Why do people continue to smoke?
- Addiction to nicotine
- Perceived benefits (relaxation, weight loss)
- Social context
- Mental health issues

Smoking Cessation Barriers
- Withdrawal symptoms
- Fear of failure
- Weight gain
- Lack of support
- Depression
- Enjoyment of tobacco
- Being around other users
- Limited knowledge of effective treatment options
Physician Barriers to Help
- Time constraints of practice
- Lack of office systems
- Low expectation of success
- Lack of knowledge of what to do
- Frustration with smokers
Smoke vs. Quit
Reasons not to Quit
- Family and friends smoke
- Withdrawal symptoms
- Inability to cope with stress
- Connection with smoking
- Previous unsuccessful attempts to quit
Reasons to Quit
- Encouragement from family and friends
- Health improvements
- To save money
- Pregnancy
- Smoke-free environment policies
- Desire to be a role model
- Medical treatment that requires abstinence
Tobacco Dependence as a chronic disease

Benefits of Quitting
-
20 mins:
blood pressure and pulse rate return to normal -
8 hours:
blood nicotine & CO halved, oxygen back to normal -
24 hours:
CO eliminated; lungs start to clear mucus etc. -
48 hours:
nicotine eliminated; senses of taste & smell much improved. -
72 hours:
breathing easier; bronchial tubes begin to relax; energy levels increase -
2-12 weeks:
- circulation improves
- lung function increased b
-
3-9 months:
- <10% coughs, wheezing decrease
-
5 years:
- risk of lung cancer halved, risk of heart attack halved
-
10 years:
- compared to continued smoking
- risk of heart attack equal to never-smoker’s
Quitting- other benefits
- Improved health and physical performance
- Improved taste of food and sense of smell
- Better appearance, including reduced wrinkling/aging of skin and whiter teeth
- Healthier families, babies and children
- A good example for children and others
- More money in your pocket.
Treatment of Nicotine Addiction
- Combination of counseling and pharmacotherapy is more effective than either option alone
- The more intense the intervention, the better the outcome of abstinence.
Pharmacologic Options
- Patients attempting to quit smoking should always be encouraged to use effective medications unless they are contraindicated in specific populations e.g.
- Pregnant women, smokeless tobacco users, light smokers, adolescents.
- Two categories of pharmaceutical options:
Counselling
