FM
Management
Individualised Care Z
Take an individualised approach to management that is tailored to the specific needs and circumstances of your patient. Take into account the patient’s:
- Personal preferences Z
- Comorbidities
- Risks from polypharmacy
- Ability to benefit from long-term interventions because of reduced life expectancy
- Disabilities (e.g., visual impairment).
Diet, Physical Activity, and Sleep
Nutritional advice should be tailored to the needs of the individual patient, and be provided by a healthcare professional with specific expertise and competencies in nutrition.
Encourage the patient to: Z
- Include high-fibre, low-glycaemic-index sources of carbohydrate in their diet, such as fruit, vegetables, wholegrains, and pulses.
- Eat low-fat dairy products and oily fish.
- Limit their intake of foods containing saturated and trans fatty acids.
In terms of physical activity, encourage the patient to: Z
- Reduce sedentary behaviour and be more physically active.
- Incorporate activity into their daily life (e.g., brisk walking, gardening, cycling). In this way, the patient can gradually increase the amount and intensity of activity they do.
- Do at least 30 minutes of moderate (or greater intensity) physical activity on 5 or more days a week.
If the patient is overweight, set an initial body weight loss target of 5% to 10%. Z Evidence suggests this is the minimum weight loss in obese patients to improve glycaemic control, lipid levels, and blood pressure.
Cardiovascular Risk Management
Blood Pressure (BP)
The National Institute for Health and Care Excellence (NICE) in the UK recommends maintaining blood pressure at:
- Below 135/85 mmHg for adults aged under 80, based on ambulatory or home BP monitoring (or <140/90 mmHg based on clinic BP).
- Below 145/85 mmHg for patients aged 80 and over, based on ambulatory or home BP monitoring (or <150/90 mmHg based on clinic BP).
///
Lipids
Based on these categories, the ESC recommends in patients with type 2 diabetes who are:
- At moderate cardiovascular risk: an LDL-cholesterol target of <2.6 mmol/L (<100 mg/dL).
- At high cardiovascular risk: an LDL-cholesterol target of <1.8 mmol/L (<70 mg/dL) and LDL-cholesterol reduction of at least 50%; a secondary goal of a non-HDL-cholesterol target of <2.6 mmol/L (<100 mg/dL).
- At very high cardiovascular risk: an LDL-cholesterol target of <1.4 mmol/L (<55 mg/dL) and LDL-cholesterol reduction of at least 50%; a secondary goal of a non-HDL-cholesterol target of <2.2 mmol/L (<85 mg/dL).
Antiplatelets
- Chronic kidney disease
Antihyperglycemic Medications
In the UK, NICE recommends:
- If the patient manages their type 2 diabetes either with lifestyle and diet, or with lifestyle and diet combined with a single drug that is not associated with hypoglycaemia, support them to aim for an HbA1c level of 48 mmol/mol (6.5%).
- If the patient is on a drug associated with hypoglycaemia, support them to aim for an HbA1c level of 53 mmol/mol (7.0%).
Consider a slightly higher HbA1c level on a case-by-case basis for:
- Patients who are older, frail, or unlikely to achieve longer-term risk-reduction benefits (e.g., those with a reduced life expectancy).
- Patients for whom tight blood glucose control poses a high risk of the consequences of hypoglycaemia, including: people who are at risk of falling; people who have impaired awareness of hypoglycaemia; those who drive or operate machinery as part of their job.
- Patients for whom intensive management is not appropriate (e.g., people with significant comorbidities).
