IM
INVESTIGATIONS
In uncomplicated ulcers, basic investigations like CBC and chemistry are usually normal ( Hb may be low in bleeding ulcers)
The 2 “specific” investigations in peptic ulcer patients are:
- Endoscopy (confirms ulcer)
- H. Pylori testing (Barium studies are no longer done)
ENDOSCOPY
- It is the best investigation to diagnose ulcers
- During endoscopy, biopsy of the ulcer is always taken and sent for H. Pylori testing(CLO TEST)
- In case of gastric ulcer, biopsy is also sent to rule out carcinoma(some gastric ulcers can be malignant)
- DU are never malignant.
Endoscopic views
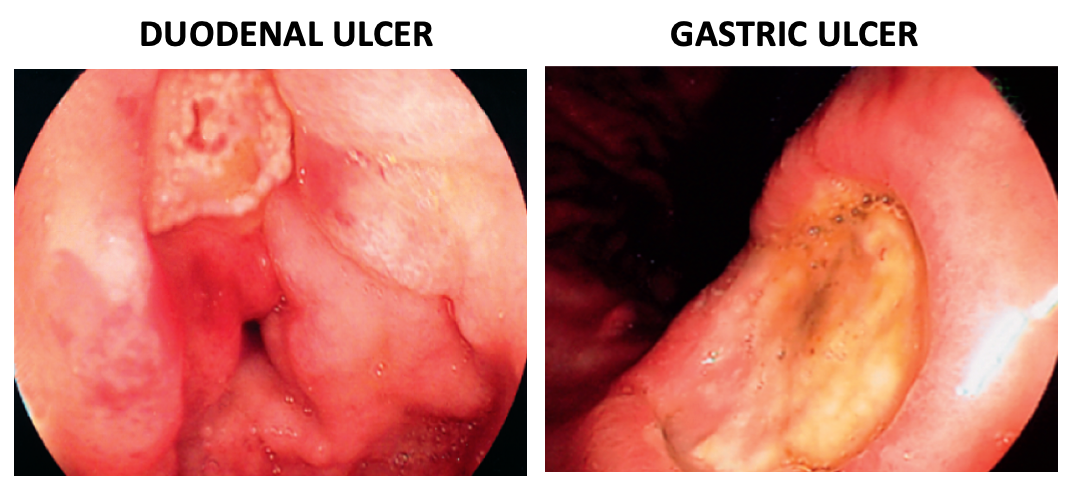
H. Pylori testing
4 commonly used methods of detecting H. Pylori:
- Urea breath test (most frequently used with 95% sensitivity)
- Stool antigen test (most frequently used with 95% sensitivity)
- CLO test (after biopsy)
- Serum antibody titers ⇒ (very frequently used but low specificity. Can be done if 1,2 & 3 are not available)
Before understanding the urea breath test and CLO test , remember the following: H. Pylori produces the enzyme “ urease” which can split urea into NH3( ammonia ) and CO2
urease
UREA --> NH3 + CO2
- Urea breath test:
- Pt. ingests urea tablets which contain C₁₄
- H. Pylori urease splits urea into NH3 & CO2
- CO2 (which contains C14) is exhaled through the lungs and collected in a bag
- Results are very quick ( 15 min)
Tablets & bag ( full kit)
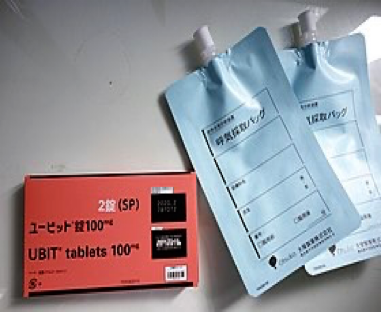
2) Stool Antigen test: H. Pylori antigens are checked in the stool.
3) CLO test ( rapid urease test):
- Biopsy of the ulcer taken during endoscopy
- Sample is placed in a solution which contains urea
- Urease of H. Pylori splits urea & releases NH3 → color of the solution changes
Before doing 1, 2 and 3, stop PPIs for 14 days
Surgery
Diagnosis :
-
Endoscopy—This has replaced Ba–meal examination as the mainstay of diagnosis. In addition to confirming the presence of peptic ulceration, endoscopy allows esophageal disease to be excluded, may reveal unsuspected pathology and allows gastric ulcers to be biopsied to exclude malignancy.
