Routine Assessments Include
-
Maternal status / wellbeing
- General health (physical and emotional)
- Blood pressure
-
Weight
-
Nutritional counselling
- Calculate a woman’s BMI at the first antenatal visit.


- Calculate a woman’s BMI at the first antenatal visit.
| Category | Pre-pregnancy BMI (kg/m²) | Weight gain (kg) | Rates of weight gain 2nd & 3rd trimester (kg/week) |
|---|---|---|---|
| Underweight | <18.5 | 12.6-18 | 0.45 (0.45-0.6) |
| Normal weight | 18.5 – 24.9 | 11.3-15.8 | 0.45 (0.36-0.45) |
| Overweight | 25.0 – 29.9 | 6.8-11.3 | 0.27 (0.23-0.32) |
| Obese (all classes) | ≥30 | 5-9 | 0.23 (0.18-0.27) |
Calculations assume 0.5–2 kg weight gain in the 1st trimester.
Fetal Status / Wellbeing
- Abdominal examination (size, shape indicates gestation of the pregnancy)
- Kick chart / fetal movement chart
- Fetal heart rate.

Assessing the Position of the Fetus
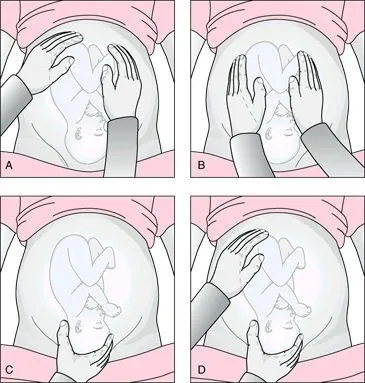
Disease Detection
- Look for problems requiring additional care
| Parameter | Condition |
|---|---|
| Skin, general appearance, night blindness, goiter | Malnutrition |
| Temperature, dysuria | Signs of infection |
| Blood pressure, edema, proteinuria, reflexes | Signs of pre-eclampsia |
| Hemoglobin, conjunctiva/palms/tongue pallor | Signs of anemia |
| Breast exam | Breast disease |
| Baby’s movements, fundal height, baby’s heart beat | Fetal distress/demise |
| Pelvic and speculum exam | Sexually transmitted diseases |
When to Contact Your Doctor?
- Vaginal bleeding
- Premature labour
- Rupture of the membranes
- Decreased fetal movements
- Severe headaches, visual blurring or
- Spotting of vision
Antenatal Visits
Traditional antenatal care includes a series of between 7 and 11 visits; however, the number of visits necessary for adequate care is disputed.
- The typical frequency of visits in an uncomplicated pregnancy is as follows:
- Every 4 weeks for the first 28 weeks
- Every 2 to 3 weeks between 28 and 36 weeks
- Weekly after 36 weeks.
Antenatal Care Guidelines
-
Typical visits include evaluation of BP, weight, urine for protein levels, and checking the fetal heart rate. Psychosocial screening at least once each trimester.
-
It is recommended that pregnant women initiate antenatal care by 10 to 12 weeks’ gestation.
-
The first antenatal visit should include a comprehensive history, laboratory work, and education about pregnancy health. Height and weight should be recorded to calculate BMI.
-
At the first antenatal visit, all pregnant women should also have a blood test to check FBC, ABO blood group, Rh D status, and the presence of erythrocyte antibodies.
-
Screening for depression, which is common during pregnancy and in the first 12 months after delivery, may be beneficial.
Dietary and Physical Activity Recommendations in Pregnancy
-
Diet and physical activity-based interventions in pregnancy are beneficial and can reduce gestational weight gain, as well as the rate of caesarean delivery.
-
Daily antenatal vitamins containing folate (400-800 micrograms/day) are recommended as tolerated throughout pregnancy, and at least through the first 3 months of pregnancy.
- Alcohol consumption is contraindicated in pregnancy.
Education
- Consider these specific issues:
- ◊ Smoking
- ◊ Substance misuse
- ◊ Working
- ◊ Air travel: women with uncomplicated pregnancies can fly safely until 36 weeks’ gestation. Z fitness to flight
- ◊ Exercise
Childbirth Education
- Relative risks and benefits of home versus hospital birth
- Labour and delivery
- Pain relief options
- Potential obstetric complications and procedures
- Normal newborn care
- Postnatal adjustment
Breastfeeding
Miscellaneous
- Other educational issues to discuss include:
- Dental care
- Nutrition
- Wearing a seat belt
- Sleep position
- Sexual activity
- Postnatal contraception
- Circumcision of male infants
Routine Testing
- Full blood count (FBC)
- ABO blood group, Rhesus status, presence of erythrocyte antibodies
- Rubella status, hepatitis B screening
- Screening for STIs (syphilis, HIV, gonorrhoea, and chlamydia)
- Urine dipstick and culture
- BP measurement, gestational diabetes screening
- Check of last cervical screening, and
- Ultrasound
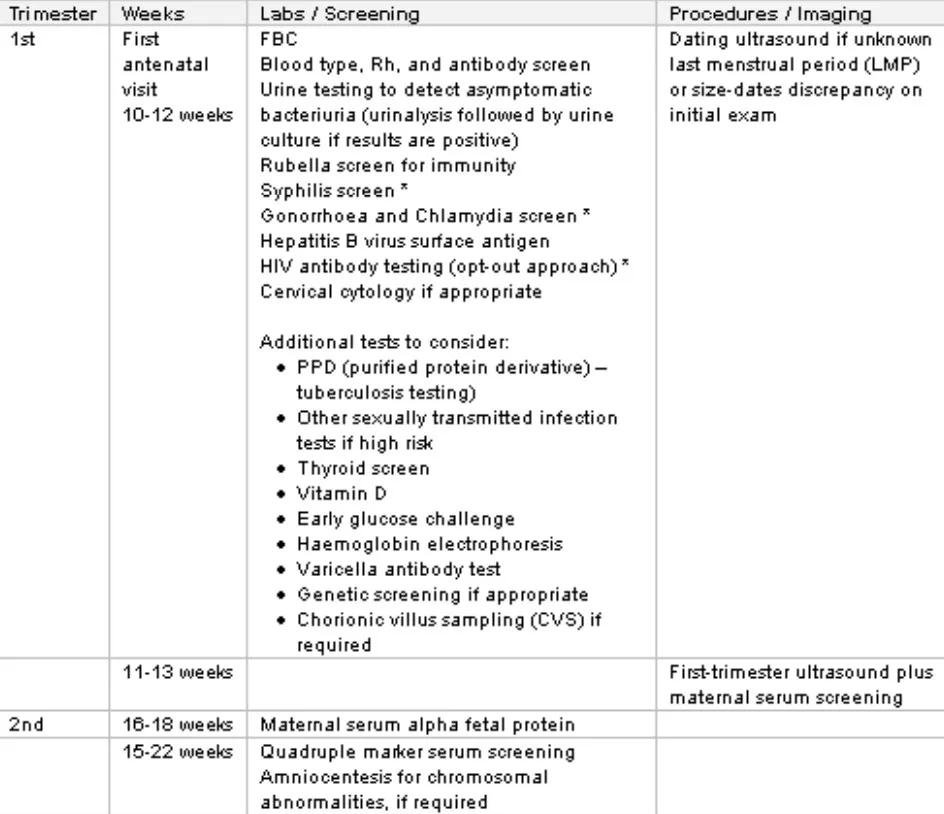 28w Z anti-d immunoglobulin if needed
28w Z anti-d immunoglobulin if needed