Medication Classes
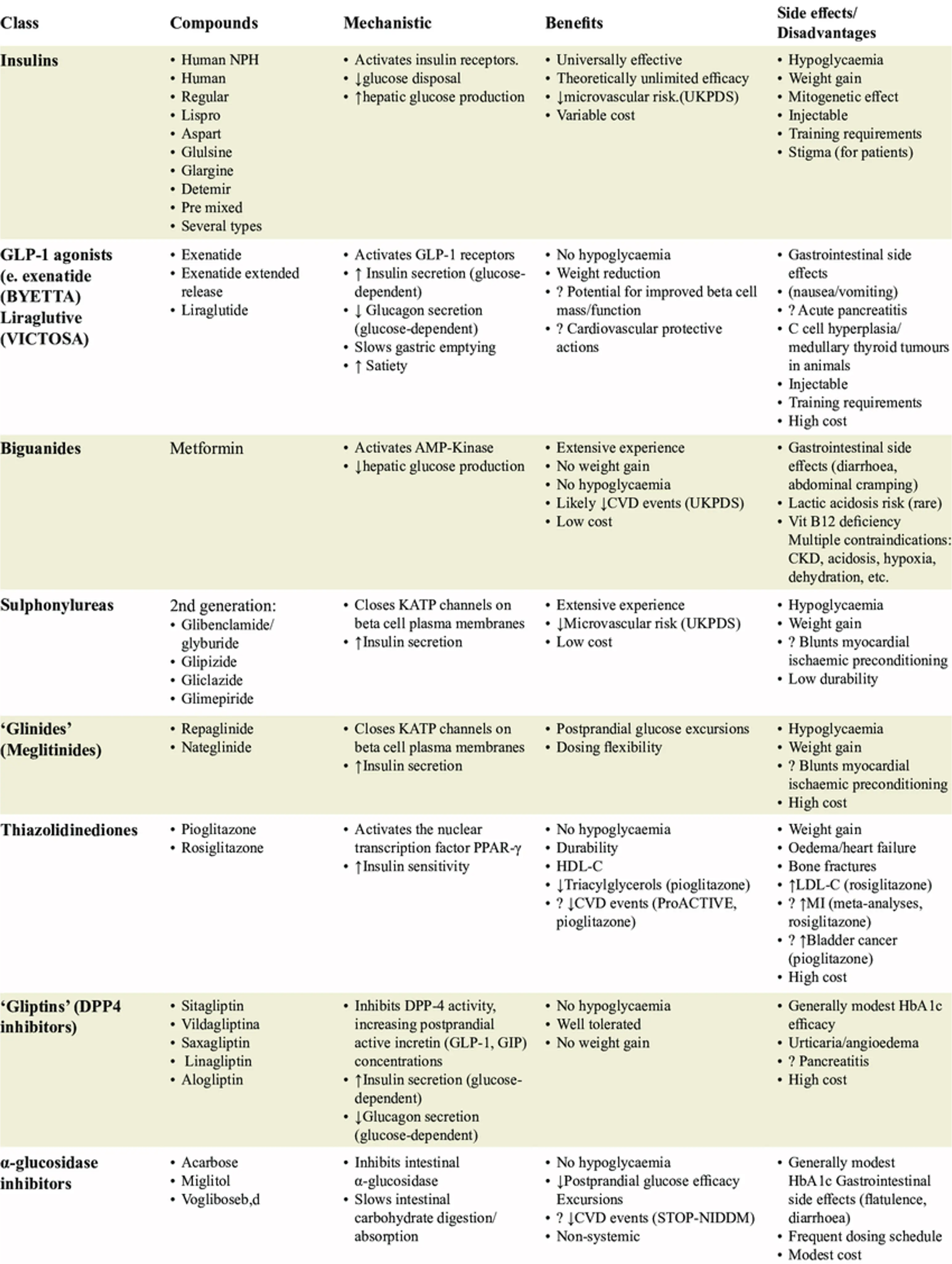
Management
Prevention and Managing Complications
- Macrovascular
- Microvascular
metformin drug of choice to DM2 Z sulphonylureas
Glucagon like peptide GLP SGL - kidney disease
insulin used when hba1c >9%
overweight want to lose weight doesnt want use insulin, used metformin sulph not controlled, we’d give glucagon like peptide
Therapeutic
Main Types treatments of Acute complication:
- Hypoglycemic coma.
- Diabetic keto-acidosis (DKA).
- Hyperosmolar hyperglycemic state (HHS)
- Hyperosmolar non-ketotic coma (HONK).
- Lactic acidosis (rare).