- Intensive intervention that lasts a minimum of 10 minutes
- Commonly conducted by nurses in various health-care settings
- Motivational Interviewing
- Directive and client-centred standard counselling techniques
- Stages of Change theory
Other options of treatment
- Hypnosis
- Herbal remedies
- Acupuncture
- Laser treatment
No clinical evidence to verify results from these treatments
Some clients/patients report that they are beneficial.
Model for treatment of tobacco use and dependence
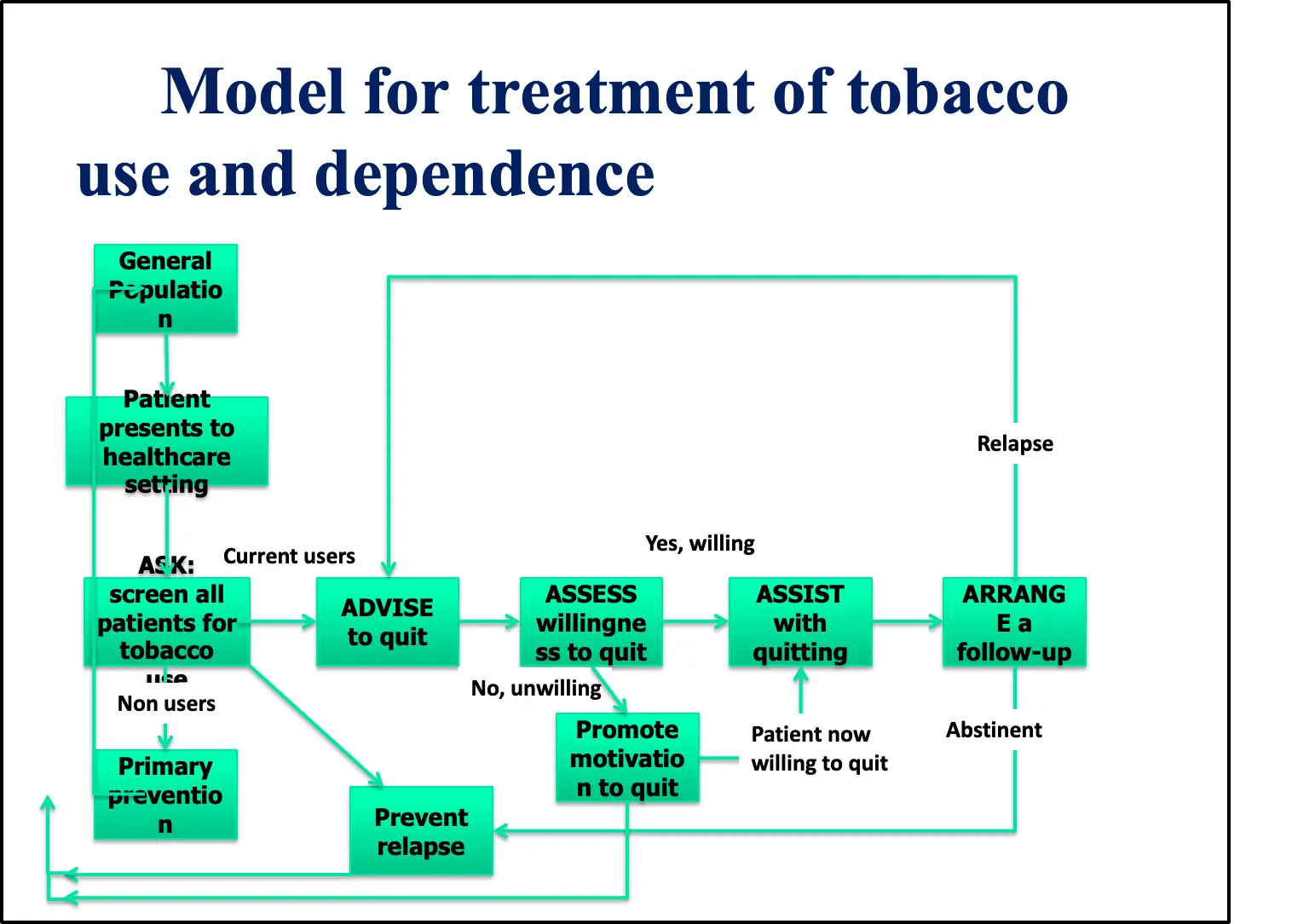 Source:
Tobacco Use and Dependence Guideline Panel. Treating Tobacco Use and Dependence: 2008 Update. Rockville (MD): US Department of Health and Human Services; 2008 May. Clinical Interventions for Tobacco Use and Dependence.
Source:
Tobacco Use and Dependence Guideline Panel. Treating Tobacco Use and Dependence: 2008 Update. Rockville (MD): US Department of Health and Human Services; 2008 May. Clinical Interventions for Tobacco Use and Dependence.
The 5 As Approach Z
- Ask about a patients’ smoking status.
- Advise those who smoke to stop.
- Assess their readiness to stop.
- Assist smokers in their stopping attempts.
- Arrange for follow-up on these attempts.
The following slides give a range of issues to bear in mind when you counsel patients to quit
5 as applies to Those who:
- Are willing to quit,
- Aren’t willing to quit, and
- Recently quit.
Smoking Cessation Treatment for Those Willing to Quit Z
- ASK Identify and document tobacco use status of every patient at every visit.
Example: When recording vital signs, include an area to note tobacco use.
ADVISE In a clear, strong, and personalized manner advise, every tobacco smoker to quit.
-
Advise examples:
- Clear: “I think it’s important for you to quit smoking now, and I can help you.”
- Strong: “As your clinician, I need you to know that quitting smoking now is the most important thing you can do to protect your health.”
- Personalized: “Continuing to smoke makes your asthma worse.”
-
ASSESS
- Is the user willing to make a quit attempt at this time?
- YES
- Provide assistance to dependence treatments.
- NO
- Provide an intervention shown to increase future quit attempts, such as nicotine gum, quit lines and behavioral counseling.
- YES
- Is the user willing to make a quit attempt at this time?
ASSIST
-
Offer medication. Provide or refer for counseling or additional behavioral treatment.