-
USG—This is advisable to exclude gallstones as cholelithiasis and peptic ulceration often coexist and share common symptoms.
Differential Diagnosis
- Chronic gastric ulcer.
- Chronic cholecystitis.
- Chronic amebiasis and worm infestation.
- Chronic pancreatitis.
- Chronic appendicitis.
- Intestinal tuberculosis.
FM
Diagnosis of Peptic Ulcer Disease
- Endoscopy is the preferred investigation
- Gastric ulcers may occasionally be malignant and therefore must always be biopsied
- Patients should also be screened for H. pylori infection
- Some are invasive and require endoscopy; others are non-invasive
- Overall, breath tests are best because of their accuracy, simplicity, and non-invasiveness
Endoscopy
Considered if:
- ALARM signals and signs are the major determinant of the need for endoscopy, not age on its own.
- No response to medication in 7-10 days.
- Symptoms persist after 6-8 weeks.
- Signs of systemic illness.
- Recurrence after treatment.
- Long-standing GORD.
Age Consideration
- In patients aged 55 years and older with unexplained and persistent recent onset dyspepsia alone, an urgent referral for endoscopy should be made.
Urgent Referral for Endoscopy
Indicated for patients with dyspepsia of any age with any of the following conditions:
Symptoms Z
- Chronic gastrointestinal bleeding
- Progressive unintentional weight loss
- Progressive difficulty swallowing
- Persistent vomiting
- Iron deficiency anaemia
- Epigastric mass
- Suspicious barium meal.
Endoscopy Preparation
Patients undergoing endoscopy should be free from medication with either a PPI or an H2 receptor antagonist for a minimum of two weeks.
H. Pylori Testing
- Serology
- Urea Breath test Z
- Fecal antigen test
- Endoscopy
- Strip test
Assessment of Dyspepsia
New Onset Dyspepsia
-
Age <60
- No alarm features
- Alarm features (see text)
- Breath or stool test for H. pylori
- Positive
- Antimicrobial therapy
- Improvement
- No improvement
- Tricyclic antidepressant (trial for 8-12 weeks) or prokinetic (trial for 4-8 weeks)
- Improvement
- No improvement
- Consider further workup or psychotherapy
- Tricyclic antidepressant (trial for 8-12 weeks) or prokinetic (trial for 4-8 weeks)
- Antimicrobial therapy
- Positive
- Breath or stool test for H. pylori
-
Age ≥60
- Endoscopy
- Breath or stool test for H. pylori
- Negative
- Proton pump inhibitor (trial for 4-8 weeks)
- Improvement
- No improvement
- Proton pump inhibitor (trial for 4-8 weeks)
- Negative
- Breath or stool test for H. pylori
- Endoscopy
Therapeutics
Investigations:
1- Laboratory findings:
- Microcytic hypochromic anemia may occur with blood loss from a bleeding ulcer.
- Leukocytosis suggests ulcer penetration or perforation.
- An elevated serum amylase in a patient with severe epigastric pain suggests ulcer penetration into the pancreas.
- A fasting serum gastrin level to screen for Zollinger-Ellison syndrome is needed in some patients with recurrent intractable ulcers .
2-Endoscopy:
-
Upper endoscopy is the procedure of choice for the diagnosis.
-
Duodenal ulcers are virtually never malignant and do not require biopsy. However, biopsies of gastric ulcers are performed to rule out malignancy.
•Imaging: Barium upper gastrointestinal series has limited accuracy .
•Testing for H pylori: (Discussed previously)
Diagnosis:
A. Noninvasive testing for H. pylori:
-
Serologic ELISA tests have sensitivity and specificity of over 90%. Positive serologic tests do not necessarily imply ongoing active infection. After H. pylori eradication with antibiotics, antibody levels decline to undetectable levels in 50% of patients by 12-18 months.
-
A fecal antigen immunoassay has excellent sensitivity and specificity (90%). A positive test is indicative of active infection Z
-
The 13C-urea and 14C-urea breath tests also have excellent sensitivity and specificity (90%), and a positive test is indicative of active infection. However, their greater cost makes them less attractive than other noninvasive tests in most clinical settings.
B. Endoscopic testing for H. pylori: Endoscopically obtained gastric biopsy specimens can be obtained for detection of H pylori by testing for urease production.
Histologic assessment of biopsies from the gastric antrum and body is more definitive.