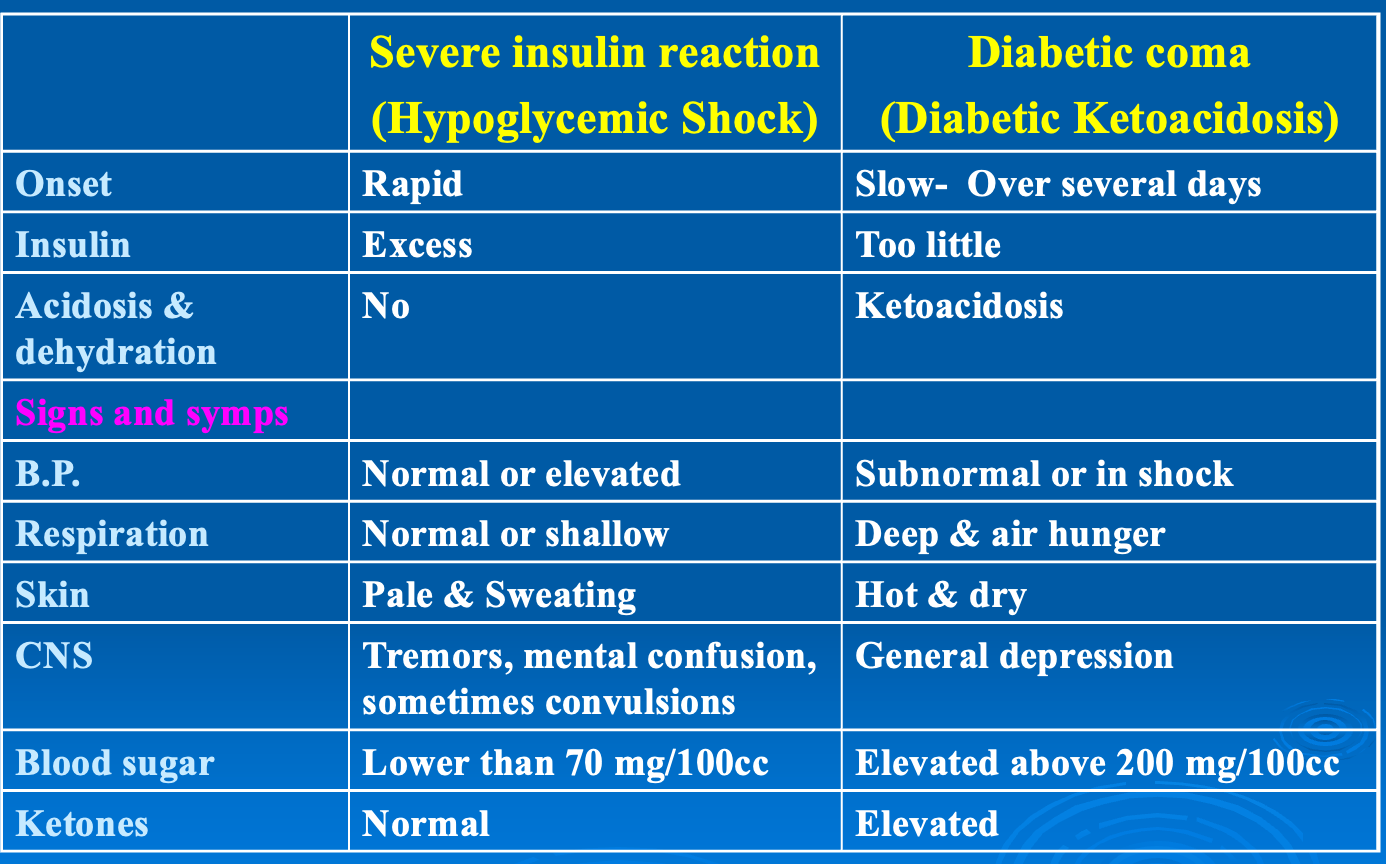
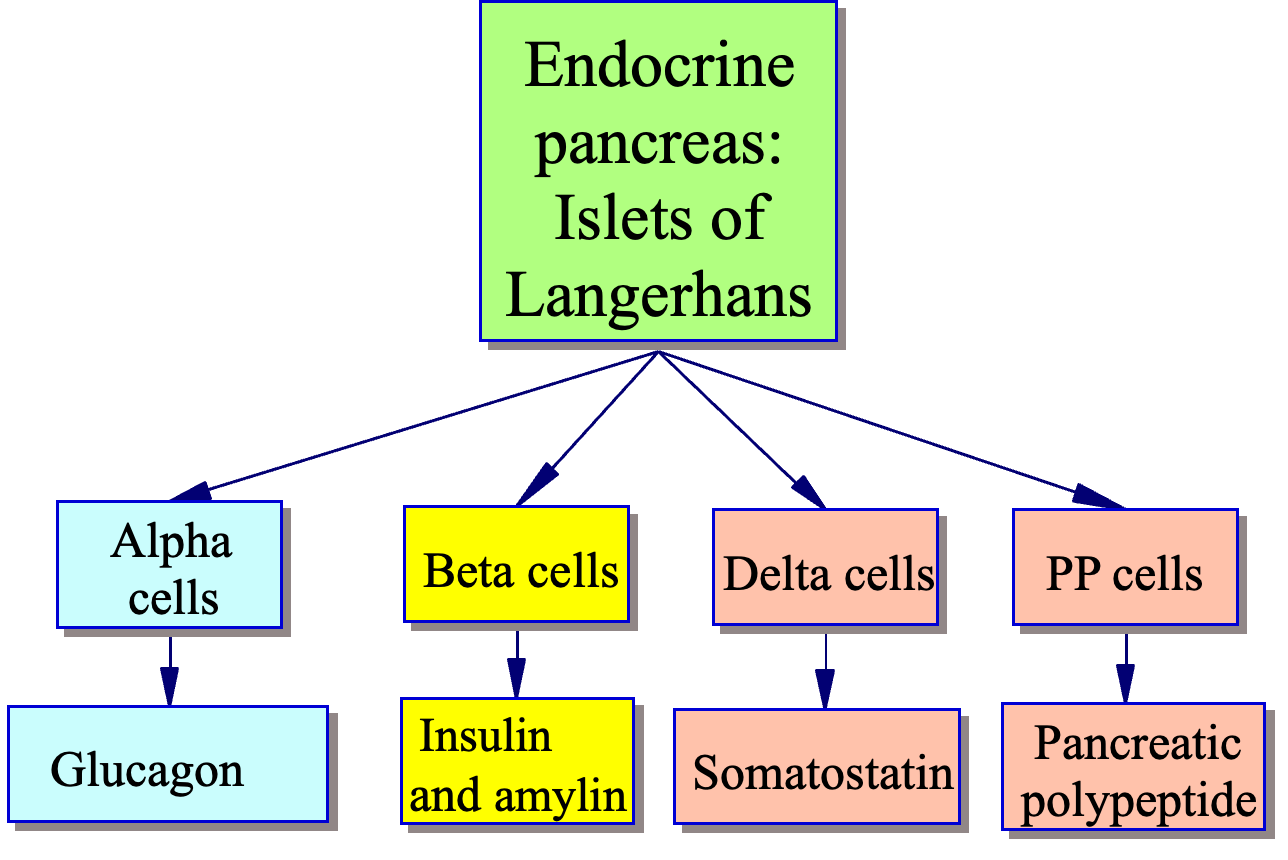
Treatment
- Life-style modification: e.g.
- Diet: should have low glycemic index (i.e. ↑ vegetables and ↓ CHO).
- Weight reduction.
- Encourage physical exercise.
- Correction of the precipitating factors: e.g. infection.
- Metformin: it ↓hepatic output of glucose and ↓ intestinal glucose absorption so it ↓ plasma insulin levels.
- Insulin sensitizers e.g. pioglitazone or sulphonylureas to ↑ insulin receptors sensitivity.
- Small dose of fluorinated corticosteroids e.g dexamethazone : because it has anti-immunological effect e little or no hyperglycemic effect.
- In case of local insulin resistance: -Change the site of injection regularly. -Give aprotinin (trasylol) with insulin at the injection site to inhibit the proteolytic enzymes.
Counter regulatory Hormones
They counteract the storage functions of insulin in regulating blood glucose levels during periods of fasting, exercise, and other situations that either limit glucose intake or deplete glucose stores.
- The catecholamines,
- Growth hormone, and Thyroid Hormone
- Glucagon, Glucocorticoids.
