Primary Prevention
-
LDL-C
≥190 mg/dL -
Diabetes
LDL-C 70–189 mg/dL
Age 40–75 y -
≥7.5% estimated 10-y ASCVD risk
and age 40–75 y
 <20 years only treat if familial dyslipidaemia
20-40 years Consider treat if LDL ≥4.1 (160) + FH premature ASCVD
<20 years only treat if familial dyslipidaemia
20-40 years Consider treat if LDL ≥4.1 (160) + FH premature ASCVD
40 - 75/85yrs we calculate the 10 year risk ASCVD , but if DM give statin. ( ≥85 years NICE) (≥75 ACC) no need to calculate risk just assess clinically the need and discuss
Guidelines for Primary Prevention
Lifestyle Changes for Preventing Cardiovascular Disease
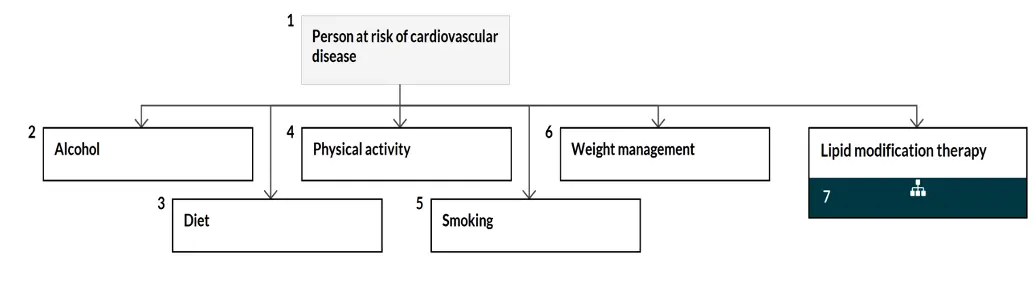
- Person at risk of cardiovascular disease
- Alcohol
- Diet
- Physical activity
- Smoking
- Weight management
- Lipid modification therapy
Diet Therapy
- I LOST 1 KG THIS WEEK
- TIME TO REWARD MYSELF!

Diet Therapy
(Always initiated firstly in the management. Except patients with familial hypercholesterolemia and Statin benefit group in which both drugs and diet should begin together.)
- Total fat restriction → ↓hypertriglyceridemia
- Cholesterol & Saturated fat → ↓Hypercholesterolemia (LDL)
- Decrease CHO (Sucrose & simple sugars) → ↓VLDL.
- Increase dietary fibers (oat or rice bran) → ↓LDL
American Heart Association
- Increase vegetables, fresh fruit, cereals, whole grain.
- No alcohol → ↓ Hypertriglyceridemia
- Decrease caloric intake and stabilization of weight.
- Total fat calories should be 20-25% with saturated fat < 8%.

Exercise
- Aerobic physical activity
- Minimum 3-4 sessions per week
- Lasting on average 40 minutes per session
- Involving moderate-to-vigorous intensity physical activity.
- ▼TG, ▼VLDL-C, and ▲HDL-C
Effect of Impact Exercise on Cholesterol levels 12-month follow-up

Modrate: Brisk walking (2.4-4mile per hour), bikng (5-9 mph), active yoga, recreational swimming.
Vigorous: Jogging/ running, biking (>10mph), swimming labs, single tennis
Dyslipidemia Management
Weight Loss
- Weight loss improves the plasma lipoprotein profile.
- Reductions in LDL-C and VLDL-C
- Management options:
We recommend adjunctive pharmacotherapy for weight loss and weight-loss maintenance for individuals with BMI ≥ 30 kg/m2 or BMI ≥ 27 kg/m2 with adiposity-related complications, to support medical nutrition therapy, physical activity and psychological interventions. Options include liraglutide 3.0 mg, naltrexone-bupropion combination and orlistat.
Figure 12: BMI and lipid risk factors for men in the Framingham Offspring Study.


Recommendation
- Assess ASCVD Risk in Each Age Group
- Emphasize Adherence to Healthy Lifestyle
Age 0-19 y
- Lifestyle to prevent or reduce ASCVD risk
- Diagnosis of Familial Hypercholesterolemia → statin
Age 20-39 y
- Estimate lifetime risk to encourage lifestyle to reduce ASCVD risk
- Consider statin if family history of premature ASCVD and LDL-C ≥160 mg/dL (≥4.1 mmol/L)
Age 40-75 y and LDL-C ≥70-<190 mg/dL (≥1.8-<4.9 mmol/L) without diabetes mellitus
- 10-year ASCVD risk percent begins risk discussion
Risk Calculation
-
LDL-C ≥190 mg/dL (≥4.9 mmol/L)
- No risk assessment; High-intensity statin (Class I)
-
Diabetes mellitus and age 40-75 y
- Moderate-intensity statin (Class I)
-
Diabetes mellitus and age 40-75 y
- Risk assessment to consider high-intensity statin (Class IIa)
Age >75 y
- Clinical assessment, Risk discussion

<20 years only treat if familial dyslipidaemia
20-40 years Consider treat if LDL ≥4.1 (160) + high lifetime ASCVD risk / FH premature ASCVD
We treat 40-75/85 we calculate the 10 year risk ASCVD percent and act accordingly.
( ≥85 years NICE) (≥75 ACC) no need to calculate risk just assess clinically the need and discuss
Pooled Cohort Equation
 US: ASCVD Risk Score Calculator:
http://tools.acc.org/ASCVD-Risk-Estimator-Plus/#!/calculate/estimate/
US: ASCVD Risk Score Calculator:
http://tools.acc.org/ASCVD-Risk-Estimator-Plus/#!/calculate/estimate/