Medication examples:
- Nicotine lozenge
- Varenicline
Behavioral treatment examples:
- Recommend a quit plan, such as STAR.
- Set a quit date for ASAP.
- Tell family, friends and coworkers.
- Anticipate challenges.
- Remove tobacco products.
ARRANGE
- Arrange for follow-up soon after quit date, a second follow-up within the first month and others as needed.
- Identify problems and anticipate challenges.
- Remind patients of available sources, such as quit lines.
- Provide encouragement.
Smoking Cessation Treatment for Those NOT Willing to Quit Y
ASK, ADVISE & ASSESS
- Use the same 5As for users unwilling to quit as those willing to quit.
ASSIST Provide motivational interventions designed to increase future quit attempts.
-
Motivational examples: The 5 Rs
- Relevance: Identify why it is personally relevant to get the patient to quit.
- Risks: Ask the patient to identify negative consequences of smoking.
- Rewards: Ask the patient to identify benefits of stopping.
- Roadblocks: Identify the patient’s barriers to success and how to approach them.
- Repetition: Repeat motivational interventions.
-
Motivational examples: Express empathy
- Use open-ended questions. How important do you think it is for you to quit?
- Use reflective listening. “So you think smoking helps you maintain your weight.”
- Normalize patient’s feelings. “Many people worry about managing without cigarettes.”
- Support their right to choose. “I’m here to help you when you are ready.”
-
Motivational examples: Develop discrepancy
- Highlight the discrepancy between the patient’s smoking versus the patient’s stated values.
“You’re devoted to your family. How do you think your smoking affects them?” - Reinforce change talk.
“So, you realize how smoking is making it hard to keep up with your kids.” - Deepen the commitment to change
“We would like to help you avoid a stroke like the one your father had.”
- Highlight the discrepancy between the patient’s smoking versus the patient’s stated values.
-
Motivational examples: Roll with resistance
- Back off and use reflection.
- “Sounds like you’re feeling pressured about your tobacco use.”
- Express empathy.
- “I understand it’s hard to quit.”
- Ask permission to provide information.
- “Would you like to hear about some strategies that can help you quit?”
- Back off and use reflection.
-
Motivational examples: Support self-efficacy
- Help patients build on past successes.
- “You were fairly successful last time you tried to quit.”
- Offer options for small, achievable steps toward change.
- “Can you try smoking one less cigarette a day? A quit line can help you.”
- Help patients build on past successes.
ARRANGE
- More than one motivational intervention may be needed.
- Provide follow-up at the next visit.
- Offer additional interventions to motivate and support.
Treatment for Those Who Recently Quit
ASK
- Determine if the smoker is still smoke-free. then,
ASSESS
-
Relapse potential.
-
Most relapses occur within the first two weeks, but the risk can persist for a long time; therefore,
- Identify and address challenges, including
- lack of support for cessation,
- negative mood or depression,
- strong or prolonged withdrawal symptoms,
- weight gain and
- smoking lapses.
- Identify and address challenges, including
ASSIST
- Provide encouragement and relapse prevention to address the challenges of staying smoke-free.
- Challenge example
- Lack of support
- Depression
- Prevention response
- Schedule follow-ups, urge use of quit lines, identify source of support
- Counsel or refer to counseling/support groups.
- Challenge example
Smoking during Pregnancy Y
- Pregnancy is an optimal time for smoking cessation
- It is highly recommended for pregnant women using behavioral and social therapy
- If behavioral and social therapy are not possible then short-acting NRT
- The risk to the fetus of continued smoking by the mother far outweighs any potential side effects of NRT.
Smoking and Psychiatric Disorder Y
- Treating these patients is associated with reduced depression, anxiety, and stress
- Close monitoring is important
- Stopping smoking may exacerbate a patient’s condition.
- Offer tobacco dependence treatment when symptoms are not severe.
- NRT is safe and effective for smokers with a mental illness.
- Intensive counseling and close follow-up are important in such patients.
- Varenicline and bupropion can be used but with cautions
Stages of Change Z
- PRECONTEMPLATION
- ◦ Unaware or unwilling to change
- CONTEMPLATION
- ◦ Ambivalent, but thinking about changing
- PREPARATION
- ◦ Decided to change and taking steps
- ACTION
- ◦ Started to do things differently
- MAINTENANCE
- ◦ Changed for some time and integrating the change into their routine.
