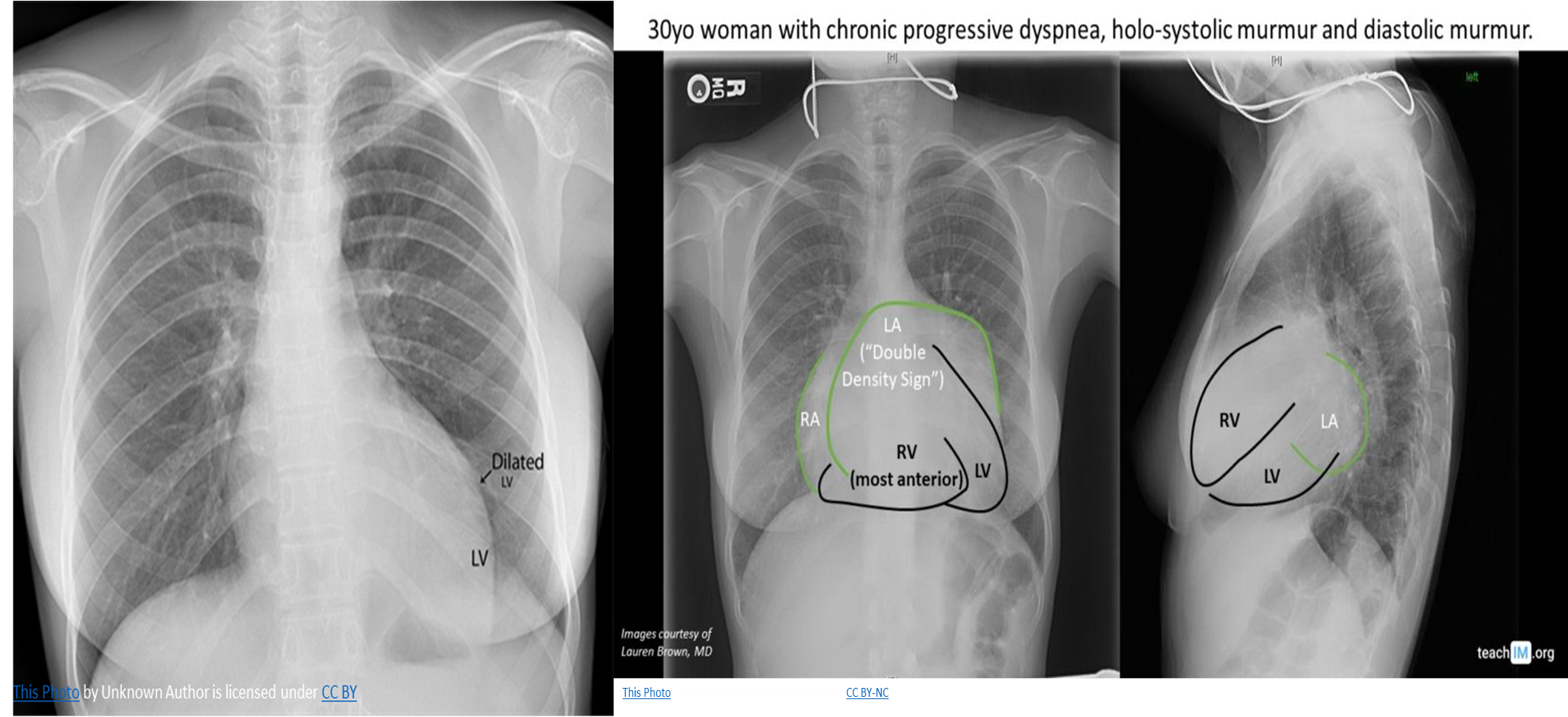
CXR
-
Cardiomegaly: enlarged left atrium and ventricle
-
Signs of congestive heart failure
-
Acute MR: heart size is usually normal but shows pulmonary edema (alveolar edema).
Treatment
Acute mitral regurgitation
-
All patients: primary urgent surgical repair or valve replacement.
-
Manage HF before surgery. (diuretics, nitrates, antihypertensive drugs).
-
If secondary MR: identify and treat the underlying cause (revascularization therapy for ischemic MR)
Surgical therapy:
Indications
- Acute primary MR (urgent surgery)
- Acute secondary MR that does not adequately respond to medical therapy
Procedures
- Valve repair: preferred option because of the reduced risk of mortality and complications
- Valve replacement: severe destruction of the mitral valve
- Revascularization therapy: ischemic MR with papillary muscle rupture`
Medical therapy
-
Temporizing measure before surgery
-
Vasodilators: to reduce afterload and improve cardiac output e.g. Nitroprusside, Nitrates
-
Diuretics: furosemide: acute pulmonary edema
-
Hypotension: inotropes (dobutamine)
-
Atrial fibrillation: cardiac resynchronization therapy to improve hemodynamics.
Chronic mitral regurgitation
Medical therapy: all patients to optimize cardiac function but surgery is the definitive treatment option.
Medical management:
-
Identify & treat underlying cause 2nd MR
-
Heart failure
-
Diuretics: furosemide
-
ACE inhibitors: Lisinopril
-
Beta blockers: Metoprolol
-
-
Ischemic MR: revascularization therapy
-
Atrial fibrillation: evaluation for cardiac resynchronization therapy
Surgical
- LV dysfunction: LVEF 30–60%
- Severe MR and persistent symptomatic heart
Management of chronic MR: symptoms and extent of heart failure and the cause of MR because of the high mortality rate and low likelihood of symptom improvement.
- Left ventricular assisted device
Complications
- Heart failure; pulmonary edema
- Cardiogenic shock
- Atrial fibrillation
- Increases risk of stroke and other thromboembolic complications
- Acute decompensation of heart failure in chronic MR
- Endocarditis
- Pulmonary artery hypertension
Case 1
A 20-year-old man is evaluated for sudden onset palpitations, dyspnea, and dizziness. His temperature is 36.0°C, pulse is 102/min, and blood pressure is 135/86 mmHg. Chest examination demonstrates pectus excavatum. Cardiac auscultation reveals a mid systolic click followed by a late-systolic crescendo murmur over the cardiac apex. ECG demonstrates. Which of the following is the most likely diagnosis?
-
Coarctation of the aorta
-
Aortic stenosis
-
Mitral valve prolapse
-
Mitral stenosis
-
Ventricular septal defect
Case 2
A 70-year-old woman is being evaluated for sudden onset dyspnea. 3 days prior, she underwent PCI, which demonstrated right coronary artery stenosis. The ECG at that time demonstrated ST-segment elevation in leads II, III, and aVF. Current temperature is 37.0°C, pulse is 120/min, respirations are 20/min, and blood pressure is 90/50 mmHg. On physical examination, the following murmur pattern is appreciated over the 5th left midclavicular intercostal space. Which of the following is the most likely explanation for this patient’s new onset dyspnea?
-
Ventricular septal rupture
-
Ventricular aneurysm
-
Papillary muscle rupture
-
Ventricular arrhythmia
-
Left ventricular free wall rupture
Mitral + tricuspid Regurge, VSD,
Tricuspid increased with inspiration, on tricuspid area or left sternal border
VSD in 3rd ICS - can be found in any area of the chest