Ultrasonography
-
First-trimester ultrasound screening is optimal for pregnancy dating.
- Between 11+2 weeks and 14+1 weeks’ gestation.
-
Advantages of first-trimester ultrasonography include its ability to help determine the presence of an intrauterine pregnancy, gestational age, and evaluate for multiple gestation.
-
An ultrasound examination performed in the second-trimester is optimal for a survey of the fetal anatomy and placental location, between 18 and 22 weeks’ gestation.
-
Obese patients should be informed that their fetus is at increased risk for congenital anomalies, including undiagnosed anomalies. Sonographic fetal anatomical assessment may be better performed at 20 to 22 weeks in obese patients.
Placenta Praevia Information
-
Routine second-trimester ultrasound examination will reveal placental location and relationship to the internal cervical os. Placenta praevia complicates 0.3% to 0.5% of pregnancies.
-
The majority (>80%) of praevia cases diagnosed at 20 weeks’ gestation resolve by term. Thus, a follow-up ultrasound in the third-trimester, usually around 32 weeks’ gestation, is warranted.
-
In women with a persistent low-lying placenta or placenta praevia at 32 weeks’ gestation, a further ultrasound should be arranged at 36 weeks.
WHO Recommendations on ANC
49 recommendations were grouped into five topic areas:
- A. Nutritional interventions (14)
- B. Maternal and fetal assessment (13)
- C. Preventive measures (7)
- D. Interventions for common physiological symptoms (6)
- E. Health systems interventions to improve the utilization and quality of ANC (9)