Prochaska and DiClemente
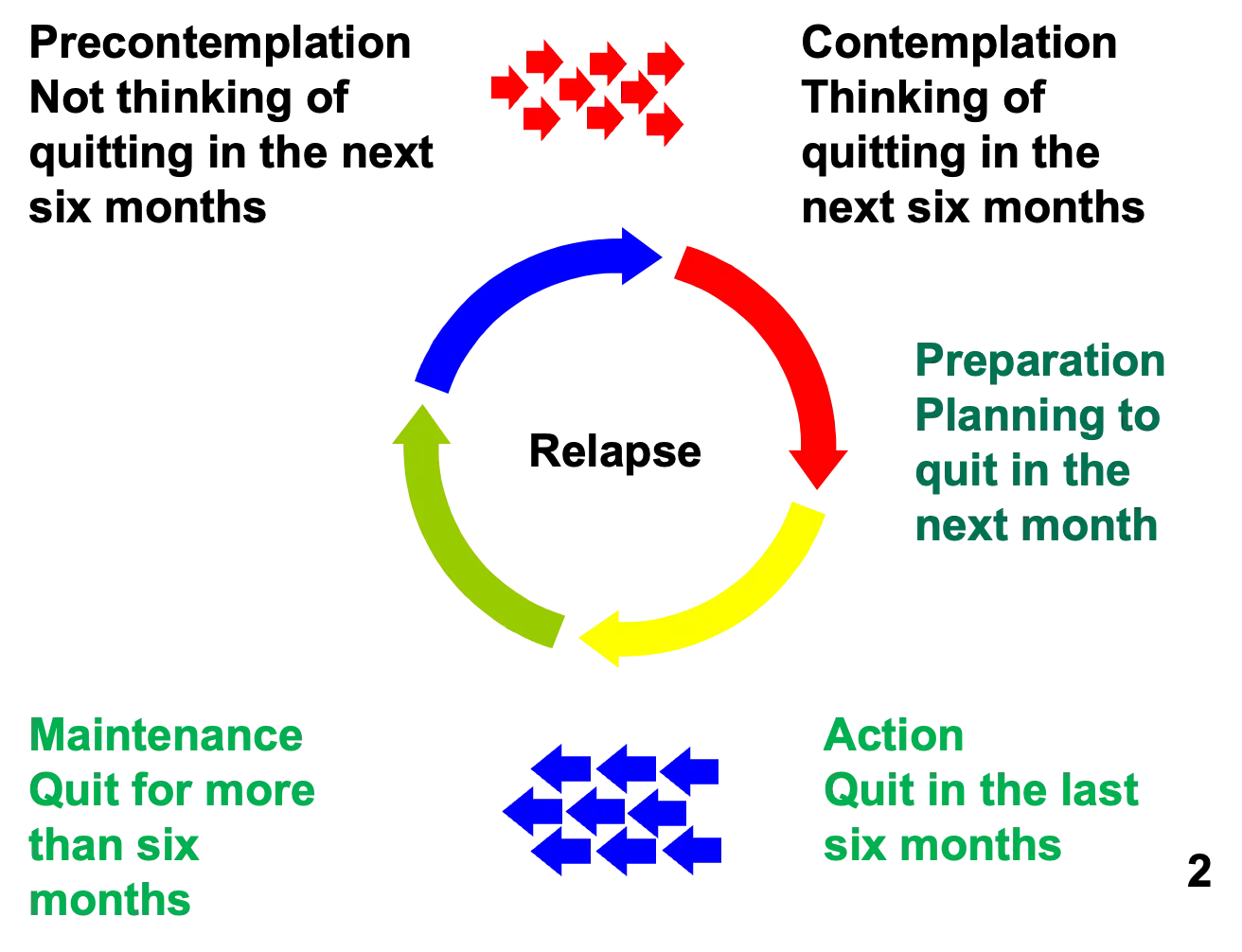 There is a broad range of research supporting a “stages-of-change” model for smoking cessation. These five stages include: precontemplation, contemplation, preparation, action and maintenance - with relapse as an element that can throw the smoker back to the beginning of the entire process. Most people begin in the precontemplation stage, as the small arrows leading to the circle imply, and the exit point for the successful smoker is from the maintenance stage. As we all know, this is a cyclical process and most smokers need several attempts to successfully manoeuvre through this process.