Mechanism of Glucose Stimulated Insulin Secretion
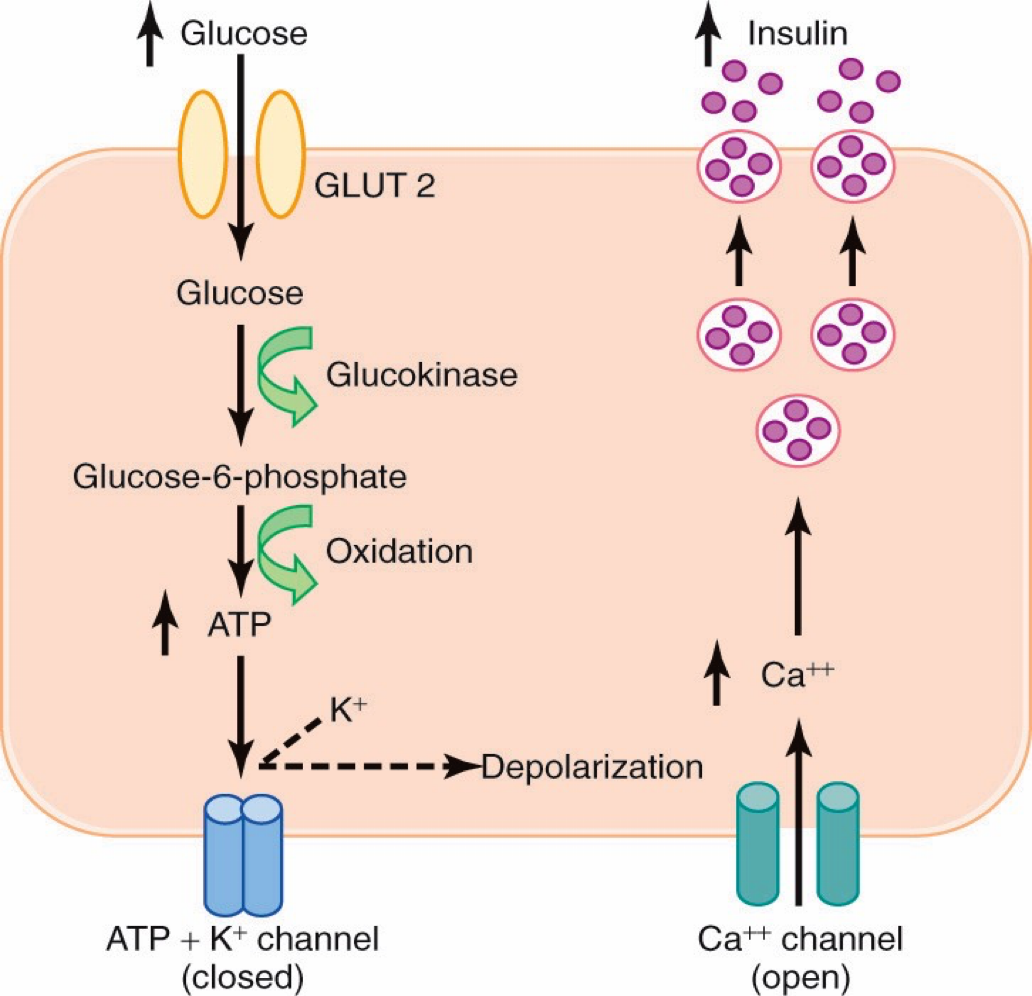
| Function | Cell Type | Description |
|---|---|---|
| Insulin Secretion | Beta Cells (70-80%) | Produce and secrete insulin to regulate blood sugar levels |
| Glucagon Secretion | Alpha Cells (15-20%) | Produce and secrete glucagon to raise blood sugar levels |
| Somatostatin Secretion | Delta Cells (5-10%) | Inhibit insulin secretion and glucagon release to regulate blood sugar levels |
| Pancreatic Polypeptide Secretion | PP Cells (1-2%) | Regulate pancreatic secretions and gut motility |
| Regulation of Blood Sugar Levels | All Islet Cell Types | Maintain blood sugar levels within a narrow range (70-110 mg/dL) |
| Feedback Regulation | All Islet Cell Types | Adjust secretory activity based on changing glucose levels |
| Autoregulation | Beta Cells | Regulate their own function through autocrine and paracrine mechanisms |
| Inflammation Regulation | All Islet Cell Types | Produce cytokines to regulate inflammation in response to immune challenges or tissue damage |
| Tissue Remodeling | All Islet Cell Types | Participate in angiogenesis, fibrosis, and other processes that maintain pancreatic structure and function |
| Hormone Regulation | All Islet Cell Types | Regulate the secretion of other hormones, such as growth hormone |