There is a broad range of research supporting a “stages-of-change” model for smoking cessation. These five stages include: precontemplation, contemplation, preparation, action and maintenance - with relapse as an element that can throw the smoker back to the beginning of the entire process. Most people begin in the precontemplation stage, as the small arrows leading to the circle imply, and the exit point for the successful smoker is from the maintenance stage. As we all know, this is a cyclical process and most smokers need several attempts to successfully manoeuvre through this process.
1. Pre-Contemplation
- In the pre-contemplation stage, clients may not recognize the consequences of their actions.
- In this stage, patients are typically not considering changing their behaviour. – Reasons might be ignorance or denial of problems.
- Intervention strategies include listening actively, expressing empathy, and accepting the client’s resistance rather than opposing it.
- Personalized tasks may include asking clients to reconsider their behaviour by analysing the risks of their actions and identifying any benefits of changing.
2. Contemplation
- Here clients acknowledge their problem, but may not have the confidence to take a step forward.
- Clues to recognizing clients in this stage include uncertainty, conflicted emotions, or ambivalence about changing.
- Instilling hope in the client’s ability to proceed is a crucial form of support in this stage.
- Interventions may include asking about a client’s beliefs to help gain a deeper understanding of their behaviour.
- Asking about possible barriers to change may also be helpful. Clients may gain a stronger sense of purpose by asking them to weigh the pros and cons of present behaviour as well as the pros and cons of changing.
3. Preparation
- Clients are willing to take small steps forward.
- Evidence of this stage may include statements confirming a client’s commitment to change and a willingness to prepare a plan of action.
- Setting small, achievable goals is critical for clients in this stage.
- Strategic tasks may include identifying resources, supports, and skills the client may draw on and then help the client create a plan to attain them.
- Encourage the client’s self-efficacy and commitment to change.
4. Action
- Clients in the action stage have developed clear plans for change and are implementing them.
- They are easily identified by their direct actions towards accomplishing their goals.
- The intervention strategies in this stage include periodic reviews of client motivations, resources, progress, and enthusiastically praising success.
5. Maintenance
- Clients enter the maintenance stage after adopting their new change for at least six months.
- Continuing more as a consultant, the counsellor provides advice, guidance, and support to clients in the maintenance stage only as needed.
- People typically remain in this stage for up to 5 years as confidence in sustaining their new lifestyle increases and fear of relapse decreases.
- Interventions during this stage may include helping clients recognize how overconfidence sometimes leads to relapse.
6. Relapse
- The unofficial 6th stage of change is relapse.
- Relapses are common in the process of making lifelong changes.
- Clients in this stage have lapsed back to old behaviour and are easily recognized by their frustration, disappointment, or feelings of failure.
- Intervention strategies and tasks include de-stigmatizing and normalizing the notion of relapse, helping the client identify the cause, and devising a plan to avoid this trigger in the future.
- The keys to success in the relapse stage are helping clients reassess their supports and skills and reaffirm their commitment to their goals.
Myths You May Encounter as You Work with Your Patients to Help Them Stop Smoking
-
Myth 1: Smoking is just a bad habit.
- Fact: Tobacco use is an addiction.
- Nicotine is a very addictive drug. For some people, it can be as addictive as heroin or cocaine.
- Fact: Tobacco use is an addiction.
-
Myth 2: Quitting is just a matter of willpower.
- Fact: Because smoking is an addiction, quitting is often very difficult. A number of treatments are available that can help.
-
Myth 3: If you can’t quit the first time you try, you will never be able to quit.
- Fact: Quitting is hard. Usually, people make two or three tries, or more, before being able to quit for good.
-
Myth 4: The best way to quit is “cold turkey.”
- Fact: The most effective way to quit smoking is by using a combination of counseling and nicotine replacement therapy (such as the nicotine patch, inhaler, gum, or nasal spray) or non-nicotine medicines (such as bupropion SR).
-
Myth 5: Quitting is expensive.
- Fact: Treatments cost from 10 a day. A pack-a-day smoker spends almost $1,000 per year. Check with your health insurance plan to find out if smoking cessation medications and/or counseling are covered.